angioplasty
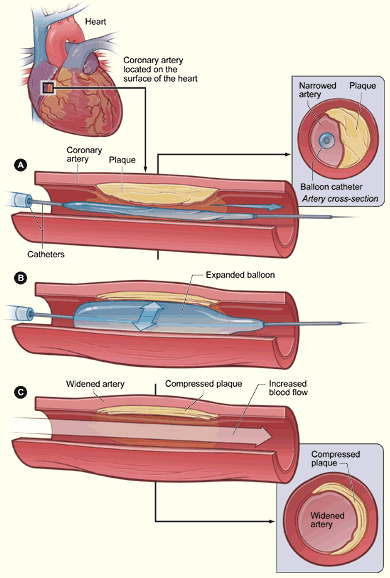
Cross-section of a coronary artery with plaque buildup. The coronary artery is located on the surface of the heart. Figure A shows the deflated balloon catheter inserted into the narrowed coronary artery. In figure B, the balloon is inflated, compressing the plaque and restoring the size of the artery. Figure C shows normal blood flow restored in the widened artery.

Placement of a stent in a coronary artery with plaque buildup. The coronary artery is located on the surface of the heart. Figure A shows the deflated balloon catheter and closed stent inserted into the narrowed coronary artery. In figure B, the balloon is inflated, expanding the stent and compressing the plaque to restore the size of the artery. Figure C shows normal blood flow restored in the stent-widened artery.
Angioplasty is a keyhole surgery procedure for repairing damaged or diseased blood vessels. It involves the use of a catheter and a balloon to open up blocked arteries, usually those in the heart. The catheter is passed into a main artery, often in the groin, and pushed along until it reaches the narrowed vessel. The balloon at the tip of the catheter is then inflated so that it pushes opens up the artery – most commonly pushing any build-up of plaque (fatty deposits) in the artery against the vessel's wall – allowing a freer flow of blood. Angioplasty is less radical alternative to open heart or bypass surgery.
Coronary angioplasty
Coronary angioplasty is used to restore blood flow through a narrowed or blocked artery in the heart. It is also known by a variety of other names: balloon angioplasty, coronary artery angioplasty, percutaneous coronary intervention, and percutaneous transluminal angioplasty.
The arteries of the heart – the coronary arteries – can become narrowed and blocked due to buildup of a material called plaque on their inner walls. This narrowing reduces the flow of blood through the artery and can lead, over time, to coronary artery disease and heart attack. In angioplasty, a thin tube called a catheter with a balloon or other device on the end is first threaded through a blood vessel in the arm or groin (upper thigh) up to the site of a narrowing or blockage in a coronary artery. Once in place, the balloon is then inflated to push the plaque outward against the wall of the artery, widening the artery and restoring the flow of blood through it.
Angioplasty is used to:
Angioplasty was first used in 1977. A tiny balloon was used to open or widen narrowed arteries. Since then, new devices and medicines have improved the procedure and made it appropriate for more people. The improvements include:
When a stent is not used, in 4 out of 10 people the artery will close again within the first 6 months.
Today, angioplasty is performed on more than 1 million people a year in the United States. The procedure is best done:
Research on angioplasty continues to:
When is coronary angioplasty done?
Your doctor may consider angioplasty if lifestyle changes and medicines do not improve your symptoms of coronary artery disease. Angioplasty is an alternative to coronary bypass surgery, which is a major operation.
Your doctor will consider several factors when recommending angioplasty or bypass surgery:
Angioplasty is often selected if:
The advantages of angioplasty are that it:
The disadvantage of angioplasty is that the artery may close again. If this happens, you will need a second angioplasty or bypass surgery. Bypass surgery tends to do a more complete job of restoring the heart's blood supply.
Your doctor will discuss treatment options with you and recommend the best procedure for you.
Coronary angioplasty is also used as an emergency procedure during a heart attack. Quickly opening a blocked coronary artery minimizes the damage during a heart attack and restores blood flow to the heart muscle. There are also drugs that can be used to dissolve clots in a coronary artery. These drugs are most effective when given within 3 hours after the heart attack begins. Angioplasty performed early, without drugs that dissolve clots, also minimizes damage to the heart muscle.
Risks
Angioplasty is a common medical procedure. Major complications are rare, but any medical procedure has risks. The risks of angioplasty include:
Other less-common complications include:
The risk of complications is higher in:
Before coronary angioplasty?
meeting with your doctor
A heart specialist (cardiologist) performs the angioplasty. If your angioplasty is not done as an emergency, you will meet with your cardiologist before the procedure to have a physical exam and discuss the procedure. Your doctor will order:
Your angioplasty will be scheduled at a hospital. You will also be told:
What to expect
During coronary angioplasty?
Angioplasty is performed in a special part of the hospital called the cardiac catheterization lab. This lab has special video screens and X-ray machines. Your doctor uses this equipment to see enlarged pictures of the blocked areas in your coronary arteries.
Preparation (prep)
At the cardiac catheterization lab, you will lie on a table. The doctor will use an intravenous (IV) line to give you fluids and medicines. The medicines relax you and prevent blood clots. The rest of your prep includes:
Steps in angioplasty
When you are comfortable, the doctor will begin the procedure.
When the doctor finishes, the wire and catheter are removed. A special outer catheter may remain in place. If a closure device is used, all tubes will be removed.
During the procedure, strong antiplatelet medicines are given through the IV to prevent clots from forming in the artery or on the stent. These medicines help thin your blood. They usually are started just before the angioplasty and may continue for 12–24 hours afterward.
Recovery
After the angioplasty procedure, you will be moved to a special care unit.
You must lie still for several hours to allow the blood vessels in your groin (or arm) to seal completely.
While you recover, nurses will check:
The place where the tube was inserted may feel sore or tender for about 1 week.
In most cases, you may go home 1–2 days after the procedure.
After coronary angioplasty?
Angioplasty is not a cure for coronary artery disease (CAD). You should discuss with your doctor what led to CAD and the need for angioplasty.
Going home
When you are ready to leave the hospital, you will receive instructions to follow at home, including:
Swelling
Drainage
If you have pain or bleeding where the tube was inserted
Your doctor will prescribe medicine to prevent blood clots from forming. It is very important that you take the medicine as directed. The medicine can prevent the stent from becoming blocked. Types of medicine may include:
Most people can return to work and other normal activities about 1 week after angioplasty.
Cardiac rehabilitation
Your doctor may recommend that you participate in a cardiac rehabilitation (rehab) program. Cardiac rehab provides medical guidance and support to help you return to work or daily activities.


