osteoporosis
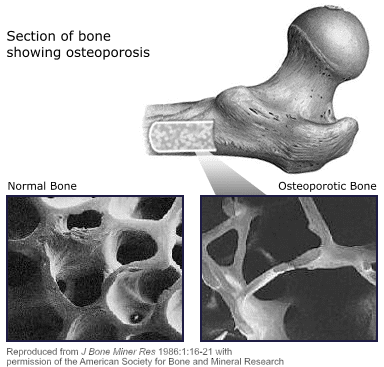
Osteoporosis is a disease characterized by low bone mass and structural deterioration of bone tissue, leading to bone fragility and an increased risk of fractures of the hip, spine, and wrist. Men as well as women are affected by osteoporosis, a disease that can be prevented and treated.
Osteoporosis is not the same as osteomalacia, which is demineralization of bone due to vitamin D deficiency. However, the two conditions may be present simultaneously, causing severe bone weakness.
Osteoporosis is a natural part of aging. By the age of 70, bone density of the skeleton has typically fallen by about one third. For hormonal reasons, significant osteoporosis is much more common in women than in men. Also, for reasons unknown, black people are less affected than white people or Asians.
Prevention
To reach optimal peak bone mass and continue building new bone tissue as you age, you should consider several factors.
Calcium
An inadequate supply of calcium over a lifetime contributes to the development of osteoporosis. Many published studies show that low calcium intake appears to be associated with low bone mass, rapid bone loss, and high fracture rates. Nutrition surveys show that many people consume less than half the amount of calcium recommended to build and maintain healthy bones. Good sources of calcium include low-fat dairy products, such as milk, yogurt, cheese, and ice cream; dark green, leafy vegetables, such as broccoli, collard greens, bok choy, and spinach; sardines and salmon with bones; tofu; almonds; and foods fortified with calcium, such as orange juice, cereals, and breads. Depending upon how much calcium you get each day from food, you may need to take a calcium supplement.
Calcium needs change during one's lifetime. The body's demand for calcium is greater during childhood and adolescence, when the skeleton is growing rapidly, and during pregnancy and breast-feeding. Postmenopausal women and older men also need to consume more calcium. Also, as you age, your body becomes less efficient at absorbing calcium and other nutrients. Older adults also are more likely to have chronic medical problems and to use medications that may impair calcium absorption.
Vitamin D
Vitamin D plays an important role in calcium absorption and in bone health. It is made in the skin through exposure to sunlight. While many people are able to obtain enough vitamin D naturally, studies show that vitamin D production decreases in the elderly, in people who are housebound, and for people in general during the winter. Depending on your situation, you may need to take vitamin D supplements to ensure a daily intake of between 400 to 800 IU of vitamin D. Massive doses are not recommended.
Exercise
Like muscle, bone is living tissue that responds to exercise by becoming stronger. Weight-bearing exercise is the best for your bones because it forces you to work against gravity. Examples include walking, hiking, jogging, stair climbing, weight training, tennis, and dancing.
Smoking and drinking
Smoking is bad for your bones as well as for your heart and lungs. Women who smoke have lower levels of estrogen compared to nonsmokers, and they often go through menopause earlier. Smokers also may absorb less calcium from their diets.
Regular consumption of 2 to 3 oz a day of alcohol may be damaging to the skeleton, even in young women and men. Those who drink heavily are more prone to bone loss and fractures, because of both poor nutrition and increased risk of falling.
Medications that cause bone loss
The long-term use of glucocorticoids (medications prescribed for a wide range of diseases, including arthritis, asthma, Crohn's disease, lupus, and other diseases of the lungs, kidneys, and liver) can lead to a loss of bone density and fractures. Bone loss can also result from long-term treatment with certain antiseizure drugs, such as phenytoin (Dilantin) and barbiturates; gonadotropin-releasing hormone (GnRH) drugs used to treat endometriosis; excessive use of aluminum-containing antacids; certain cancer treatments; and excessive thyroid hormone. It is important to discuss the use of these drugs with your physician and not to stop or change your medication dose on your own.
Symptoms
Osteoporosis is often called the "silent disease" because bone loss occurs without symptoms. People may not know that they have osteoporosis until their bones become so weak that a sudden strain, bump, or fall causes a hip to fracture or a vertebra to collapse. Collapsed vertebrae may initially be felt or seen in the form of severe back pain, loss of height, or spinal deformities such as kyphosis (severely stooped posture).
Detection
Following a comprehensive medical assessment, your doctor may recommend that you have your bone mass measured. A bone mineral density (BMD) test is the best way to determine your bone health. BMD tests can identify osteoporosis, determine your risk for fractures (broken bones), and measure your response to osteoporosis treatment. The most widely recognized bone mineral density test is called a dual-energy X-ray absorptiometry or DXA test. It is painless – a bit like having an X-ray – but with much less exposure to radiation. It can measure bone density at your hip and spine.
Bone density tests can:
Treatment
A comprehensive osteoporosis treatment program includes a focus on proper nutrition, exercise, and safety issues to prevent falls that may result in fractures. In addition, your physician may prescribe a medication to slow or stop bone loss, increase bone density, and reduce fracture risk.
Nutrition
The foods we eat contain a variety of vitamins, minerals, and other important nutrients that help keep our bodies healthy. All of these nutrients are needed in balanced proportion. In particular, calcium and vitamin D are needed for strong bones, and for your heart, muscles, and nerves to function properly.
Exercise
Exercise is an important component of an osteoporosis prevention and treatment program. Exercise not only improves your bone health, but it increases muscle strength, coordination, and balance, and leads to better overall health. While exercise is good for someone with osteoporosis, it should not put any sudden or excessive strain on your bones. As extra insurance against fractures, your doctor can recommend specific exercises to strengthen and support your back.
Therapeutic medications
Currently, alendronate, raloxifene, risedronate, and ibandronate are approved by the U. S. Food and Drug Administration (FDA) for preventing and treating postmenopausal osteoporosis. Teriparatide is approved for treating the disease in postmenopausal women and men at high risk for fracture. Estrogen/hormone therapy (ET/HT) is approved for preventing postmenopausal osteoporosis, and calcitonin is approved for treatment.
Alendronate, risedronate, and zoledronic acid have been shown to increase bone mass and reduce the incidence of spine, hip, and other fractures. Ibandronate has been shown to reduce the incidence of spine fractures.
Alendronate is available in daily and weekly doses. Risedronate is available in daily, weekly, and twice monthly doses. Ibandronate is available in a monthly dose and as an intravenous injection administered once every three months. Zoledronic acid is available as an intravenous injection administered once yearly.
Side effects for oral bisphosphonates include gastrointestinal problems such as difficulty swallowing, inflammation of the esophagus, and peptic ulcer.
Side effects for intravenous bisphosphonates include flu-like symptoms, fever, pain in muscles or joints, and headache. These side effects can occur shortly after receiving an infusion and generally stop within two to three days.
There have also been rare reports of osteonecrosis of the jaw and of visual disturbances in people taking oral and intravenous bisphosphonates.
Some bisphosphonates are marketed with calcium and vitamin D supplements. These nutrients are important for everyone, and people should include adequate amounts of them in their diets.
The Women's Health Initiative, a large Government-funded research study, recently demonstrated that the drug Prempro (estrogen combined with progestin), which is used in hormone therapy, is associated with a modest increase in the risk of breast cancer, stroke, and heart attack. The WHI also demonstrated that in patients who had a hysterectomy, estrogen therapy alone was associated with an increase in the risk of stroke, but not of breast cancer or cardiovascular disease. A large study from the National Cancer Institute indicated that long-term use of estrogen therapy may be associated with an increased risk of ovarian cancer.
Estrogen therapy is approved for treatment of menopausal symptoms but should be prescribed for the shortest period of time possible. When used solely for the prevention of postmenopausal osteoporosis, any ET/HT regimen should only be considered for women at significant risk of osteoporosis, and nonestrogen medications should be carefully considered first.
Fall prevention
Preventing falls is a special concern for men and women with osteoporosis. Falls can increase the likelihood of fracturing a bone in the hip, wrist, spine, or other part of the skeleton. In addition to the environmental factors listed below, falls can also be caused by impaired vision and/or balance, chronic diseases that affect mental or physical functioning, and certain medications, such as sedatives and antidepressants. It is important that individuals with osteoporosis be aware of any physical changes that affect their balance or gait, and that they discuss these changes with their health care provider. Here are some tips to help eliminate the environmental factors that lead to falls.
Outdoors:
Indoors:


