pulmonary embolism
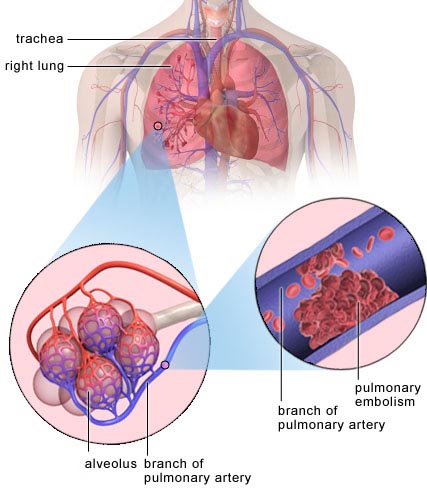
Example of where a pulmonary embolism may occur. Image: BUPA.
A pulmonary embolism is an obstruction or sudden blockage in the pulmonary artery or one of its branches, usually due to a blood clot that traveled to the lung from the leg. A clot that forms in one part of the body and travels in the bloodstream to another part of the body is called an embolus.
Pulmonary embolism (PE) is a serious condition that can cause:
If a clot is large, or if there are many clots, pulmonary embolism can cause death.
In most cases, pulmonary embolism is a complication of a condition called deep vein thrombosis (DVT). In DVT, blood clots form in the deep veins of the body – most often in the legs. These clots can break free, travel to the lung, and block an artery.
More than 600,000 people in the United States have a pulmonary embolism each year, and more than 60,000 of them die. Most of those who die do so within 30 to 60 minutes after symptoms start. Pulmonary embolism is one of the most common causes of death in hospitalized people who must remain in bed for a long time.
Causes
Nine out of 10 cases of pulmonary embolism are caused by blood clots that form in the legs (deep vein thrombosis) and then travel to the lungs.
Leg clots can form when blood flow is restricted and slows down. This happens when you do not move around for long periods of time, such as:
Rarely, an air bubble, part of a tumor, or other tissue travels to the lung and causes pulmonary embolism.
Diagnosis
Your doctor will take a health history and perform a physical exam in order to:
Physical exam
The physical exam will include:
Tests
To help determine whether you have a pulmonary embolism or related disease or condition, initial testing includes:
To measure the amount of oxygen and carbon dioxide in the blood (arterial blood gas). A pulmonary embolism may change the levels of oxygen and carbon dioxide in the blood.
Your doctor will order additional tests based on how likely it is that you have a pulmonary embolism and which tests are available. Tests could include:
Treatment
The primary goals in treating pulmonary embolism are to:
Treatment may include:
Treatment will vary depending on how severe your symptoms are. If your symptoms are severe, you need immediate emergency treatment. If your symptoms are mild, you can be treated as an outpatient.
Medicines
Anticoagulants (blood thinners) decrease your blood's ability to clot. They are used to stop clots from getting bigger and to prevent blood clots from forming. Anticoagulants do not break up blood clots that have already formed. Your body's natural system will dissolve the clot. Anticoagulants can be given:
Heparin and warfarin may be given at the same time. Heparin acts quickly, whereas warfarin takes 2 to 3 days before it starts to work. Once warfarin is working, the heparin will be stopped. Pregnant women cannot take warfarin and are treated with heparin only.
If you have deep vein thrombosis, treatment with anticoagulants usually lasts for 3 to 6 months. However, the length of treatment may vary if:
The most common side effect of anticoagulants is bleeding. You need to have regular blood tests to check how well the medicine is working. You should call your doctor right away if you have easy bruising or bleeding.
Thrombin inhibitors are new medicines that interfere with the clotting process. They are used to treat some types of clots for patients who cannot take heparin.
Emergency treatment
When pulmonary embolism is life threatening, doctors may use treatments to remove or break up clots in the lungs. These treatments are given in the emergency room or in the hospital and include:
Additional considerations
Vena cava filters are used when you cannot take medicines to thin your blood, or if you are taking blood thinners and continue to develop clots. The filter is inserted inside a large vein called the inferior vena cava (the vein that carries blood from the body back to the heart). It can catch the clots as they try to move through the body to the lungs. This treatment can prevent a clot from traveling to the lungs. It cannot stop other clots from forming.
Graduated compression stockings are worn on the legs from the arch of the foot to just above or below the knee. These stockings are tight at the feet and become looser as they go up the leg. This causes a gentle compression (or pressure) up your leg. The stockings provide support and reduce the chronic swelling that can occur in the leg after a blood clot has occurred.
Prevention
Preventing pulmonary embolism begins with preventing deep vein thrombosis (DVT). It is important to know whether you are at risk for DVT and to take steps to lower your risk.
If you have never had a deep vein clot, but are in a situation that may increase your risk, be sure to:
If you already have had DVT or a pulmonary embolism, you need to prevent further clots from developing by:
Life after pulmonary embolism
Once you have had a pulmonary embolism (with or without deep vein thrombosis (DVT)), you have a greater chance of having another one. After treatment has begun and you are feeling better, your treatment will continue at home.
At home, you will continue taking blood-thinning medicines. It is important that you:
Medicines used to treat pulmonary embolism can thin your blood too much. This can cause:
Pass bright red blood in your stool or have black tarry stools
Develop pain in your abdomen
Have any sudden changes in your vision
Have sudden loss of movement of your legs or arms
Have sudden memory loss or confusion
Treatment for pulmonary embolism usually lasts up to 6 months. During treatment and after, you should continue to:


