catheter ablation
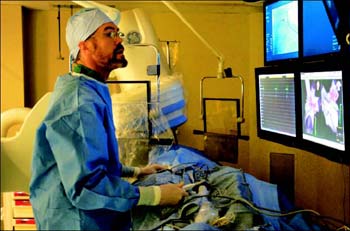
Catheter ablation procedure.
Catheter ablation is a medical procedure used to treat some types of arrhythmia. An arrhythmia is a problem with the speed or rhythm of the heartbeat.
During catheter ablation, a long, thin, flexible tube is put into a blood vessel in the patient's arm, groin (upper thigh), or neck. This tube is called an ablation catheter. It's then guided to the heart through the blood vessel. A special machine sends energy through the catheter to the heart. This energy finds and destroys small areas of heart tissue where abnormal heartbeats may cause an arrhythmia to start.
Overview
The heart's electrical system controls the speed and rhythm of the heartbeat. With each heartbeat, an electrical signal spreads from the top of the heart to the bottom. As it travels, the electrical signal causes the heart to contract and pump blood.
The process repeats with each new heartbeat. A problem with any part of this process can cause an arrhythmia.
Catheter ablation is one of several treatments for arrhythmia. A doctor may recommend it if:
Though few, catheter ablation has risks. These include bleeding, infection, and pain where the catheter is inserted. More serious problems include blood clots and puncture of the heart.
Cardiologists (doctors who specialize in treating people with heart problems) sometimes perform ablation through open-heart surgery. But this method is not as common as catheter ablation, which doesn't require surgery to open the chest cavity.
Outlook
Catheter ablation alone doesn't always restore a normal heart rate and rhythm. Other treatments may need to be used as well. Also, some people who have the procedure may need to have it done again. This can happen when the first procedure doesn't fully correct the problem.
Who needs catheter ablation?
A doctor may recommend catheter ablation if the patient:
Before catheter ablation
Before having catheter ablation, a patient should discuss with his/her doctor:
Some people go home the same day as the procedure. Others need to stay overnight for one or more days. Driving after the procedure may not be safe.
During catheter ablation
Catheter ablation is done in a hospital. Doctors who do this procedure have special training in cardiac electrophysiology (the electrical system of the heart) and ablation (destruction) of diseased heart tissue.
At the start
Before the procedure, the patient is given medicine through an intravenous (IV) line inserted in a vein in the arm. The medicine helps to the patient relax and may make him/her sleepy. The patient is also connected to several machines that check the heart's activity during the procedure.
Once the patient is drowsy, an area on the patient's arm, groin (upper thigh), or neck is numbed. This is where the ablation catheter (a long, thin, flexible tube) will be inserted into a blood vessel. A needle is used to make a small hole through the skin into the blood vessel. A tapered tube called a sheath is put through this hole.
A thin, flexible wire and the catheter is then put through the sheath and into the blood vessel. This guide wire is threaded through the blood vessel to the heart. The wire helps the catheter to be placed correctly.
Special X-ray movies are taken of the guide wire and the catheter as they are moved into the heart. The movies help the doctor see where to place the tip of the catheter.
During the procedure
Electrodes at the end of the catheter are used to stimulate the heart and record its electrical activity. This helps establish where abnormal heartbeats are starting in your heart.
The catheter is moved so that its tip is aimed at the small area of heart tissue where the abnormal heartbeat is starting. A special machine sends energy through the catheter to destroy this very small area of heart tissue.
Types of energy used include radio-frequency (heat generated by electrodes), laser, or cryo- (very cold temperatures).
What the patient may feel
The patient may sleep on and off during the procedure and will generally not feel anything except for:
The procedure lasts 3 to 6 hours. When the procedure is done, the ablation catheter will be pulled back and taken out along with the sheath and guide wire. The opening left in the blood vessel is closed and bandaged. Nurses apply pressure to this site to help prevent major bleeding and to help the site begin to heal.
After catheter ablation
After the procedure, the patient is moved to a special care unit where he/she lies still for 4 to 6 hours of recovery. Lying still prevents bleeding at the site where the catheter was inserted.
While the patient is in the special care unit, he/she is connected to special devices that measure the heart's electrical activity and blood pressure. Nurses check these monitors continuously and also check to make sure that there's no bleeding at the catheter insertion site.
Going home
A doctor determines whether the patient needs to stay overnight in the hospital. Some people go home the same day. Others need to stay overnight for 1 or more days.
Before the patient's, he/she is informed by the doctor:
Driving after the procedure may not be safe. The patient will be informed if they needs to arrange for someone to drive them home.
Recovery and recuperation
Recovery from catheter ablation is usually quick. The patient may feel stiff and achy from lying still for 4 to 6 hours after the procedure. In addition, a small bruise may form at the site where the ablation catheter was inserted. The area may feel sore or tender for about a week. Most people are able to return to normal activity in a few days.
The doctor will give information about signs and symptoms to watch for. The patient should tell the doctor if he/she has problems such as:
Risks
Though few, catheter ablation does have risks. Possible problems are:
As with any heart procedure, complications can sometimes, although rarely, be fatal. The risk of complications is higher if the patient has diabetes or kidney disease. It also is higher if the patient is 75 years old or older.


