rheumatoid arthritis
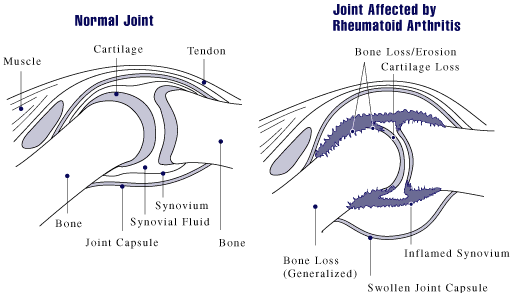
A joint (the place where two bones meet) is surrounded by a capsule that protects and supports it. The joint capsule is lined with a type of tissue called synovium, which produces synovial fluid that lubricates and nourishes joint tissues. In rheumatoid arthritis, the synovium becomes inflamed, causing warmth, redness, swelling, and pain. As the disease progresses, the inflamed synovium invades and damages the cartilage and bone of the joint. Surrounding muscles, ligaments, and tendons become weakened. Rheumatoid arthritis also can cause more generalized bone loss that may lead to osteoporosis (fragile bones that are prone to fracture).
Rheumatoid arthritis is an inflammatory disease that causes pain, swelling, stiffness, and loss of function in the joints. It has several special features that make it different from other kinds of arthritis. For example, rheumatoid arthritis generally occurs in a symmetrical pattern, meaning that if one knee or hand is involved, the other one also is. The disease often affects the wrist joints and the finger joints closest to the hand. It can also affect other parts of the body besides the joints. In addition, people with rheumatoid arthritis may have fatigue, occasional fevers, and a general sense of not feeling well.
Rheumatoid arthritis affects people differently. For some people, it lasts only a few months or a year or two and goes away without causing any noticeable damage. Other people have mild or moderate forms of the disease, with periods of worsening symptoms, called flares, and periods in which they feel better, called remissions. Still others have a severe form of the disease that is active most of the time, lasts for many years or a lifetime, and leads to serious joint damage and disability.
Features of rheumatoid arthritis
Although rheumatoid arthritis can have serious effects on a person's life and well-being, current treatment strategies – including pain-relieving drugs and medications that slow joint damage, a balance between rest and exercise, and patient education and support programs – allow most people with the disease to lead active and productive lives. In recent years, research has led to a new understanding of rheumatoid arthritis and has increased the likelihood that, in time, researchers will find even better ways to treat the disease.
Development and progression
Joints
A joint is a place where two bones meet. The ends of the bones are covered by cartilage, which allows for easy movement of the two bones. The joint is surrounded by a capsule that protects and supports it. The joint capsule is lined with a type of tissue called synovium, which produces synovial fluid, a clear substance that lubricates and nourishes the cartilage and bones inside the joint capsule.
Like many other rheumatic diseases, rheumatoid arthritis is an autoimmune disease (auto means self), so-called because a person's immune system, which normally helps protect the body from infection and disease, attacks joint tissues for unknown reasons. White blood cells, the agents of the immune system, travel to the synovium and cause inflammation (synovitis), characterized by warmth, redness, swelling, and pain – typical symptoms of rheumatoid arthritis. During the inflammation process, the normally thin synovium becomes thick and makes the joint swollen and puffy to the touch.
As rheumatoid arthritis progresses, the inflamed synovium invades and destroys the cartilage and bone within the joint. The surrounding muscles, ligaments, and tendons that support and stabilize the joint become weak and unable to work normally. These effects lead to the pain and joint damage often seen in rheumatoid arthritis. Researchers studying rheumatoid arthritis now believe that it begins to damage bones during the first year or two that a person has the disease, one reason why early diagnosis and treatment are so important.
Other parts of the body
Some people with rheumatoid arthritis also have symptoms in places other than their joints. Many people with rheumatoid arthritis develop anemia, or a decrease in the production of red blood cells. Other effects that occur less often include neck pain and dry eyes and mouth. Very rarely, people may have inflammation of the blood vessels, the lining of the lungs, or the sac enclosing the heart.
Occurrence and impact
Scientists estimate that about 1.3 million people, or about 0.6% of the US adult population, have rheumatoid arthritis. Interestingly, some recent studies have suggested that although the number of new cases of rheumatoid arthritis for older people is increasing, the overall number of new cases may actually be going down.
Rheumatoid arthritis occurs in all races and ethnic groups. Although the disease often begins in middle age and occurs with increased frequency in older people, children and young adults also develop it. Like some other forms of arthritis, rheumatoid arthritis occurs much more frequently in women than in men. About two to three times as many women as men have the disease.
By all measures, the financial and social impact of all types of arthritis, including rheumatoid arthritis, is substantial, both for the Nation and for individuals. From an economic standpoint, the medical and surgical treatment for rheumatoid arthritis and the wages lost because of disability caused by the disease add up to billions of dollars annually. Daily joint pain is an inevitable consequence of the disease, and most patients also experience some degree of depression, anxiety, and feelings of helplessness. For some people, rheumatoid arthritis can interfere with normal daily activities, limit job opportunities, or disrupt the joys and responsibilities of family life. However, there are arthritis self-management programs that help people cope with the pain and other effects of the disease and help them lead independent and productive lives.
Causes
Scientists still do not know exactly what causes the immune system to turn against itself in rheumatoid arthritis, but research over the last few years has begun to piece together the factors involved.
Genetic (inherited) factors: Scientists have discovered that certain genes known to play a role in the immune system are associated with a tendency to develop rheumatoid arthritis. Some people with rheumatoid arthritis do not have these particular genes; still others have these genes but never develop the disease. These somewhat contradictory data suggest that a person's genetic makeup plays an important role in determining if he or she will develop rheumatoid arthritis, but it is not the only factor. What is clear, however, is that more than one gene is involved in determining whether a person develops rheumatoid arthritis and how severe the disease will become.
Environmental factors: Many scientists think that something must occur to trigger the disease process in people whose genetic makeup makes them susceptible to rheumatoid arthritis. A viral or bacterial infection appears likely, but the exact agent is not yet known. This does not mean that rheumatoid arthritis is contagious: a person cannot catch it from someone else.
Other factors: Some scientists also think that a variety of hormonal factors may be involved. Women are more likely to develop rheumatoid arthritis than men, pregnancy may improve the disease, and the disease may flare after a pregnancy. Breast-feeding may also aggravate the disease. Contraceptive use may alter a person's likelihood of developing rheumatoid arthritis. Scientists think that levels of the immune system molecules interleukin 12 (IL-12) and tumor necrosis factor-alpha (TNF-α) may change along with the changing hormone levels seen in pregnant women. This change may contribute to the swelling and tissue destruction seen in rheumatoid arthritis. These hormones, or possibly deficiencies or changes in certain hormones, may promote the development of rheumatoid arthritis in a genetically susceptible person who has been exposed to a triggering agent from the environment. Even though all the answers are not known, one thing is certain: rheumatoid arthritis develops as a result of an interaction of many factors. Researchers are trying to understand these factors and how they work together.
Diagnosis and treatment
Diagnosing and treating rheumatoid arthritis requires a team effort involving the patient and several types of health care professionals. A person can go to his or her family doctor or internist or to a rheumatologist. A rheumatologist is a doctor who specializes in arthritis and other diseases of the joints, bones, and muscles. As treatment progresses, other professionals often help. These may include nurses, physical or occupational therapists, orthopaedic surgeons, psychologists, and social workers.
Studies have shown that patients who are well informed and participate actively in their own care have less pain and make fewer visits to the doctor than do other patients with rheumatoid arthritis.
Patient education and arthritis self-management programs, as well as support groups, help people to become better informed and to participate in their own care. Self-management programs teach about rheumatoid arthritis and its treatments, exercise and relaxation approaches, communication between patients and health care providers, and problem solving. Research on these programs has shown that they help people:
Diagnosis
Rheumatoid arthritis can be difficult to diagnose in its early stages for several reasons. First, there is no single test for the disease. In addition, symptoms differ from person to person and can be more severe in some people than in others. Also, symptoms can be similar to those of other types of arthritis and joint conditions, and it may take some time for other conditions to be ruled out. Finally, the full range of symptoms develops over time, and only a few symptoms may be present in the early stages. As a result, doctors use a variety of the following tools to diagnose the disease and to rule out other conditions:
Medical history: This is the patient's description of symptoms and when and how they began. Good communication between patient and doctor is especially important here. For example, the patient's description of pain, stiffness, and joint function and how these change over time is critical to the doctor's initial assessment of the disease and how it changes over time.
Physical examination: This includes the doctor's examination of the joints, skin, reflexes, and muscle strength.
Laboratory tests: One common test is for rheumatoid factor, an antibody that is present eventually in the blood of most people with rheumatoid arthritis. (An antibody is a special protein made by the immune system that normally helps fight foreign substances in the body.) Not all people with rheumatoid arthritis test positive for rheumatoid factor, however, especially early in the disease. Also, some people test positive for rheumatoid factor, yet never develop the disease. Other common laboratory tests include a white blood cell count, a blood test for anemia, and a test of the erythrocyte sedimentation rate (often called the sed rate), which measures inflammation in the body. C-reactive protein is another common test that measures disease activity.
X-rays: X-rays are used to determine the degree of joint destruction. They are not useful in the early stages of rheumatoid arthritis before bone damage is evident, but they can be used later to monitor the progression of the disease.
Treatment
Doctors use a variety of approaches to treat rheumatoid arthritis. These are used in different combinations and at different times during the course of the disease and are chosen according to the patient's individual situation. No matter what treatment the doctor and patient choose, however, the goals are the same: to relieve pain, reduce inflammation, slow down or stop joint damage, and improve the person's sense of well-being and ability to function.
Good communication between the patient and doctor is necessary for effective treatment. Talking to the doctor can help ensure that exercise and pain management programs are provided as needed, and that drugs are prescribed appropriately. Talking to the doctor can also help people who are making decisions about surgery.
Goals of treatment
Current treatment approaches
Health behavior changes: Certain activities can help improve a person's ability to function independently and maintain a positive outlook.
Rest and exercise: People with rheumatoid arthritis need a good balance between rest and exercise, with more rest when the disease is active and more exercise when it is not. Rest helps to reduce active joint inflammation and pain and to fight fatigue. The length of time for rest will vary from person to person, but in general, shorter rest breaks every now and then are more helpful than long times spent in bed.
Exercise is important for maintaining healthy and strong muscles, preserving joint mobility, and maintaining flexibility. Exercise can also help people sleep well, reduce pain, maintain a positive attitude, and lose weight. Exercise programs should take into account the person's physical abilities, limitations, and changing needs.
Joint care: Some people find using a splint for a short time around a painful joint reduces pain and swelling by supporting the joint and letting it rest. Splints are used mostly on wrists and hands, but also on ankles and feet. A doctor or a physical or occupational therapist can help a person choose a splint and make sure it fits properly. Other ways to reduce stress on joints include self-help devices (for example, zipper pullers, long-handled shoe horns); devices to help with getting on and off chairs, toilet seats, and beds; and changes in the ways that a person carries out daily activities.
Stress reduction: People with rheumatoid arthritis face emotional challenges as well as physical ones. The emotions they feel because of the disease – fear, anger, and frustration – combined with any pain and physical limitations can increase their stress level. Although there is no evidence that stress plays a role in causing rheumatoid arthritis, it can make living with the disease difficult at times. Stress also may affect the amount of pain a person feels. There are a number of successful techniques for coping with stress. Regular rest periods can help, as can relaxation, distraction, or visualization exercises. Exercise programs, participation in support groups, and good communication with the health care team are other ways to reduce stress.
Healthful diet: With the exception of several specific types of oils, there is no scientific evidence that any specific food or nutrient helps or harms people with rheumatoid arthritis. However, an overall nutritious diet with enough – but not an excess of – calories, protein, and calcium is important. Some people may need to be careful about drinking alcoholic beverages because of the medications they take for rheumatoid arthritis. Those taking methotrexate may need to avoid alcohol altogether because one of the most serious long-term side effects of methotrexate is liver damage.
Climate: Some people notice that their arthritis gets worse when there is a sudden change in the weather. However, there is no evidence that a specific climate can prevent or reduce the effects of rheumatoid arthritis. Moving to a new place with a different climate usually does not make a long-term difference in a person's rheumatoid arthritis.
Medications: Most people who have rheumatoid arthritis take medications. Some medications are used only for pain relief; others are used to reduce inflammation. Still others, often called disease-modifying antirheumatic drugs (DMARDs), are used to try to slow the course of the disease. The person's general condition, the current and predicted severity of the illness, the length of time he or she will take the drug, and the drug's effectiveness and potential side effects are important considerations in prescribing drugs for rheumatoid arthritis. The table below shows currently used rheumatoid arthritis medications, along with their uses and effects, side effects, and monitoring requirements.
Biologic response modifiers are new drugs used for the treatment of rheumatoid arthritis. They can help reduce inflammation and structural damage to the joints by blocking the action of cytokines, proteins of the body's immune system that trigger inflammation during normal immune responses. Three of these drugs, etanercept (Enbrel), infliximab (Remicade), and adalimumab (Humira), reduce inflammation by blocking the reaction of TNF-a molecules. Another drug, called anakinra (Kineret), works by blocking a protein called interleukin 1 (IL-1) that is seen in excess in patients with rheumatoid arthritis.
For many years, doctors initially prescribed aspirin or other pain-relieving drugs for rheumatoid arthritis, as well as rest and physical therapy. They usually prescribed more powerful drugs later only if the disease worsened.
Today, however, many doctors have changed their approach, especially for patients with severe, rapidly progressing rheumatoid arthritis. Studies show that early treatment with more powerful drugs, and the use of drug combinations instead of one medication alone, may be more effective in reducing or preventing joint damage. Once the disease improves or is in remission, the doctor may gradually reduce the dosage or prescribe a milder medication.
Surgery: Several types of surgery are available to patients with severe joint damage. The primary purpose of these procedures is to reduce pain, improve the affected joint's function, and improve the patient's ability to perform daily activities. Surgery is not for everyone, however, and the decision should be made only after careful consideration by patient and doctor. Together they should discuss the patient's overall health, the condition of the joint or tendon that will be operated on, and the reason for, as well as the risks and benefits of, the surgical procedure. Cost may be another factor. Commonly performed surgical procedures include joint replacement, tendon reconstruction, and synovectomy.
Joint replacement: This is the most frequently performed surgery for rheumatoid arthritis, and it is done primarily to relieve pain and improve or preserve joint function. Artificial joints are not always permanent and may eventually have to be replaced. This may be an important consideration for young people.
Tendon reconstruction: Rheumatoid arthritis can damage and even
rupture tendons, the tissues that attach muscle to bone. This surgery,
which is used most frequently on the hands, reconstructs the damaged tendon
by attaching an intact tendon to it. This procedure can help to restore
hand function, especially if the tendon is completely ruptured.
Synovectomy: In this surgery, the doctor actually removes the inflamed
synovial tissue. Synovectomy by itself is seldom performed now because
not all of the tissue can be removed, and it eventually grows back. Synovectomy
is done as part of reconstructive surgery, especially tendon reconstruction.
Routine monitoring and ongoing care: Regular medical care is important to monitor the course of the disease, determine the effectiveness and any negative effects of medications, and change therapies as needed. Monitoring typically includes regular visits to the doctor. It also may include blood, urine, and other laboratory tests and X-rays.
People with rheumatoid arthritis may want to discuss preventing osteoporosis with their doctors as part of their long-term, ongoing care. Osteoporosis is a condition in which bones become weakened and fragile. Having rheumatoid arthritis increases the risk of developing osteoporosis for both men and women, particularly if a person takes corticosteroids. Such patients may want to discuss with their doctors the potential benefits of calcium and vitamin D supplements, hormone therapy, or other treatments for osteoporosis.
Alternative and complementary therapies: Special diets, vitamin supplements, and other alternative approaches have been suggested for treating rheumatoid arthritis. Although many of these approaches may not be harmful in and of themselves, controlled scientific studies either have not been conducted on them or have found no definite benefit to these therapies. Some alternative or complementary approaches may help the patient cope or reduce some of the stress associated with living with a chronic illness. As with any therapy, patients should discuss the benefits and drawbacks with their doctors before beginning an alternative or new type of therapy. If the doctor feels the approach has value and will not be harmful, it can be incorporated into a patient's treatment plan. However, it is important not to neglect regular health care.
Medications: uses, effects, side-effects, monitoring
Analgesics and Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
Analgesics relieve pain; NSAIDs are a large class of medications useful against pain and inflammation. A number of NSAIDs are available over the counter. More than a dozen others – including a subclass called COX-2 inhibitors – are available only with a prescription.
NSAIDs can cause stomach irritation or, less often, can affect kidney function. The longer a person uses NSAIDs, the more likely he or she is to have side effects, ranging from mild to serious. Many other drugs cannot be taken when a patient is being treated with NSAIDs because they alter the way the body uses or eliminates these other drugs. NSAIDs sometimes are associated with serious gastrointestinal problems, including ulcers, bleeding, and perforation of the stomach or intestine. People over age 65 and those with any history of ulcers or gastrointestinal bleeding should use NSAIDs with caution.
Check with your health care provider or pharmacist before you take NSAIDs. Before taking traditional NSAIDs, let your provider know if you drink alcohol or use blood thinners or if you have any of the following: sensitivity or allergy to aspirin or similar drugs, kidney or liver disease, heart disease, high blood pressure, asthma, or peptic ulcers.
Acetaminophen
Nonprescription medications used to relieve pain. Examples are aspirin-free Anacin, Excedrin caplets, Panadol, Tylenol, and Tylenol Arthritis.
Usually no side effects when taken as directed.
Not to be taken with alcohol or with other products containing acetaminophen. Not to be used for more than 10 days unless directed by a physician.
Aspirin
Aspirin is used to reduce pain, swelling, and inflammation, allowing patients to move more easily and carry out normal activities. It is generally part of early and ongoing therapy.
Upset stomach; tendency to bruise easily; ulcers, pain, or discomfort; diarrhea; headache; heartburn or indigestion; nausea or vomiting.
Doctor monitoring is needed.
Traditional NSAIDs: Ibuprofen, Ketoprofen, Naproxen
NSAIDs help relieve pain within hours of administration in dosages available over-the-counter (available for all three medications). They relieve pain and inflammation in dosages available in prescription form (ibuprofen and ketoprofen). It may take several days to reduce inflammation.
For all traditional NSAIDs: Abdominal or stomach cramps, pain, or discomfort; diarrhea; dizziness; drowsiness or light-headedness; headache; heartburn or indigestion; peptic ulcers; nausea or vomiting; possible kidney and liver damage (rare).
For all traditional NSAIDs: Before taking these drugs, let your doctor know if you drink alcohol or use blood thinners or if you have or have had any of the following: sensitivity or allergy to aspirin or similar drugs, kidney or liver disease, heart disease, high blood pressure, asthma, or peptic ulcers.
Corticosteroids
These are steroids given by mouth or injection. They are used to relieve inflammation and reduce swelling, redness, itching, and allergic reactions.
Increased appetite, indigestion, nervousness, or restlessness.
For all corticosteroids, let your doctor know if you have one of the following: fungal infection, history of tuberculosis, underactive thyroid, herpes simplex of the eye, high blood pressure, osteoporosis, or stomach ulcer.
Methylprednisolone/Prednisone
These steroids are available in pill form or as an injection into a joint. Improvements are seen in several hours up to 24 hours after administration. There is potential for serious side effects, especially at high doses. They are used for severe flares and when the disease does not respond to NSAIDs and DMARDs.
Osteoporosis, mood changes, fragile skin, easy bruising, fluid retention, weight gain, muscle weakness, onset or worsening of diabetes, cataracts, increased risk of infection, hyper-tension (high blood pressure).
Doctor monitoring for continued effectiveness of medication and for side effects is needed.
Disease-modifying antirheumatic drugs (DMARDs)
These are common arthritis medications. They relieve painful, swollen joints and slow joint damage, and several DMARDs may be used over the disease course. They take a few weeks or months to have an effect, and may produce significant improvements for many patients. Exactly how they work is still unknown.
Side effects vary with each medicine. DMARDs may increase risk of infection, hair loss, and kidney or liver damage.
Doctor monitoring allows the risk of toxicities to be weighed against the potential benefits of individual medications.
Azathioprine
This drug was first used in higher doses in cancer chemotherapy and organ transplantation. It is used in patients who have not responded to other drugs, and in combination therapy.
Cough or hoarseness, fever or chills, loss of appetite, lower back or side pain, nausea or vomiting, painful or difficult urination, unusual tiredness or weakness.
Before taking this drug, tell your doctor if you use allopurinol or have kidney or liver disease. This drug can reduce your ability to fight infection, so call your doctor immediately if you develop chills, fever, or a cough. Regular blood and liver function tests are needed.
Cyclosporine
This medication was first used in organ transplantation to prevent rejection. It is used in patients who have not responded to other drugs.
Bleeding, tender, or enlarged gums; high blood pressure; increase in hair growth; kidney problems; trembling and shaking of hands.
Before taking this drug, tell your doctor if you have one of the following: sensitivity to castor oil (if receiving the drug by injection), liver or kidney disease, active infection, or high blood pressure. Using this drug may make you more susceptible to infection and certain cancers. Do not take live vaccines while on this drug.
Hydroxychloroquine
It may take several months to notice the benefits of this drug, which include reducing the signs and symptoms of rheumatoid arthritis.
Diarrhea, eye problems (rare), headache, loss of appetite, nausea or vomiting, stomach cramps or pain.
Doctor monitoring is important, particularly if you have an allergy to any antimalarial drug or a retinal abnormality.
Gold sodium thiomalate
This was one of the first DMARDs used to treat rheumatoid arthritis.
Redness or soreness of tongue; swelling or bleeding gums; skin rash or itching; ulcers or sores on lips, mouth, or throat; irritation on tongue. Joint pain may occur for one or two days after injection.
Before taking this drug, tell your doctor if you have any of the following: lupus, skin rash, kidney disease, or colitis. Periodic urine and blood tests are needed to check for side effects.
Leflunomide
This drug reduces signs and symptoms and slows structural damage to joints caused by arthritis.
Bloody or cloudy urine; congestion in chest; cough; diarrhea; difficult, burning, or painful urination or breathing; fever; hair loss; headache; heartburn; loss of appetite; nausea and/or vomiting; skin rash; stomach pain; sneezing; and sore throat.
Before taking this medication, let your doctor know if you have one of the following: active infection, liver disease, known immune deficiency, renal insufficiency, or underlying malignancy. You will need regular blood tests, including liver function tests. Leflunomide must not be taken during pregnancy because it may cause birth defects in humans.
Methotrexate
This drug can be taken by mouth or by injection and results in rapid improvement (it usually takes 3-6 weeks to begin working). It appears to be very effective, especially in combination with infliximab or etanercept. In general, it produces more favorable long-term responses compared with other DMARDs such as sulfasalazine, gold sodium thiomalate, and hydroxychloroquine.
Abdominal discomfort, chest pain, chills, nausea, mouth sores, painful urination, sore throat, unusual tiredness or weakness.
Doctor monitoring is important, particularly if you have an abnormal blood count, liver or lung disease, alcoholism, immune-system deficiency, or active infection. Methotrexate must not be taken during pregnancy because it may cause birth defects in humans.
Sulfasalazine
This drug works to reduce the signs and symptoms of rheumatoid arthritis by suppressing the immune system.
Abdominal pain, aching joints, diarrhea, headache, sensitivity to sunlight, loss of appetite, nausea or vomiting, skin rash.
Doctor monitoring is important, particularly if you are allergic to sulfa drugs or aspirin, or if you have a kidney, liver, or blood disease.
Biologic response modifiers
These drugs selectively block parts of the immune system called cytokines. Cytokines play a role in inflammation. Long-term efficacy and safety are uncertain.
Increased risk of infection, especially tuberculosis. Increased risk of pneumonia, and listeriosis (a foodborne illness caused by the bacterium Listeria monocytogenes).
It is important to avoid eating undercooked foods (including unpasteurized cheeses, cold cuts, and hot dogs) because undercooked food can cause listeriosis for patients taking biologic response modifiers.
Tumor necrosis factor Inhibitors: Etanercept, Infliximab, Adalimumab
These medications are highly effective for treating patients with an inadequate response to DMARDs. They may be prescribed in combination with some DMARDs, particularly methotrexate. Etanercept requires subcutaneous (beneath the skin) injections two times per week. Infliximab is taken intravenously (IV) during a 2-hour procedure. It is administered with methotrexate. Adalimumab requires injections every 2 weeks. Long-term efficacy and safety are uncertain.
Etanercept: Pain or burning in throat; redness, itching, pain, and/or swelling at injection site; runny or stuffy nose. Infliximab: Abdominal pain, cough, dizziness, fainting, headache, muscle pain, runny nose, shortness of breath, sore throat, vomiting, wheezing. Adalimumab: Redness, rash, swelling, itching, bruising, sinus infection, headache, nausea.
Long-term efficacy and safety are uncertain. Doctor monitoring is important, particularly if you have an active infection, exposure to tuberculosis, or a central nervous system disorder. Evaluation for tuberculosis is necessary before treatment begins.
Interleukin1 Inhibitor: Anakinra
This medication requires daily injections. Long-term efficacy and safety are uncertain.
Redness, swelling, bruising, or pain at the site of injection; head-ache; upset stomach; diarrhea; runny nose; and stomach pain.
Doctor monitoring is required.


