Raynaud's disease
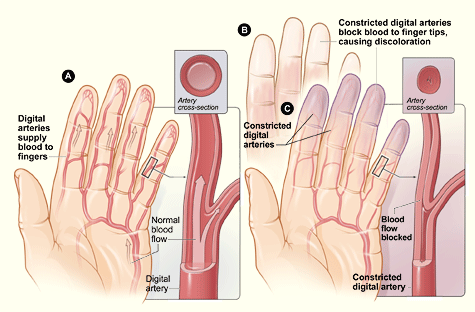
Figure A shows the normal digital arteries with normal blood flow to the fingers. The inset images show cross-sections of a normal artery. Figure B shows white discoloration of the fingertips caused by blocked blood flow. Figure C shows narrowed digital arteries, causing blocked blood flow and purple discoloration of the fingertips. The inset images show cross-sections of a narrowed artery blocking the flow of blood.
Raynaud's disease and Raynaud's phenomenon are rare disorders that affect blood vessels. These disorders are marked by brief episodes of vasospasm (narrowing of the blood vessels). Vasospasm causes decreased blood flow to the fingers and toes, and rarely to the nose, ears, nipples, and lips. The fingers are the most commonly affected area, but the toes also are affected in 40 percent of people with Raynaud's.
When this disorder occurs without any known cause, it is called Raynaud's disease, or primary Raynaud's. When the condition occurs along with a likely cause, it is known as Raynaud's phenomenon, or secondary Raynaud's. Primary Raynaud's is more common and tends to be less severe than secondary Raynaud's.
When you have primary or secondary Raynaud's, cold temperatures or stressful emotions can trigger attacks. During these attacks, there is a brief lack of blood flow to the affected body part(s), and the skin can temporarily become white then bluish. As blood flow returns to the area, the skin turns red. The affected areas can throb or feel numb and tingly. With severe Raynaud's, prolonged or repeated episodes can cause sores or tissue death (gangrene).
It is normal for the body to keep its vital inner organs warm by limiting blood flow to the arms, legs, fingers, and toes. The body naturally does this in response to a long period of cold. This response can cause frostbite. In people with Raynaud's, the response to cold is quicker and stronger. The response can be triggered by mild or short-lived changes in temperature, such as:
In people with Raynaud's, blood flow is more strongly reduced in response to cold temperatures than in people without the disorder. When Raynaud's is severe (which is uncommon), exposure to cold for as little as 20 minutes can cause major tissue damage.
The blood vessels of people with Raynaud's also physically overreact to stressful emotions. It is normal during times of psychological stress for the body to release hormones that narrow its blood vessels. But for people with Raynaud's, this squeezing of blood vessels is stronger. This results in less blood reaching fingers, toes, and sometimes other extremities.
Outlook
For most people, primary Raynaud's is more of a bother than a serious illness and it can usually be managed with minor lifestyle changes. Secondary Raynaud's can be more difficult to manage, but several treatments may help prevent or relieve symptoms. Among the most important treatments for secondary Raynaud's is treating of the underlying condition.
Causes
In most cases of Raynaud's, no cause can be found. When this happens, the disorder is called primary Raynaud's. When a cause can be found, the disorder is called secondary Raynaud's. Secondary Raynaud's can be linked to many different medical or workplace conditions, such as:
Diseases
Secondary Raynaud's is especially common in people who have scleroderma or systemic lupus erythematosus. About 9 out of 10 people with scleroderma have Raynaud's. About 1 out of 3 people with lupus have Raynaud's. The disease also is linked to other diseases that damage blood vessels or nerves, including:
Raynaud's also can be associated with thyroid problems and pulmonary arterial hypertension (high blood pressure in the arteries of the lungs).
Repetitive actions
Typing, playing the piano, or another repetitive action done for long periods of time is often linked to secondary Raynaud's. Using vibrating tools at work also can make you more likely to develop the disorder.
Chemicals
Exposure to certain chemicals at work can cause a scleroderma-like illness that is linked to Raynaud's. Nicotine in cigarette smoke also can make you more prone to developing Raynaud's.
Medicines
Several medicines are linked to secondary Raynaud's, including:
Who is at risk?
About 3 out of 4 cases of primary Raynaud's occur in women between the ages of 15 and 40 years, although the reason is unknown. People in colder climates are also more likely to develop Raynaud's than people in warmer areas.
Signs and symptoms
People with Raynaud's (primary or secondary) have attacks in response to cold or emotional stress. The attacks can affect the fingers and toes, and rarely the nose, ears, nipples, or lips. The affected body parts will usually have two or more of the following changes:
Attacks usually last about 15 minutes. They can last less than a minute or as long as several hours. Attacks can occur daily or weekly.
Sometimes attacks affect only one or two fingers or toes. Different areas may be affected at different times. Attacks can cause sores or tissue death (gangrene) in people with severe secondary Raynaud's. However, severe Raynaud's is very uncommon.
Diagnosis
Raynaud's is usually diagnosed based on a patient's history of experiencing color changes in their extremities in response to exposure to cold or emotional stress. A cold simulation test also may be used to provoke symptoms for the doctor to see.
Doctors use the patient's history of symptoms, a physical exam, and diagnostic tests to rule out other conditions that might act like Raynaud's.
Specialists involved
A rheumatologist is a doctor who specializes in treating disorders of the joints, bones, and muscles. Often, a rheumatologist diagnoses and treats patients with Raynaud's, but internists and family practice doctors also are able to diagnose and treat Raynaud's.
Diagnostic tests and procedures
To help diagnose Raynaud's, doctors may do a cold simulation test. This test can trigger an attack that is typical of the disorder. They also may do tests for inflammatory disorders that damage blood vessels or nerves. Having these conditions along with Raynaud's symptoms makes it more likely that a patient has secondary Raynaud's disease.
In the cold simulation test, temperature sensors are taped to the fingers of the hand. The hand is then briefly exposed to the cold, usually by dunking it in ice water. If the patient likely has Raynaud's, it will take more than the normal time for the finger temperature to return to what it was at the start of the test.
Doctors also may do a test called a nailfold capillaroscopy. For this test, the doctor puts a drop of oil on the skin at the base of the fingernail and then looks at it under a microscope. If the doctor sees abnormal looking blood vessels, this suggests an inflammatory disorder such as scleroderma.
Doctors also can use two specific blood tests to look for inflammatory conditions: the antinuclear antibody test and the erythrocyte sedimentation rate.
Treatment
There is no cure for primary or secondary Raynaud's, but many measures can reduce the number or intensity of attacks, including:
In most people with primary Raynaud's, the disorder is successfully managed with lifestyle adjustments. Patients with secondary Raynaud's may need medicines in addition to lifestyle changes, and in rare cases, they may need surgery. Anyone with Raynaud's who develops sores on their fingers or toes or elsewhere on their body should see a doctor right away to prevent tissue loss.
Lifestyle changes
Most of the lifestyle changes that help people with Raynaud's aim to avoid the triggers of attacks. These triggers include cold, emotional stress, and certain medicines, chemicals, or actions. To protect the body from cold, people can:
To avoid emotional triggers, people can steer clear of stressful situations if possible. Relaxation techniques also can be helpful under stress.
To avoid workplace or recreational triggers, people can:
A number of medicines can trigger attacks. People with Raynaud's should avoid:
Other helpful lifestyle changes for people with Raynaud's are those that boost blood flow in the body. These include exercising regularly and quitting smoking.
When attacks do occur, people with Raynaud's can take several steps to limit the length and strength of the attacks. These steps include:
Medicines and surgery
Most of the medicines used to treat people with Raynaud's are given to improve blood flow to the extremities. These medicines include calcium channel-blockers, such as:
Calcium channel-blockers help limit the number and severity of attacks in about 2 out of 3 patients with Raynaud's.
Also helpful are alpha-blockers, such as prazosin and doxazosin. In addition, skin creams that dilate blood vessels, such as nitroglycerine paste, can help heal skin sores.
The rare patient who develops sores or tissue death (gangrene) needs more aggressive treatment. Such treatment includes antibiotics and surgery to cut out damaged tissue. People with severe, worsening Raynaud's may have surgery or shots to block the action of nerves in the hands and feet that control blood flow in the skin. This surgery often gets rid of symptoms for 1–2 yr. Patients may need shots more than once.
Living with Raynaud's disease
Primary and secondary Raynaud's are conditions that may be lifelong. Most people with primary Raynaud's respond to simple lifestyle changes or medicines. Such treatment is not always as successful in secondary Raynaud's. If you have secondary Raynaud's, you may find that in time your medicines are less effective and your attacks become more frequent and/or more severe. Switching to a new treatment may help relieve or prevent your symptoms. Be sure to seek a doctor's care if you develop sores on your fingers or toes or elsewhere on the body.


