cardiomyopathy
Cardiomyopathy is any of several disease of the heart muscle. These diseases have a variety of causes, symptoms, and treatments. In cardiomyopathy, the heart muscle becomes enlarged or abnormally thick or rigid. In rare cases, the muscle tissue in the heart is replaced with scar tissue.
As cardiomyopathy progresses, the heart becomes weaker and less able to pump blood through the body. This can lead to heart failure, arrhythmias (abnormal heart rhythms), fluid buildup in the lungs or legs, and, more rarely, endocarditis (a bacterial infection of the lining of the heart). The weakening of the heart also can lead to other severe complications.
The three main types of cardiomyopathy are:
A rare, genetic type of cardiomyopathy is arrhythmogenic ventricular dysplasia (ARVD).
Cardiomyopathy can have a specific cause, such as damage to the heart from a heart attack, high blood pressure, or a viral infection. Some types of cardiomyopathy are caused by a gene mutation and run in families. In many cases, the cause is unknown.
Cardiomyopathy can affect people of all ages, from babies to older adults. However, certain age groups are more likely to have certain types of cardiomyopathy. Treatment may involve medicines, surgery, nonsurgical procedures, and lifestyle changes.
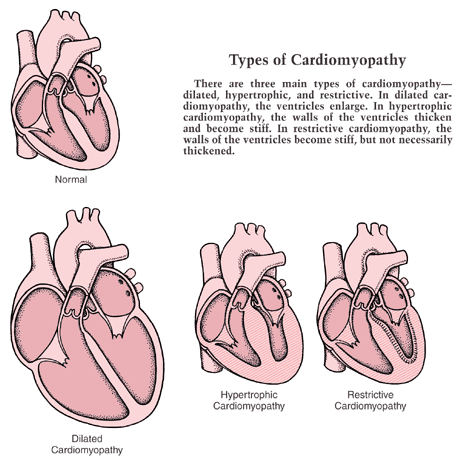
Types of cardiomyopathy
Dilated cardiomyopathy
Dilated cardiomyopathy is the most common form of cardiomyopathy. It generally occurs in adults aged 20 to 60 years. Men are more likely than women to develop dilated cardiomyopathy.
Dilated cardiomyopathy affects the heart's ventricles and atria. The ventricles are the two lower chambers of the heart, and the atria are the two upper chambers. Dilated cardiomyopathy usually starts in the left ventricle, where the heart muscle begins to dilate or stretch and become thinner. This leads to enlargement of the inside of the ventricle. The problem often spreads to the right ventricle and then to the atria as the disease gets worse.
When the chambers dilate, the heart can't pump blood very well. The heart tries to cope by dilating the chambers even more. Over time, the heart becomes weaker and heart failure can occur. Symptoms of heart failure include feeling tired, swelling of the legs and feet, and shortness of breath. Dilated cardiomyopathy also can lead to heart valve problems, arrhythmias, and blood clots in the heart. Having advanced dilated cardiomyopathy is a common reason for needing a heart transplant.
Up to one-half of all cases of dilated cardiomyopathy may be hereditary (passed down in the genes from parent to child). These cases are called familial dilated cardiomyopathy. Dilated cardiomyopathy also can be a complication of many conditions, including coronary artery disease and high blood pressure. It also can be caused by viral infections, excessive use of alcohol, and exposure to certain drugs (including cocaine, amphetamines, and some drugs used in cancer treatments). In some cases, no cause can be found.
Hypertrophic cardiomyopathy
Hypertrophic cardiomyopathy occurs when the heart muscle thickens abnormally. The thickening generally happens in the left ventricle, the heart's main pumping chamber. This type of cardiomyopathy can affect people of any age.
Hypertrophic cardiomyopathy can be obstructive or nonobstructive. In the obstructive type, the septum (the wall that divides the left and right sides of the heart) thickens and bulges into the left ventricle. This bulge blocks the flow of blood out of the ventricle. The ventricle must work much harder to pump blood past the blockage and out to the body. Symptoms can include chest pain, dizziness, shortness of breath, or fainting.
Obstructive hypertrophic cardiomyopathy also can affect the heart's mitral valve, causing blood to leak backward through the valve.
In nonobstructive hypertrophic cardiomyopathy, the thickened heart muscle does not block the flow of blood out of the ventricle. The entire ventricle may become thicker (symmetric ventricular hypotrophy) or it may happen only at the bottom of the heart (apical hypertrophy). The right ventricle also may be affected.
In both kinds of hypertrophic cardiomyopathy, the thickened muscle makes the inside of the left ventricle smaller so that it holds less blood. The walls of the ventricles also may become stiff. As a result, they are less able to relax and fill with blood. This causes increased pressure in the ventricles and the blood vessels of the lungs. Changes also occur to the cells in the damaged heart muscle. This may interfere with the heart's electrical signals, leading to arrhythmias.
Some people with hypertrophic cardiomyopathy have no symptoms, and the condition does not affect their lives. Others have severe symptoms or develop complications such as serious arrhythmias. A few people with the condition have sudden cardiac arrest because of dangerous arrhythmias.
Hypertrophic cardiomyopathy can be inherited because of a gene mutation or develop over time because of high blood pressure or aging. Often, the cause is unknown.
Restrictive cardiomyopathy
Restrictive cardiomyopathy tends to mostly affect older adults. In this cardiomyopathy, the ventricles become stiff and rigid due to replacement of the normal heart muscle with abnormal tissue, such as scar tissue. As a result, the ventricles cannot relax normally and expand to fill with blood, which causes the atria to become enlarged. Eventually, blood flow in the heart is reduced, and complications such as heart failure or arrhythmias occur.
Restrictive cardiomyopathy can occur for no known reason, or it can develop because the person has another disease. Some of the diseases that can cause restrictive cardiomyopathy include hemochromatosis, sarcoidosis, amyloidosis, and connective tissue disorders. Restrictive cardiomyopathy also can occur as a result of radiation treatments, infections, or scarring after surgery.
Arrhythmogenic right ventricular dysplasia
Arrhythmogenic right ventricular dysplasia (ARVD) is a rare type of cardiomyopathy. ARVD develops when the muscle tissue in the right ventricle dies and is replaced with scar tissue. This process causes problems in the heart's electrical signaling, resulting in arrhythmias. Symptoms include a feeling of strong or irregular heartbeats (palpitations) and fainting after exercise.
ARVD usually develops in teens or young adults and is often the cause of sudden cardiac death in young athletes. ARVD is thought to be an inherited disease.
Causes
Many times, the cause of cardiomyopathy is unknown. When this happens, the disease is called idiopathic (or primary) cardiomyopathy. The majority of cardiomyopathies in children are idiopathic.
Sometimes, cardiomyopathy is inherited (passed down in the genes from parent to child) or caused by another disease or condition.
Dilated cardiomyopathy
Dilated cardiomyopathy can be inherited. It also can be caused by certain diseases, conditions, and substances, including:
Hypertrophic cardiomyopathy
Hypertrophic cardiomyopathy can be inherited. It also can develop over time because of high blood pressure or aging. Often, the cause of hypertrophic cardiomyopathy is unknown.
Restrictive cardiomyopathy
Certain diseases and conditions can cause restrictive cardiomyopathy, including:
Arrhythmogenic right ventricular dysplasia
Arrythmogenic right ventricular dysplasia is thought to be an inherited disease.
Who is at risk for cardiomyopathy?
Populations affected
People of all ages can develop cardiomyopathy, but certain cardiomyopathies are more common in certain groups:
Major risk factors
Major risk factors for developing cardiomyopathy include:
- A previous heart attack
- Myocarditis
Some people with cardiomyopathy never have symptoms. That is why it's important to identify people who may be at high risk for this disease so that potential problems (such as serious arrhythmias or sudden cardiac death) can be prevented.
Signs and symptoms
Some people with cardiomyopathy never have symptoms, and others have no symptoms in the early stages of the disease. As cardiomyopathy progresses and the heart weakens, signs and symptoms of heart failure usually appear. These signs and symptoms include:
Other signs and symptoms can include dizziness, lightheadedness, fainting during exercise, abnormal heart rhythms (arrhythmias), and an extra or unusual sound heard during the heartbeat (heart murmur).
Diagnosis
If cardiomyopathy is suspected, the diagnosis is based on a person's:
The physical exam will identify a number of findings in patients with cardiomyopathy. The doctor will use a stethoscope to listen to the person's heart and lungs for sounds that may suggest the presence of cardiomyopathy. These sounds may even indicate a certain type of cardiomyopathy. For example, the loudness, timing, and location of a heart murmur may suggest that a person has hypertrophic obstructive cardiomyopathy. A "crackling" sound in the lungs may be a sign of heart failure, which often develops in the later stages of cardiomyopathy.
Physical signs also help the doctor diagnose cardiomyopathy. Swelling of the abdomen, legs, or feet may indicate excess fluid, which is a sign of heart failure. Sometimes, doctors discover cardiomyopathy during a routine exam if they hear a heart murmur or if the patient has an abnormal electrocardiogram (see Diagnostic tests and procedures below).
Specialists involved
Often a cardiologist or pediatric cardiologist is involved in the care of a patient with cardiomyopathy. A cardiologist is a doctor who specializes in heart diseases. A pediatric cardiologist specializes in children's heart diseases.
Diagnostic tests and procedures
Doctors may order one or more tests to diagnose cardiomyopathy, including:
There are several different types of echocardiograms, including a stress echocardiogram. During this test, an echocardiogram is done both before and after your heart is stressed either by having you exercise or by injecting a medicine into your bloodstream that makes your heart beat faster and work harder. A stress echocardiogram is usually done to find out if you have decreased blood flow to your heart (coronary artery disease). Echocardiogram is a good way to diagnose hypertrophic cardiomyopathy because it shows the thickened walls of the heart.
During exercise stress testing, your blood pressure and EKG readings are monitored while you walk or run on a treadmill or pedal a bicycle. Other heart tests, such as nuclear heart scanning or echocardiography, also can be done at the same time. These would be ordered if your doctor needs more information than the exercise stress test can provide about how well your heart is working.
If you are unable to exercise, a medicine can be injected through an intravenous line (IV) into your bloodstream to make your heart work harder and beat faster, as if you are exercising on a treadmill or bicycle. Nuclear heart scanning or echocardiography is then usually done. During nuclear heart scanning, radioactive tracer is injected into your bloodstream, and a special camera shows the flow of blood through your heart and arteries. Echocardiography uses sound waves to show blood flow through the chambers and valves of your heart and to show the strength of your heart muscle.
Your doctor also may order two newer tests along with stress testing if more information is needed about how well your heart works. These new tests are magnetic resonance imaging (MRI) and positron emission tomography (PET) scanning of the heart. MRI shows detailed images of the structures and beating of your heart, which may help your doctor better assess if parts of your heart are weak or damaged. PET scanning shows the level of chemical activity in different areas of your heart. This can help your doctor determine if enough blood is flowing to the areas of your heart. A PET scan can show decreased blood flow caused by disease or damaged muscles that may not be detected by other scanning methods.
The doctor may order additional tests to confirm the diagnosis or if surgery is planned. These tests may include:
Because some types of cardiomyopathy run in families, the doctor may recommend looking for the disease in the parents, brothers and sisters, and children of people with cardiomyopathy.
Genetic counseling may be recommended. Genetic counseling is useful to help define and explain how the disease runs in families and to determine the chances of parents passing it on to their children.
Treatment
Not everyone with cardiomyopathy needs treatment. People who have no symptoms may not need treatment. In some cases, dilated cardiomyopathy that comes on suddenly may even go away on its own. For other people with cardiomyopathy, treatment is necessary.
Specific treatments depend on the type of cardiomyopathy, how severe the symptoms and complications are, and the age and overall health of the person.
Goals of treatment
The main goals of treating cardiomyopathy are to:
Specific types of treatment
Treatments for cardiomyopathy may include medicines, surgery, nonsurgical procedures, and lifestyle changes.
Medicines
A number of medicines may be used to treat cardiomyopathy, including:
Surgery
Doctors can use several different types of surgery to treat cardiomyopathy, including removing part of the enlarged heart muscle (septal myectomy) and implanting devices that help the heart beat more effectively. Heart transplant is sometimes used in cases of severe heart failure.
Septal myectomy. Septal myectomy (also called septal myomectomy) is open-heart surgery for people with hypertrophic obstructive cardiomyopathy and severe symptoms. It is generally used in younger patients and when medicines aren't working well.
In septal myectomy, a surgeon removes part of the thickened septum that is bulging into the left ventricle. This widens the pathway in the ventricle that leads to the aortic valve and improves blood flow through the heart and out to the body. The tissue that is removed does not grow back. If necessary, the mitral valve can be repaired or replaced at the same time. This surgery is often successful, and the person can return to a normal life with no symptoms.
Surgically implanted devices. Surgeons can place several different types of devices in the heart to help it beat more effectively. One device is a pacemaker, which electronically helps maintain normal heart rhythm. Sometimes, doctors choose to use a biventricular pacemaker, which coordinates contractions between the heart's left and right ventricles.
A left ventricular assist device (LVAD) helps the heart pump blood to the body. LVAD can be used as a long-term therapy or as a short-term treatment for people who are waiting for a heart transplant.
An implantable cardioverter defibrillator (ICD) is used in people who are at risk of life-threatening arrhythmia or sudden cardiac death. This small device is implanted in the chest and connected to the heart with wires. If the ICD senses a dangerous change in heart rhythm, it will send an electric shock to the heart to restore a normal heartbeat.
Heart transplant. In this surgery, a doctor replaces a person's diseased heart with a healthy heart from a person who has recently died. It is a last resort for people with heart failure when all other treatments have failed.
Nonsurgical procedure
Alcohol septal ablation. In this procedure, a doctor injects ethanol (a type of alcohol) through a catheter into the small artery that supplies blood to the thickened area of heart muscle. The alcohol kills the cells and the thickened tissue shrinks to a more normal size. Blood can flow freely through the pathway in the ventricle that leads to the aortic valve, and symptoms improve.
Lifestyle changes
The doctor may recommend lifestyle changes to manage a condition that is causing the cardiomyopathy. These changes may help reduce symptoms.
Lifestyle changes may include:
Prevention
People can make lifestyle choices to reduce the risk of conditions that may lead to cardiomyopathy, such as coronary artery disease, high blood pressure, and heart attack. Examples of lifestyle choices include:
People also can control high blood pressure, high blood cholesterol, and diabetes by:
Some types of cardiomyopathy, such as inherited forms, can't be prevented. Restrictive cardiomyopathy can't always be prevented because it occurs as the result of another disease. Sometimes, underlying diseases can be prevented or treated early enough to stop restrictive cardiomyopathy from developing.
It may be possible to prevent sudden cardiac death if doctors can identify a person at high risk of this event and treat him or her with an implantable cardioverter defibrillator.
Living with cardiomyopathy
Some people, especially those with hypertrophic cardiomyopathy, may live a healthy life with few problems or symptoms. Others may have serious symptoms and complications. Very rarely, cardiomyopathy can cause sudden death in young people.
Here are some things you can do if you have cardiomyopathy:
You may need to take antibiotics before seeing the dentist or having certain medical procedures. This is important because it can prevent an infection in your heart (endocarditis).
Ongoing health care needs
You should talk to your doctor if you notice new or worse symptoms, such as swelling in your legs or feet. These could be a sign that your condition is getting worse.
You also should talk with your doctor to find out how much exercise is right for you. People with hypertrophic cardiomyopathy should not exercise vigorously, but moderate exercise, such as walking, is often a good idea.
Your doctor can help you decide what kind of diet is right for you. Doctors will often recommend that people with hypertrophic cardiomyopathy drink lots of water and other fluids. Your doctor also may suggest a diet low in salt and fat.
Cardiomyopathy often runs in families. Your doctor may suggest that your parents, brothers and sisters, and children get checked every once in a while to see whether they have cardiomyopathy.
Support groups
The Children's Cardiomyopathy Foundation provides support and information to parents of children with cardiomyopathy.
Long-term care, hospice, end-of-life issues
Cardiomyopathy can have serious complications, such as heart failure, serious arrhythmias, or sudden cardiac death. It is important that you discuss these possibilities with your family and your doctor and prepare for them.
Advance directives are documents that tell doctors and hospitals what treatment you want or do not want if you are too ill to speak for yourself. If you have a serious condition for which there is no cure, you may decide that you only want treatment to make you comfortable. You may or may not want treatment if your heart or breathing stops. Advance directives are a way for you to record your wishes about such treatment ahead of time.
As long as you are able to make your own decisions, your advance directive will not be used, and you can accept or refuse any medical treatment. But if you become seriously ill, you may not be able to make decisions about your own treatment.
Two types of advance directives include a living will and a medical power of attorney. A living will provides directions and instructions about your health care preferences. A medical power of attorney names a person you trust to speak for you when you are unable to make decisions.
Advance directives are easy to prepare. You can do it yourself without a lawyer, as long as you are 18 years or older. You may prepare your advance directive by:
Depending on the State where you live, the document also may need to be witnessed by one or two people or notarized.
Give a copy of your living will and/or medical power of attorney to a family member and keep another copy in a safe place. People with severe heart failure are in the hospital often. It is important that you or a family member bring copies of advance directive documents every time you go to the hospital.
Hospice care
If you have heart failure that gets worse over time, your treatments may eventually stop working. If you and your doctor agree that your treatments are not working, hospice care may be an option. Hospice is an organization that can comfort and support you and your family. A team of people provides hospice care. This team includes doctors, nurses, social workers, nurses' aides, chaplains, and volunteers.
The goals of hospice care are to provide:
Hospice supports life and views dying as a natural process. Hospice will work with you and your family to provide the services you need.
Research
If you are diagnosed with cardiomyopathy, you should ask your doctor about any research studies available that you may be eligible to enroll in. Research studies often provide focused attention on questions about diagnosis and treatment. The researchers conducting studies are generally experts in the field, and they may assist you and your doctor, while also gaining information that could be helpful to other patients with cardiomyopathy.


