renal dialysis

Figure 1. Patient receiving hemodialysis
Image source: Fresenius Medical Care Deutschland GmbH.
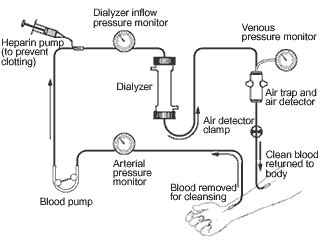
Figure 2. Hemodialysis.
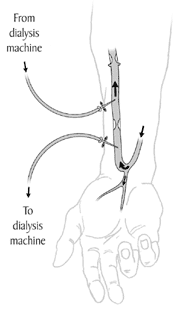
Figure 3. Arteriovenous fistula.
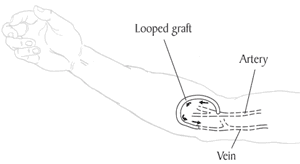
Figure 4. Looped graft.
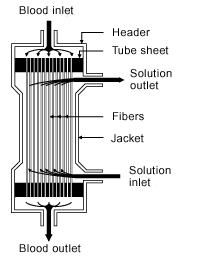
Figure 5. Hollow fiber dialyzer.
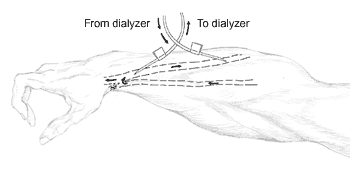
Figure 6. Arterial and venous needles.
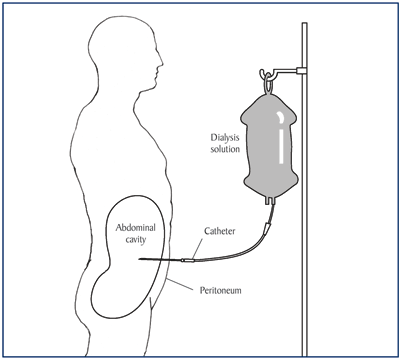
Figure 7. Peritoneal dialysis.
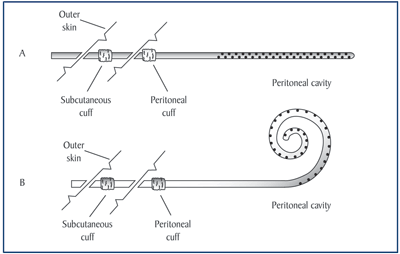
Figure 8. Double-cuff Tenckhoff peritoneal catheters: standard (A), curled (B).
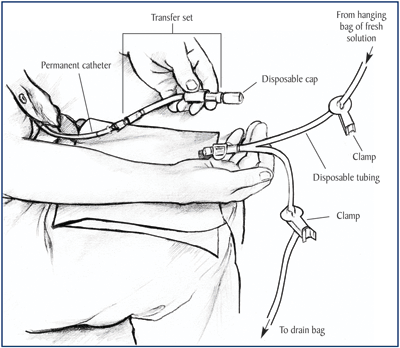
Figure 9. Transfer set. Between exchanges, you can keep your catheter and transfer set hidden inside your clothing. At the beginning of an exchange, you will remove the disposable cap from the transfer set and connect it to a Y-tube. The branches of the Y-tube connect to the drain bag and the bag of fresh dialysis solution. Always wash your hands before handling your catheter and transfer set, and wear a surgical mask whenever you connect or disconnect.
Figure 10. During an exchange, you can read, talk, watch television, or sleep.
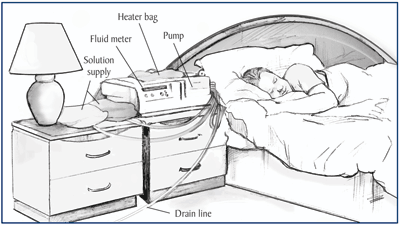
Figure 11. A cycler performs four or five exchanges overnight, while you sleep.
Renal dialysis, also called kidney dialysis or simply dialysis, is a medical treatment for removing harmful wastes and surplus salt and water from the blood following kidney failure. When in good working order kidneys clean the blood. They also make hormones that keep bones strong and blood healthy. When kidneys fail, there are two options: a kidney transplant or dialysis.
There are two main types of dialysis: hemodialysis and peritoneal dialysis. Both types filter the blood, hemodialysis using a machine and peritoneal dialysis using the lining of the abdomen, called the peritoneal membrane. Each type has both risks and benefits. They also require that a special diet be followed.
Hemodialysis
Hemodialysis is the most common method used to treat advanced and permanent kidney failure. Since the 1960s, when hemodialysis first became a practical treatment for kidney failure, much has been learned much about how to make hemodialysis treatments more effective and minimize side effects. In recent years, more compact and simpler dialysis machines have made home dialysis increasingly attractive. But even with better procedures and equipment, hemodialysis is still a complicated and inconvenient therapy that requires a coordinated effort from your whole health care team, including a nephrologist, dialysis nurse, dialysis technician, dietitian, and social worker. The most important members of your health care team are you and your family. By learning about your treatment, you can work with your health care team to give yourself the best possible results, and you can lead a full, active life.
How hemodialysis works
In hemodialysis (Figure 2), your blood is allowed to flow, a few ounces at a time, through a special filter that removes wastes and extra fluids. The clean blood is then returned to your body. Removing the harmful wastes and extra salt and fluids helps control your blood pressure and keep the proper balance of chemicals like potassium and sodium in your body.
One of the biggest adjustments you must make when you start hemodialysis treatments is following a strict schedule. Most patients go to a clinic – a dialysis center – three times a week for 3 to 5 or more hours each visit. For example, you may be on a Monday-Wednesday-Friday schedule or a Tuesday-Thursday-Saturday schedule. You may be asked to choose a morning, afternoon, or evening shift, depending on availability and capacity at the dialysis unit. Your dialysis center will explain your options for scheduling regular treatments.
Researchers are exploring whether shorter daily sessions, or longer sessions performed overnight while the patient sleeps, are more effective in removing wastes. Newer dialysis machines make these alternatives more practical with home dialysis.
In the US, several centers around the country teach people how to perform their own hemodialysis treatments at home. A family member or friend who will be your helper must also take the training, which usually takes at least 4 to 6 weeks. Home dialysis gives you more flexibility in your dialysis schedule. With home hemodialysis, the time for each session and the number of sessions per week may vary, but you must maintain a regular schedule by giving yourself dialysis treatments as often as you would receive them in a dialysis unit.
Adjusting to changes
Even in the best situations, adjusting to the effects of kidney failure and the time you spend on dialysis can be difficult. Aside from the "lost time," you may have less energy. You may need to make changes in your work or home life, giving up some activities and responsibilities. Keeping the same schedule you kept when your kidneys were working can be very difficult now that your kidneys have failed. Accepting this new reality can be very hard on you and your family. A counselor or social worker can answer your questions and help you cope.
Many patients feel depressed when starting dialysis, or after several months of treatment. If you feel depressed, you should talk with your social worker, nurse, or doctor because this is a common problem that can often be treated effectively.
Getting your vascular access ready
One important step before starting hemodialysis is preparing a vascular access, a site on your body from which your blood is removed and returned. A vascular access should be prepared weeks or months before you start dialysis. It will allow easier and more efficient removal and replacement of your blood with fewer complications. Figures 3 and 4.
Equipment and procedures
When you first visit a hemodialysis center, it may seem like a complicated mix of machines and people. But once you learn how the procedure works and become familiar with the equipment, you'll be more comfortable.
Dialysis machine
The dialysis machine is about the size of a dishwasher. It has three main jobs:
Dialyzer
The dialyzer is a large canister containing thousands of small fibers through which your blood is passed (Fig 5). Dialysis solution, the cleansing fluid, is pumped around these fibers. The fibers allow wastes and extra fluids to pass from your blood into the solution, which carries them away. The dialyzer is sometimes called an artificial kidney.
Dialysis solution
Dialysis solution, also known as dialysate, is the fluid in the dialyzer that helps remove wastes and extra fluid from your blood. It contains chemicals that make it act like a sponge. Your doctor will give you a specific dialysis solution for your treatments. This formula can be adjusted based on how well you handle the treatments and on your blood tests.
Needles
Many people find the needle sticks to be one of the hardest parts of hemodialysis treatments. Most people, however, report getting used to them after a few sessions. If you find the needle insertion painful, an anesthetic cream or spray can be applied to the skin. The cream or spray will numb your skin briefly so you won't feel the needle.
Most dialysis centers use two needles – one to carry blood to the dialyzer and one to return the cleaned blood to your body. Some specialized needles are designed with two openings for two-way flow of blood, but these needles are less efficient and require longer sessions. Needles for high-flux or high-efficiency dialysis need to be a little larger than those used with regular dialyzers.
Some people prefer to insert their own needles. You'll need training on inserting needles properly to prevent infection and protect your vascular access. You may also learn a "ladder" strategy for needle placement in which you "climb" up the entire length of the access session by session so that you don't weaken an area with a grouping of needle sticks. A different approach is the "buttonhole" strategy in which you use a limited number of sites but insert the needle back into the same hole made by the previous needle stick. Whether you insert your own needles or not, you should know these techniques to better care for your access.
Tests to see how well your dialysis is working
About once a month, your dialysis care team will test your blood by using one of two formulas – URR or Kt/V – to see whether your treatments are removing enough wastes. Both tests look at one specific waste product, called blood urea nitrogen (BUN), as an indicator for the overall level of waste products in your system.
Conditions related to kidney failure and their treatments
Your kidneys do much more than remove wastes and extra fluid. They also make hormones and balance chemicals in your system. When your kidneys stop working, you may have problems with anemia and conditions that affect your bones, nerves, and skin. Some of the more common conditions caused by kidney failure are extreme tiredness, bone problems, joint problems, itching, and "restless legs." Restless legs will keep you awake as you feel them twitching and jumping.
Anemia and erythropoietin (EPO)
Anemia is a condition in which the volume of red blood cells (erythrocytes) is low. Red blood cells carry oxygen to cells throughout the body. Without oxygen, cells can't use the energy from food, so someone with anemia may tire easily and look pale. Anemia can also contribute to heart problems.
Anemia is common in people with kidney disease because the kidneys produce the hormone erythropoietin, or EPO, which stimulates the bone marrow to produce red blood cells. Diseased kidneys often don't make enough EPO, and so the bone marrow makes fewer red blood cells. EPO is available commercially and is commonly given to patients on dialysis.
Renal osteodystrophy
The term "renal" describes things related to the kidneys. Renal osteodystrophy, or bone disease of kidney failure, affects 90% of dialysis patients. It causes bones to become thin and weak or formed incorrectly and affects both children and adults. Symptoms can be seen in growing children with kidney disease even before they start dialysis. Older patients and women who have gone through menopause are at greater risk for this disease.
iIching (pruritus)
Many people treated with hemodialysis complain of itchy skin, which is often worse during or just after treatment. Itching is common even in people who don't have kidney disease; in kidney failure, however, itching can be made worse by wastes in the bloodstream that current dialyzer membranes can't remove from the blood.
The problem can also be related to high levels of parathyroid hormone (PTH). Some people have found dramatic relief after having their parathyroid glands removed. The four parathyroid glands sit on the outer surface of the thyroid gland, which is located on the windpipe in the base of your neck, just above the collarbone. The parathyroid glands help control the levels of calcium and phosphorus in the blood.
But a cure for itching that works for everyone has not been found. Phosphate binders seem to help some people; these medications act like sponges to soak up, or bind, phosphorus while it is in the stomach. Others find relief after exposure to ultraviolet light. Still others improve with EPO shots. A few antihistamines (Benadryl, Atarax, Vistaril) have been found to help; also, capsaicin cream applied to the skin may relieve itching by deadening nerve impulses. In any case, taking care of dry skin is important. Applying creams with lanolin or camphor may help.
Sleep disorders
Patients on dialysis often have insomnia, and some people have a specific problem called the sleep apnea syndrome, which is often signaled by snoring and breaks in snoring. Episodes of apnea are actually breaks in breathing during sleep. Over time, these sleep disturbances can lead to "day-night reversal" (insomnia at night, sleepiness during the day), headache, depression, and decreased alertness. The apnea may be related to the effects of advanced kidney failure on the control of breathing. Treatments that work with people who have sleep apnea, whether they have kidney failure or not, include losing weight, changing sleeping position, and wearing a mask that gently pumps air continuously into the nose (nasal continuous positive airway pressure, or CPAP).
Many people on dialysis have trouble sleeping at night because of aching, uncomfortable, jittery, or "restless" legs. You may feel a strong impulse to kick or thrash your legs. Kicking may occur during sleep and disturb a bed partner throughout the night. The causes of restless legs may include nerve damage or chemical imbalances.
Moderate exercise during the day may help, but exercising a few hours before bedtime can make it worse. People with restless leg syndrome should reduce or avoid caffeine, alcohol, and tobacco; some people also find relief with massages or warm baths. A class of drugs called benzodiazepines, often used to treat insomnia or anxiety, may help as well. These prescription drugs include Klonopin, Librium, Valium, and Halcion. A newer and sometimes more effective therapy is levodopa (Sinemet), a drug used to treat Parkinson's disease.
Sleep disorders may seem unimportant, but they can impair your quality of life. Don't hesitate to raise these problems with your nurse, doctor, or social worker.
Amyloidosis
Dialysis-related amyloidosis (DRA) is common in people who have been on dialysis for more than 5 years. DRA develops when proteins in the blood deposit on joints and tendons, causing pain, stiffness, and fluid in the joints, as is the case with arthritis. Working kidneys filter out these proteins, but dialysis filters are not as effective.
How diet can help
Eating the right foods can help improve your dialysis and your health. Your clinic has a dietitian to help you plan meals. Follow the dietitian's advice closely to get the most from your hemodialysis treatments. Here are a few general guidelines.
You can also ask your dietitian for recipes and titles of cookbooks for patients with kidney disease. Following the restrictions of a diet for kidney disease might be hard at first, but with a little creativity, you can make tasty and satisfying meals.
Peritoneal dialysis
With peritoneal dialysis (PD), you have some choices in treating advanced and permanent kidney failure (Figure 7). Since the 1980s, when PD first became a practical and widespread treatment for kidney failure, much has been learned about how to make PD more effective and minimize side effects. Since you don't have to schedule dialysis sessions at a center, PD gives you more control. You can give yourself treatments at home, at work, or on trips. But this independence makes it especially important that you work closely with your health care team: your nephrologist, dialysis nurse, dialysis technician, dietitian, and social worker.
How peritoneal dialysis works
In PD, a catheter is used to fill your abdomen with a cleansing liquid called dialysis solution. The walls of your abdominal cavity are lined with a membrane called the peritoneum, which allows waste products and extra fluid to pass from your blood into the dialysis solution. The solution contains a sugar called dextrose that will pull wastes and extra fluid into the abdominal cavity. These wastes and fluid then leave your body when the dialysis solution is drained. The used solution, containing wastes and extra fluid, is then thrown away. The process of draining and filling is called an exchange and takes about 30 to 40 min. The period the dialysis solution is in your abdomen is called the dwell time. A typical schedule calls for four exchanges a day, each with a dwell time of 4 to 6 hr. Different types of PD have different schedules of daily exchanges.
One form of PD, continuous ambulatory peritoneal dialysis (CAPD), doesn't require a machine. As the word ambulatory suggests, you can walk around with the dialysis solution in your abdomen. Another form of PD, continuous cycler-assisted peritoneal dialysis (CCPD), requires a machine called a cycler to fill and drain your abdomen, usually while you sleep. CCPD is also sometimes called automated peritoneal dialysis (APD).
Getting ready for PD
Whether you choose an ambulatory or automated form of PD, you'll need to have a soft catheter placed in your abdomen. The catheter is the tube that carries the dialysis solution into and out of your abdomen. If your doctor uses open surgery to insert your catheter, you will be placed under general anesthesia. Another technique requires only local anesthetic. Your doctor will make a small cut, often below and a little to the side of your navel (belly button), and then guide the catheter through the slit into the peritoneal cavity. As soon as the catheter is in place, you can start to receive solution through it, although you probably won't begin a full schedule of exchanges for 2 to 3 weeks. This break-in period lets you build up scar tissue that will hold the catheter in place.
The standard catheter for PD is made of soft tubing for comfort. It has cuffs made of a polyester material, called Dacron, that merge with your scar tissue to keep it in place. The end of the tubing that is inside your abdomen has many holes to allow the free flow of solution in and out. Fig 8.
Types of pertineal dialysis
The type of PD you choose will depend on the schedule of exchanges you would like to follow, as well as other factors. You may start with one type of PD and switch to another, or you may find that a combination of automated and nonautomated exchanges suits you best. Work with your health care team to find the best schedule and techniques to meet your lifestyle and health needs.
Continuous ambulatory peritoneal dialysis (CAPD)
If you choose CAPD, you'll drain a fresh bag of dialysis solution into your abdomen. After 4 to 6 or more hours of dwell time, you'll drain the solution, which now contains wastes, into the bag. You then repeat the cycle with a fresh bag of solution. You don't need a machine for CAPD; all you need is gravity to fill and empty your abdomen. Your doctor will prescribe the number of exchanges you'll need, typically three or four exchanges during the day and one evening exchange with a long overnight dwell time while you sleep.
Continuous cycler-assisted peritoneal dialysis (CCPD)
CCPD uses an automated cycler to perform three to five exchanges during the night while you sleep. In the morning, you begin one exchange with a dwell time that lasts the entire day.
Customizing your PD
If you've chosen CAPD, you may have a problem with the long overnight dwell time. It's normal for some of the dextrose in the solution to cross into your body and become glucose. The absorbed dextrose doesn't create a problem during short dwell times. But overnight, some people absorb so much dextrose that it starts to draw fluid from the peritoneal cavity back into the body, reducing the efficiency of the exchange. If you have this problem, you may be able to use a minicycler (a small version of a machine that automatically fills and drains your abdomen) to exchange your solution once or several times overnight while you sleep. These additional, shorter exchanges will minimize solution absorption and give you added clearance of wastes and excess fluid.
If you've chosen CCPD, you may have a solution absorption problem with the daytime exchange, which has a long dwell time. You may find you need an additional exchange in the mid-afternoon to increase the amount of waste removed and to prevent excessive absorption of solution.
Preventing problems
Infection is the most common problem for people on PD. Your health care team will show you how to keep your catheter bacteria-free to avoid peritonitis, which is an infection of the peritoneum. Improved catheter designs protect against the spread of bacteria, but peritonitis is still a common problem that sometimes makes continuing PD impossible. You should follow your health care team's instructions carefully, but here are some general rules:
Keep a close watch for any signs of infection and report them so they can be treated promptly. Here are some signs to watch for:
Equipment and supplies for PD
Transfer set
A transfer set (Fig 9) is tubing that connects the bag of dialysis solution to the catheter. When your catheter is first placed, the exposed end of the tube will be securely capped to prevent infection. Under the cap is a universal connector.
When you start dialysis training, your dialysis nurse will provide a transfer set. The type of transfer set you receive depends on the company that supplies your dialysis solution. Different companies have different systems for connecting to your catheter.
Connecting the transfer set requires sterile technique. You and your nurse will wear surgical masks. Your nurse will soak the transfer set and the end of your catheter in an antiseptic solution for 5 minutes before making the connection. The nurse will wear rubber gloves while making the connection.
Depending on the company that supplies your solution, your transfer set may require a new cap each time you disconnect from the bag after an exchange (Figures 10 and 11). With a different system, the tubing that connects to the transfer set includes a piece that can be clamped at the end of an exchange and then broken off from the tubing so that it stays on the transfer set as a cap until it is removed for the next exchange. Your dialysis nurse will train you in the aseptic (germ-free) technique for connecting at the beginning of an exchange and disconnecting at the end. Follow instructions carefully to avoid infection.
Dialysis solution
Dialysis solution comes in 1.5-, 2-, 2.5-, or 3-liter bags. A liter is slightly more than 1 quart. The dialysis dose can be increased by using a larger bag, but only within the limit of the amount your abdomen can hold. The solution contains a sugar called dextrose, which pulls extra fluid from your blood. Your doctor will prescribe a formula that fits your needs.
You'll need a clean space to store your bags of solution and other supplies. You may also need a special heating device to warm each bag of solution to body temperature before use. Most solution bags come in a protective outer wrapper that allows for microwave heating. Do not microwave a bag of solution after it has been removed from its wrapper because microwaving can change the chemical makeup of the solution.
Cycler
The cycler – which automatically fills and drains your abdomen, usually at night while you sleep – can be programmed to deliver specified volumes of dialysis solution on a specified schedule. Most systems include the following components:
Testing the effectiveness of your dialysis
To see if the exchanges are removing enough waste products, such as urea, your health care team must perform several tests. These tests are especially important during the first weeks of dialysis to determine whether you're receiving an adequate amount, or dose, of dialysis.
The peritoneal equilibration test (often called the PET) measures how much sugar has been absorbed from a bag of infused dialysis solution and how much urea and creatinine have entered into the solution during a 4-hour exchange. The peritoneal transport rate varies from person to person. If you have a high rate of transport, you absorb sugar from the dialysis solution quickly and should avoid exchanges with a very long dwell time because you're likely to absorb too much solution from such exchanges.
In the clearance test, samples of used solution drained over a 24-hour period are collected, and a blood sample is obtained during the day when the used solution is collected. The amount of urea in the used solution is compared with the amount in the blood to see how effective the PD schedule is in removing urea from the blood. For the first months or even years of PD treatment, you may still produce small amounts of urine. If your urine output is more than several hundred milliliters per day, urine is also collected during this period to measure its urea concentration.
From the used solution, urine, and blood measurements, your health care team can compute a urea clearance, called Kt/V, and a creatinine clearance rate (adjusted to body surface area). The residual clearance of the kidneys is also considered. These measurements will show whether the PD prescription is adequate.
If the laboratory results show that the dialysis schedule is not removing enough urea and creatinine, the doctor may change the prescription by
Compliance
One of the big problems with PD is that patients sometimes don't perform all of the exchanges prescribed by their medical team. They either skip exchanges or sometimes skip entire treatment days when using CCPD. Skipping PD treatments has been shown to increase the risk of hospitalization and death.
Remaining kidney function
Normally the PD prescription factors in the amount of residual, or remaining, kidney function. Residual kidney function typically falls, although slowly, over months or even years of PD. This means that more often than not, the number of exchanges prescribed, or the volume of exchanges, needs to increase as residual kidney function falls.
The doctor should determine your PD dose on the basis of practice standards established by the National Kidney Foundation Dialysis Outcomes Quality Initiative (NKF-DOQI). Work closely with your health care team to ensure that you get the proper dose, and follow instructions carefully to make sure you get the most out of your dialysis exchanges.


