glaucoma
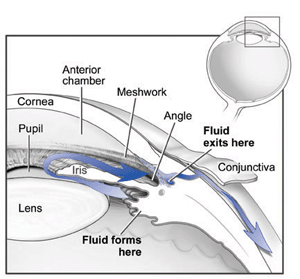
Glaucoma before surgery.
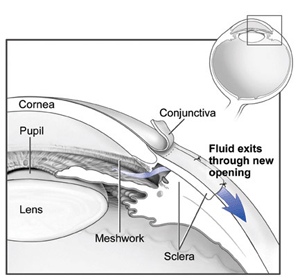
Glaucoma after surgery.
Glaucoma is a group of diseases that can damage the eye's optic nerve and result in vision loss and blindness. Glaucoma occurs when the normal fluid pressure inside the eyes slowly rises. However, with early treatment, you can often protect your eyes against serious vision loss.
Forms of glaucoma
Open-angle glaucoma is the most common form. Some people have other types of the disease.
Low-tension or normal-tension glaucoma
Optic nerve damage and narrowed side vision occur in people with normal eye pressure. Lowering eye pressure at least 30% through medicines slows the disease in some people. Glaucoma may worsen in others despite low pressures.
A comprehensive medical history is important in identifying other potential risk factors, such as low blood pressure, that contribute to low-tension glaucoma. If no risk factors are identified, the treatment options for low-tension glaucoma are the same as for open-angle glaucoma.
Angle-closure glaucoma
The fluid at the front of the eye cannot reach the angle and leave the eye. The angle gets blocked by part of the iris. People with this type of glaucoma have a sudden increase in eye pressure. Symptoms include severe pain and nausea, as well as redness of the eye and blurred vision. If you have these symptoms, you need to seek treatment immediately.
This is a medical emergency. If your doctor is unavailable, go to the nearest hospital or clinic. Without treatment to improve the flow of fluid, the eye can become blind in as few as one or two days. Usually, prompt laser surgery and medicines can clear the blockage and protect sight.
Congenital glaucoma
Children are born with a defect in the angle of the eye that slows the normal drainage of fluid. These children usually have obvious symptoms, such as cloudy eyes, sensitivity to light, and excessive tearing. Conventional surgery typically is the suggested treatment, because medicines may have unknown effects in infants and be difficult to administer. Surgery is safe and effective. If surgery is done promptly, these children usually have an excellent chance of having good vision.
Secondary glaucomas
These can develop as complications of other medical conditions. These types of glaucomas are sometimes associated with eye surgery or advanced cataracts, eye injuries, certain eye tumors, or uveitis (eye inflammation). Pigmentary glaucoma occurs when pigment from the iris flakes off and blocks the meshwork, slowing fluid drainage. A severe form, called neovascular glaucoma, is linked to diabetes. Corticosteroid drugs used to treat eye inflammations and other diseases can trigger glaucoma in some people. Treatment includes medicines, laser surgery, or conventional surgery.
Causes and risk factors
How does open-angle glaucoma damage the optic nerve?
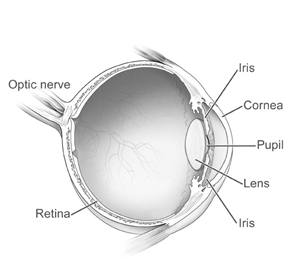
In the front of the eye is a space called the anterior chamber. A clear fluid flows continuously in and out of the chamber and nourishes nearby tissues. The fluid leaves the chamber at the open angle where the cornea and iris meet. (See diagram below.) When the fluid reaches the angle, it flows through a spongy meshwork, like a drain, and leaves the eye.
Sometimes, when the fluid reaches the angle, it passes too slowly through the meshwork drain. As the fluid builds up, the pressure inside the eye rises to a level that may damage the optic nerve. When the optic nerve is damaged from increased pressure, open-angle glaucoma – and vision loss – may result. That's why controlling pressure inside the eye is important.
Does increased eye pressure mean that I have glaucoma?
Not necessarily. Increased eye pressure means you are at risk for glaucoma, but does not mean you have the disease. A person has glaucoma only if the optic nerve is damaged. If you have increased eye pressure but no damage to the optic nerve, you do not have glaucoma. However, you are at risk. Follow the advice of your eye care professional.
Can I develop glaucoma if I have increased eye pressure?
Not necessarily. Not every person with increased eye pressure will develop glaucoma. Some people can tolerate higher eye pressure better than others. Also, a certain level of eye pressure may be high for one person but normal for another.
Whether you develop glaucoma depends on the level of pressure your optic nerve can tolerate without being damaged. This level is different for each person. That's why a comprehensive dilated eye exam is very important. It can help your eye care professional determine what level of eye pressure is normal for you.
Can I develop glaucoma without an increase in my eye pressure?
Yes. Glaucoma can develop without increased eye pressure. This form of glaucoma is called low-tension or normal-tension glaucoma. It is not as common as open-angle glaucoma.
Who is at risk for glaucoma?
Anyone can develop glaucoma. Some people are at higher risk than others. They include:
Among African Americans, studies show that glaucoma is:
A comprehensive dilated eye exam can reveal more risk factors, such as high eye pressure, thinness of the cornea, and abnormal optic nerve anatomy. In some people with certain combinations of these high-risk factors, medicines in the form of eye drops reduce the risk of developing glaucoma by about half.
What can I do to protect my vision?
Studies have shown that the early detection and treatment of glaucoma, before it causes major vision loss, is the best way to control the disease. So, if you fall into one of the high-risk groups for the disease, make sure to have your eyes examined through dilated pupils every one to two years by an eye care professional.
If you are being treated for glaucoma, be sure to take your glaucoma medicine every day. See your eye care professional regularly.
You also can help protect the vision of family members and friends who may be at high risk for glaucoma. Encourage them to have a comprehensive dilated eye exam at least once every two years. Remember: Lowering eye pressure in glaucoma's early stages slows progression of the disease and helps save vision.
Symptoms and detection
What are the symptoms of glaucoma?
At first, there are no symptoms. Vision stays normal, and there is no pain.
However, as the disease progresses, a person with glaucoma may notice his or her side vision gradually failing. That is, objects in front may still be seen clearly, but objects to the side may be missed.
As glaucoma remains untreated, people may miss objects to the side and out of the corner of their eye. Without treatment, people with glaucoma will slowly lose their peripheral (side) vision. They seem to be looking through a tunnel. Over time, straight-ahead vision may decrease until no vision remains.
Glaucoma can develop in one or both eyes.
How is glaucoma detected?
Glaucoma is detected through a comprehensive eye exam that includes:
Treatment
Can glaucoma be treated?
Yes. Immediate treatment for early stage, open-angle glaucoma can delay progression of the disease. That's why early diagnosis is very important.
Glaucoma treatments include medicines, laser trabeculoplasty, conventional surgery, or a combination of any of these. While these treatments may save remaining vision, they do not improve sight already lost from glaucoma.
How should I use my glaucoma eye drops?
If eye drops have been prescribed for treating your glaucoma, you need to use them properly and as instructed by your eye care professional. Proper use of your glaucoma medication can improve the medicine's effectiveness and reduce your risk of side effects. To properly apply your eye drops, follow these steps:
What can I do if I already have lost some vision from glaucoma?
If you have lost some sight from glaucoma, ask your eye care professional about low vision services and devices that may help you make the most of your remaining vision. Ask for a referral to a specialist in low vision.
Many community organizations and agencies offer information about low vision counseling, training, and other special services for people with visual impairments. A nearby school of medicine or optometry may provide low vision services.


