endocarditis
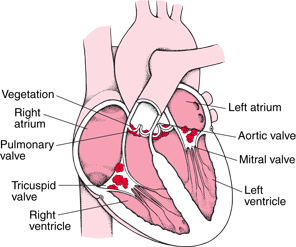
Cross section of the heart showing "vegetations" (accumulations of bacteria and blood clots) on the four valves. Image © Merck.
Endocarditis is Inflammation of the endocardium (internal lining of the heart), particularly of the heart valves, usually due to infection.
Endocarditis occurs most often in people whose endocardium has already been damaged (for example, as a result of congenital heart defects or rheumatic fever), in people whose immune system has been suppressed by anticancer drugs or immunosuppressant drugs, and in drug abusers who inject drugs intravenously. Endocarditis is also a rare feature of some types of cancer and of some autoimmune diseases (for example, systematic lupus erthematosus.
Causes and incidence
Endocarditis mat be caused by bacteria, fungi, or other microorganisms. The microorganisms may be introduced into the bloodstream during cardiac surgery, particularly if artificial materials, such as a a replacement valve, are inserted. The causative microbes may also be introduced during dental treatment (especially tooth extraction) and during surgical and investigative procedures performed on the gastrointestinal and genitourinary systems (e.g., examination of the bladder by cytoscopy). The microbes that cause endocarditis may also be introduced directly into the bloodstream on dirty needles.
People with an endocardium that is already damaged are especially vulnerable to endocarditis because clots that form on the injured surface trap the causative microorganisms, which then multiply rapidly at the site of the damage. Intravenous drug abusers are vulnerable to endocarditis, even if their hearts are healthy, because microbes from a dirty syringe or from unclean skin at the site of injection are introduced and carried to the heart in the bloodstream. People with a suppressed immune system are vulnerable because they have a lowered resistance to infection, and organisms that would normally be harmless can lead to serious infection.
Symptoms
Endocarditis may be subacute or acute. In the subacute form, the disease progresses undetected, sometimes for many months, during which time it causes serious damage to a heart valve. Symptoms are general and nonspecific, the sufferer may complain of fatigue and weakness, feverishness, night sweats, and vague aches and pains. On examination, the only evident abnormality may be a heart murmur that changes from time to time.
Acute endocarditis, which occurs less frequently, comes on suddenly. The patient suffers from severe chills, high fever, shortness of breath, and rapid or irregular heartbeat. The infection progresses quickly and may destroy the heart valves, leading to rapidly progressive heart failure (reducing pumping efficiency).
Diagnosis and treatment
Any patient suspected of having endocarditis is given a thorough physical examination. Blood samples are taken and to a laboratory for analysis. Cultures of the blood are examined for bacteria or fungi, and the sensitivity of the organisms to different types of antibiotics is determined. Tests on the heart may include electrocardiogram (ECG), electrocardiography, and angiography.
Patients are treated with high doses of antibiotics, which are usually given intravenously. Drug treatment, which may last for as long as six weeks, is started in hospital and may be continued at home. Heart valve surgery may be needed to replace a valve that has been damaged by infection or to replace an artificial valve. In some cases, heart valve replacement may need to be done as an emergency procedure.
Prevention and outlook
People at risk of endocarditis because of a heart defect are prescribed antibiotics before undergoing any procedure that runs a significant risk of introducing bacteria into the the bloodstream. People at risk should also be aware of the warning signs of endocarditis and call a doctor should they appear.
Before the introduction of antibiotic drugs, endocarditis was usually fatal. Today, treatment is successful in 65 to 80% of cases.


