heart

Front view of human heart. The pericardium has been removed, except for the edges around the blood vessels at the top. The blue arrows show the way blood is brought to the heart by the vena cavae, passes through the right atrium and ventricle, and then out through the pulmonary artery.

Rear view of human heart. The red arrows show how oxygenated blood arrives at the left atrium, passes into the left ventricle, and is then pumped out of the heart into the aorta.
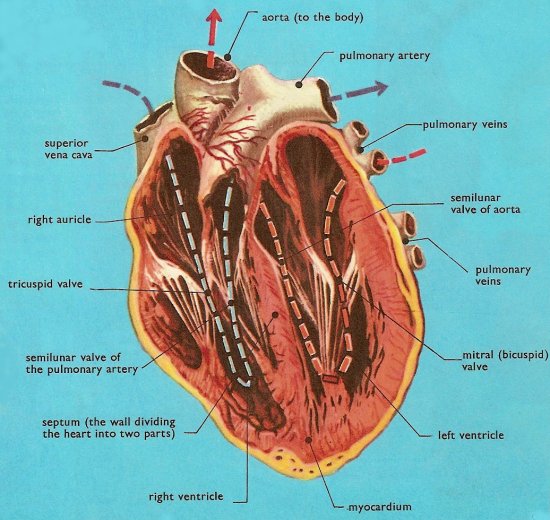
Cross-section of heart, as seen from the front. This illustration shows the cords or heart-strings which hold the mitral and tricuspid valves in their correct position. The semilunar valves are inside the small portions of the aorta and pulmonary artery which lie within the heart.
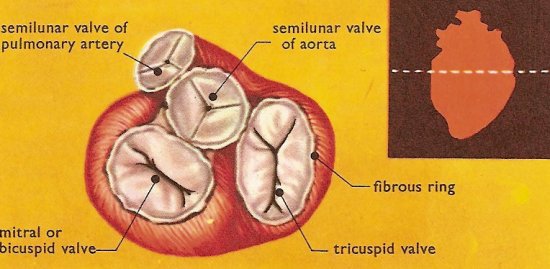
Section across the heart to show the valves. The figure inset shows the level at which the section is made.

Location of human heart.
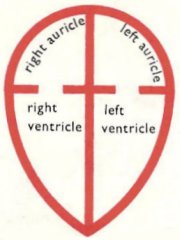
Compartments of the heart.
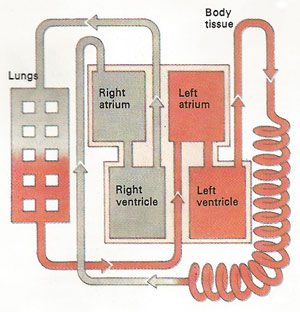
The heart is a dual-purpose pump. In the space of a single beat, blood is pumped from the eft to the systemic circulation and from the right to the pulmonary circuition for recycling.
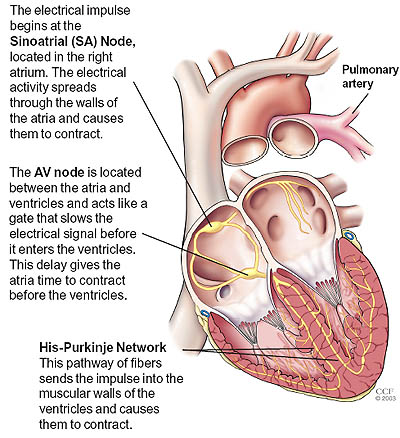
Image credit: Cleveland Clinic Foundation.
The heart is a muscular pump that circulates the blood. An adult human heart weighs between 200 and 425 grams (7 and 15 ounces) and is slightly larger than a fist. In an average lifetime, a person's heart may beat more than 3.5 billion times. Each day, the average heart beats 100,000 times, pumping about 7,600 liters (2,000 galons) of blood.
Location of the heart
The heart is located between the lungs in the middle of the chest, behind and slightly to the left of the sternum (breastbone) and in front of the spine. Because the heart is not central, but lies to the left of the center line, the heart beat is best felt on the left side of the chest. To make room for it, the left lung is rather smaller than the left.
Pericardium
A double-layered membrane called the pericardium surrounds the heart like a sac. The outer layer of the pericardium surrounds the roots of the heart's major blood vessels and is attached by ligaments to the spinal column, diaphragm, and other parts of the body. The inner layer of the pericardium is attached to the heart muscle. A coating of fluid separates the two layers of membrane, letting the heart move as it beats, yet still be attached to the body.
Layers of the heart wall
Three layers of tissue form the heart wall. The outer layer of the heart wall is the epicardium, the middle layer is the myocardium, and the inner layer is the endocardium.
The walls of the heart are largely made from myocardium, which is a special kind of muscle tissue. This muscle is so constructed that it is able to perform the 60 to 70 contractions which the healthy adult human heart undergoes every minute. On the inside this muscle is provided with a lining of flat cells called the endocardium, which is direct contact with the blood within the heart.
Chambers of the heart
The human heart has four chambers. The upper chambers are called the left and right atria, and the lower chambers are called the left and right ventricles. A wall of muscle called the septum separates the left and right atria and the left and right ventricles.
The two atria are thin-walled chambers that receive blood from the veins: the right atrium receives deoxygenated blood from systemic veins, while the left atrium receives oxygenated blood from the pulmonary veins. The two ventricles are thick-walled chambers that forcefully pump blood out of the heart. Differences in thickness of the heart chamber walls are due to variations in the amount of myocardium present, which reflects the amount of force each chamber is required to generate. The left ventricle is the largest and strongest chamber. The left ventricle's chamber walls are only about a half-inch thick, but they have enough force to push blood through the aortic valve and into the body.
Heart valves
The heart has two types of valves that keep the blood flowing in the correct direction. The valves between the atria and ventricles are called atrioventricular valves (also called cuspid valves), while those at the bases of the large vessels leaving the ventricles are called semilunar valves.
The right atrioventricular valve is the tricuspid valve. The left atrioventricular valve is the mitral valve (also called the bicuspid valve). The valve between the right ventricle and pulmonary trunk is the pulmonary valve. The valve between the left ventricle and the aorta is the aortic valve. Both the pulmonary and aortic valves are semilunar valves
When the ventricles contract, atrioventricular valves close to prevent blood from flowing back into the atria. When the ventricles relax, semilunar valves close to prevent blood from flowing back into the ventricles.
To summarize:
Pathway of blood through the heart
While it is convenient to describe the flow of blood through the right side of the heart and then through the left side, it is important to realize that both atria contract at the same time and both ventricles contract at the same time. The heart works as two pumps, one on the right and one on the left, working simultaneously. Blood flows from the right atrium to the right ventricle, and then is pumped to the lungs to receive oxygen. From the lungs, the blood flows to the left atrium, then to the left ventricle. From there it is pumped to the systemic circulation.
Blood supply to the myocardium
The myocardium of the heart wall is a working muscle that needs a continuous supply of oxygen and nutrients to function with efficiency. For this reason, cardiac muscle has an extensive network of blood vessels to bring oxygen to the contracting cells and to remove waste products.
The right and left coronary arteries, branches of the ascending aorta, supply blood to the walls of the myocardium. After blood passes through the capillaries in the myocardium, it enters a system of cardiac (coronary) veins. Most of the cardiac veins drain into the coronary sinus, which opens into the right atrium.
Conduction system
An effective cycle for productive pumping of blood requires that the heart be synchronized accurately. Both atria need to contract simultaneously, followed by contraction of both ventricles. Specialized cardiac muscle cells that make up the conduction system of the heart coordinate contraction of the chambers.
The conduction system includes several components. The first part of the conduction system is the sinoatrial (SA) node, located in the myocardium at the top of the right atrium. Without any neural stimulation, the sinoatrial node rhythmically initiates electrical impulses 70 to 80 times per minute. Because it establishes the basic rhythm of the heartbeat, it is called the heart's natural pacemaker. Each electrical impulse from the SA node travels through the muscle fibers of the atria and ventricles, causing them to contract. Other parts of the conduction system include the atrioventricular (AV) node, atrioventricular bundle, bundle branches, and conduction myofibers. All these components coordinate the contraction and relaxation of the heart chambers. Although the SA node sends electrical impulses at a certain rate, your heart rate may still change depending on physical demands, stress, or hormonal factors.
See also heart electrical system.
Cardiac cycle
The cardiac cycle refers to the alternating contraction and relaxation of the myocardium in the walls of the heart chambers, coordinated by the conduction system, during one heartbeat. Systole is the contraction phase of the cardiac cycle, and diastole is the relaxation phase. At a normal heart rate, one cardiac cycle lasts for 0.8 second.
Heart sounds
The sounds associated with the heartbeat are due to vibrations in the tissues and blood caused by closure of the valves. Abnormal heart sounds are called murmurs.
Heart rate
The sinoatrial node, acting alone, produces a constant rhythmic heart rate. Regulating factors are reliant on the atrioventricular node to increase or decrease the heart rate to adjust cardiac output to meet the changing needs of the body. Most changes in the heart rate are mediated through the cardiac center in the medulla oblongata of the brain. The center has both sympathetic and parasympathetic components that adjust the heart rate to meet the changing needs of the body.
Peripheral factors such as emotions, ion concentrations, and body temperature may affect heart rate. These are usually mediated through the cardiac center.



