THE HEALTH REVOLUTION: Surgery and Medicine in the Twenty-first Century - 3. Lifesaving Machines
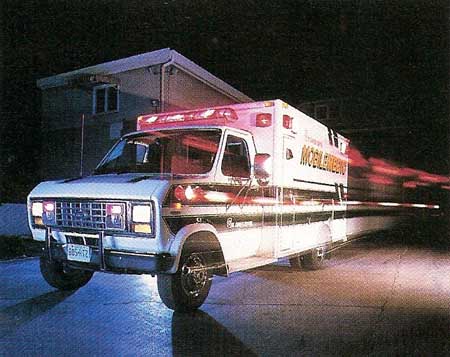
Figure 1. A modern ambulance, equipped with advanced lifesaving equipment, races to the scene of accident.

Figure 2. A heart attack victim being treated at home by a rescuer using an automatic defibrillator.
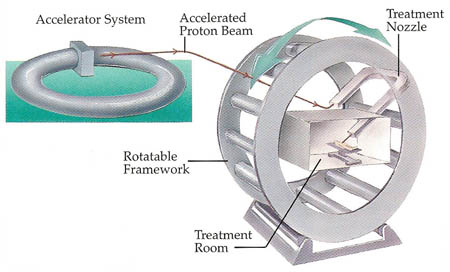
Figure 3. Proton accelerators show much promise in treating cancer. Powerful magnets create a magnetic field that accelerates protons to high speed. The protons can then be focused into a beam. The patient is placed inside a vast rotating wheel. The focused beam of protons breaks up the tumor, which is then excreted by the body. Healthy tissue near the tumor is not damaged.
Many people die needlessly each year simply because they don't receive medical treatment early enough. Further developments in such scanning methods as PET and MRI will mean that doctors will be able to detect the onset of life-threatening diseases at an earlier stage. Even the smallest of tumors will be found during routine scans and then, if necessary, will be treated by minimum-intervention methods before the tumors have a chance to threaten a patient's life.
More lives will also be saved in the future as a result of improvements in the speed and effectiveness of treatment given to accident and emergency victims (see Figure 1). How soon a medical team can get to a critically ill patient and what resources are immediately at hand can make the difference between life and death for such patients.
Heart Restart
No medical emergency is more urgent than a sudden heart attack, or cardiac arrest. All at once and without warning, a person's heart stops beating properly and the flow of blood to the brain is cut off.
Even the short delay in getting a heart attack victim to a hospital may be too long. For this reason, ambulance crews are trained in two basic methods of revival (see Figure 2). In the first, known as CPR (cardiopulmonary resuscitation), a medical technician breathes into the patient's mouth and presses on the chest repeatedly to keep the blood flowing and force oxygen as quickly as possible to the brain, heart, and other vital systems.
The emergency crew may also use a DEFIBRILLATOR. This device consists of two metal plates that can deliver a brief but powerful electric shock through the patient's heart. The sudden shock interrupts the random twitching of the heart muscles and stimulates the heart to resume its normal beating.
The difficulty is that too much time may pass before an expert is on hand to work an ordinary defibrillator. However, newly developed automatic defibrillators are helping to overcome this problem. The rescuer simply attaches sticky electrodes to the victim's chest and the automatic defibrillator does the rest. Programmed to measure the condition of the heart, it determines whether to give a shock. If a shock is needed, it determines where this shock should be directed and how strong it should be. A synthesized voice or visual display guides the rescuer in setting up the device. <
Another recent development is the surgically implanted defibrillator. This is placed just under the skin of the patient's abdomen, where it continually monitors the heart's beating with a microcomputer. If the beats become weak and irregular, the device sends out a series of electrical pulses through fine wires leading to the heart. The pulses continue for 15 to 20 seconds. Since the pulse do not have to pass through the chest wall, they need only about one-fifteenth as much energy to control heartbeat as a normal defibrillator provides. The power source for the implant is a lithium battery that lasts about three years and can be replaced at regular intervals during a minor operation.
Monitors and Alarms
Doctors fighting to save the life of a critically ill or injured person rely on an array of instruments to continuously monitor the patient's breathing and heart condition. On of the most important tools at their disposal is the electrocardiograph (EKG).
The electrocardiograph works by sensing the weak electrical currents produced by muscles in the heart. These are transmitted to the machine through wires from a number of electrodes, which are smeared with conducting paste and fixed to the arms, legs, and chest. The EKG then amplifies the currents about 3,000 times and traces the patterns of heart waves on a screen or strip of paper.
A patient who is recovering from a heart attack or from cardiac surgery is connected to an EKG in the recovery room. If the device senses that the heart is behaving abnormally, it instantly sounds an alarm at the nearest nurses' station.
One of the latest monitoring devices is the niroscope. This can show within two to three seconds whether the brain is receiving enough oxygen. Such a warning may be crucial, for example, while the patient is under an anesthetic. If deprived of oxygen for just three to four minutes, the brain would be permanently damaged.
The niroscope works by shining infrared light of different frequencies through the skull into the brain and measuring how much of that light is reflected back out. The operation of the niroscope is based on the fact that brain tissue absorbs different amounts of infrared light, depending on the amount of oxygen available to the brain cells.
Another valuable new tool is the echocardiograph. This instrument records the echoes of ultrasound waves from various parts of the heart. The instrument can show blood clots, faulty valves, and other abnormalities of the heart that might otherwise escape detection. One recent development of this technique involves the use of tiny sound transmitters that provide an even clearer image of the beating heart. The transmitters are located at the top if an endoscope that is passed down the patient's throat. By altering the angle and position of the tip of the endoscope, the doctor can accurately direct ultrasound waves at a particular section of the heart and so obtain an image of that section while the heart is beating.
| Machines That Changed Medicine | ||
|---|---|---|
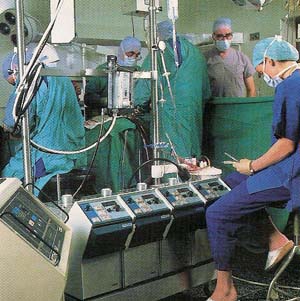
Stopping the heart long enough for surgery to be performed on it would once have been unthinkable. But this procedure is now routinely carried out, thanks to the development of the heart-lung machine. Blood from the patient is pumped into the machine. There the blood is supplied with oxygen – a task normally done by the lungs – and then passed back into the patient.
Another great medical breakthrough has been the construction of a machine to take over the role of the kidneys. These organs filter blood to remove impurities that, if allowed to accumulate, can seriously damage the body. Patients whose kidneys no longer work properly are connected to a kidney dialysis machine several times a week. The machine filters the blood artificially and returns the purified blood to the body. At first, dialysis machines were large, expensive, and in short supply, so difficult decisions had to be made concerning who would receive treatment and who would not. But advances in the technology of these devices have produced much smaller and less expensive machines that can be installed at home, which makes more machines available to more people. |
Blasting Tumors
In the battle against cancer, doctors now have a variety of different weapons from which to choose. They can operate to cut away a tumor or burn it with a high-energy laser, treat the patient with a combination of cancer-destroying chemicals, or expose the diseased area to radiation.
Bathing a tumor in radiation from a radioactive source, however, has the side effect of damaging healthy tissue around the tumor. For this reason, much interest is being shown in a new form of cancer treatment involving proton beams (see Figure 3).
Proton are positively-charged particles found inside the central part, or nucleus, of atoms. Being electrically charged, protons can be accelerated to high speed by a ring of powerful magnets inside a vast doughnut-shaped proton accelerator. protons emerging from the accelerator can then be focused into a tight beam and fired with great accuracy down a nozzle at the diseased part of the patient's body.
The patient lies inside a giant rotating wheel that can direct the depth of the proton beam coming from the accelerator to within an accuracy of a few millimeters. Such fine targeting means that the maximum dose of radiation can be delivered to the tumor. As a result, the tumor is broken up and is then excreted by the body. Tissue lying in front of or behind the tumor, however, is left undamaged since it is not subjected to such an intense bombardment of protons.