Tay-Sachs disease
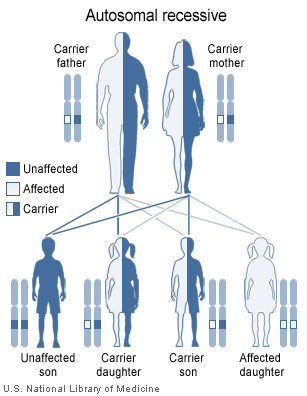
The pattern of inheritance of an automosal recessive disease.
Tay-Sachs disease is a fatal genetic lipid storage disorder in which harmful quantities of a fatty substance called ganglioside GM2 build up in tissues and nerve cells in the brain. The condition is caused by insufficient activity of an enzyme called beta-hexosaminidase A that catalyzes the biodegradation of acidic fatty materials known as gangliosides. Gangliosides are made and biodegraded rapidly in early life as the brain develops.
Infants with Tay-Sachs disease appear to develop normally for the first few months of life. Then, as nerve cells become distended with fatty material, a relentless deterioration of mental and physical abilities occurs. The child becomes blind, deaf, and unable to swallow. Muscles begin to atrophy and paralysis sets in. Other neurological symptoms include dementia, seizures, and an increased startle reflex to noise. A much rarer form of the disorder occurs in patients in their twenties and early thirties and is characterized by an unsteady gait and progressive neurological deterioration. Persons with Tay-Sachs also have "cherry-red" spots in their eyes. The incidence of Tay-Sachs is particularly high among people of Eastern European and Askhenazi Jewish descent. Patients and carriers of Tay-Sachs disease can be identified by a simple blood test that measures beta-hexosaminidase A activity.
Tay-Sachs is an autosomal recessive disease, so that both parents must carry the mutated gene in order to have an affected child. In these instances, there is a 25 percent chance with each pregnancy that the child will be affected with Tay-Sachs disease. Tay-Sachs is now largely prevented by genetic counseling of high-risk groups, such as Ashkenazi Jews. Prenatal diagnosis is available if desired.
Treatment
Presently there is no treatment for Tay-Sachs disease. Anticonvulsant medicine may initially control seizures. Other supportive treatment includes proper nutrition and hydration and techniques to keep the airway open. Children may eventually need a feeding tube.
Prognosis
Even with the best of care, children with Tay-Sachs disease usually die by age 4, from recurring infection.


