mitral valve prolapse
Mitral valve prolapse (MVP) is a condition in which one of the valves of the heart, the mitral valve, doesn't work properly. The flaps of the valve are floppy and don't close tightly. Much of the time, MVP doesn't cause any problems. Rarely, blood can leak the wrong way through the floppy valve, which may cause shortness of breath, palpitations, chest pain, and other symptoms.
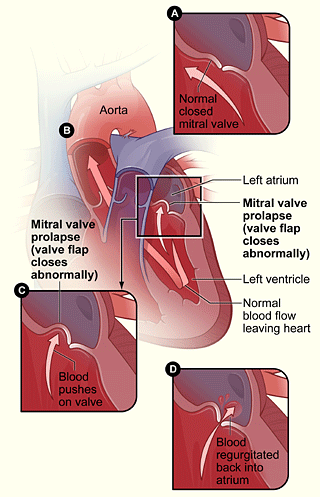
The mitral valve controls the flow of blood between the two chambers on the left side of the heart. The two chambers are the left atrium and the left ventricle. The mitral valve allows blood to flow from the left atrium to the left ventricle, but not back the other way. (The heart also has a right atrium and ventricle, separated by the tricuspid valve.)
At the beginning of a heartbeat, the atria contract and push blood through to the ventricles. The flaps of the mitral and tricuspid valves swing open to let the blood through. Then, the ventricles contract to pump the blood out of the heart. When the ventricles contract, the flaps of the mitral and tricuspid valves swing shut and form a tight seal that prevents blood from flowing back into the atria.
In mitral valve prolapse, when the left ventricle contracts, one or both flaps of the mitral valve flop or bulge back (prolapse) into the left atrium. This can prevent the valve from forming a tight seal, and allow blood to flow backward from the ventricle into the atrium. The backward flow of blood is called regurgitation, and it can lead to symptoms and complications (see mitral regurgitation).
Regurgitation doesn't occur in all cases of MVP. In fact, the majority of people with MVP don't have regurgitation and never have any symptoms or complications. In these people, even though the valve flaps prolapse, the valve is still able to form a tight seal.
When regurgitation does occur, it can cause complications and troublesome symptoms such as shortness of breath, a racing or irregular heartbeat, or chest pain. Regurgitation can get worse over time and lead to changes in the heart's size and higher pressures in the left atrium and lungs. Regurgitation increases the risk for heart valve infections.
Medicines can treat MVP symptoms that cause people to worry or have discomfort. Medicines are also used to prevent complications. Sometimes a person will need surgery to repair or replace the mitral valve.
Causes
The exact cause of mitral valve prolapse isn't known. Most people with the condition are born with it. It tends to run in families and is more common in people who were born with connective tissue disorders, such as Marfan syndrome.
The mitral valve can be abnormal in two ways. First, the valve flaps may be oversized and thickened. Second, the valve flaps may be floppy. The tissue of the flaps and their supporting "strings" are too stretchy, and parts of the valve flop or bulge back into the atrium. Some people's valves are abnormal in both ways. Either way can keep the valve from making a tight seal.
Who is at risk?
MVP occurs in all age groups and in men and women. MVP with complications or severe symptoms is seen most often in men older than 50.
Certain conditions increase the risk for MVP, including:
Signs and symptoms
The majority of people with mitral valve prolapse aren't affected by the condition because they don't have any symptoms or significant mitral valve regurgitation. Among those who do have symptoms, heart palpitations (strong or rapid heartbeats) are reported most often. Other symptoms include shortness of breath, cough, dizziness, fatigue (tiredness), anxiety, migraine, and chest discomfort. Symptoms can vary widely from one person to another. They tend to be mild but can worsen over time, mainly when there are complications of MVP.
Complications of mitral valve prolapse
Complications of MVP are rare, but when present, are most often due to regurgitation of blood through the valve. Mitral valve regurgitation is most common among men and people with high blood pressure. People with severe cases of mitral valve regurgitation may need valve surgery to prevent complications.
In mitral valve regurgitation, blood flows backward from the left ventricle into the left atrium. It can even back up from the atrium into the lungs, causing shortness of breath. The backward flow of blood puts a strain on the muscles of both the atrium and the ventricle. Over time, the strain can lead to arrhythmias (abnormal heart rhythms). Regurgitation also increases the risk of infective endocarditis, an infection of the lining of the valves.
Arrhythmias
Mitral valve regurgitation can cause arrhythmia, an abnormal speed or rhythm of the heartbeat.
There are many different types of arrhythmia. The most common arrhythmias are harmless. Others can be serious or even life threatening. When the heart rate is too slow, too fast, or irregular, the heart may not be able to pump enough blood to the body. Lack of blood flow can damage the brain, heart, and other organs.
One troublesome arrhythmia that may be seen with MVP and regurgitation is atrial fibrillation. In atrial fibrillation, the walls of the atria quiver instead of beating normally. As a result, the atria aren't able to pump blood into the ventricles the way they should.
Atrial fibrillation is bothersome but rarely life threatening unless it's very fast or unless it causes blood clots to form in the atria. Blood clots can form in the atria because some of the blood pools there instead of flowing into the ventricles. If a blood clot breaks off and goes into the bloodstream, it can reach the brain and cause a stroke.
Infection of the mitral valve
A deformed mitral valve flap attracts bacteria that may be found in the bloodstream. The bacteria attach to the valve and can cause a serious infection called infective endocarditis. Signs and symptoms of a bacterial infection include fever, chills, body aches, or headaches.
Infective endocarditis doesn't happen often, but when it does, it's serious. MVP is the most common heart condition that puts people at risk for this infection.
People with MVP and other valve problems can take antibiotics to reduce the risk of infective endocarditis. Antibiotics are often prescribed for people with MVP before dental work or certain types of surgery.
Diagnosis
Mitral valve prolapse (MVP) is most often found during a routine physical exam when your doctor uses a stethoscope to listen to your heart. Your doctor listens for a certain click and/or murmur. Stretched valve flaps, as seen in MVP, can make a clicking sound as they shut. If the valve is leaking blood back into the atrium, a murmur or whooshing sound can often be heard. However, these abnormal heart sounds may come and go, so they may not be heard at the time of an exam, even if you have MVP. As a result, diagnostic tests and procedures may also be needed to diagnose MVP.
Diagnostic tests and procedures
Echocardiogram
An echocardiogram is the most useful test for diagnosing MVP. This test uses sound waves to create a moving picture of your heart. An echocardiogram provides information about the size and shape of your heart and how well your heart chambers and valves are functioning. The test also can identify areas of poor blood flow to the heart, areas of heart muscle that are not contracting normally, and previous injury to the heart muscle caused by poor blood flow. The echocardiogram is a painless test that's used to look for prolapse of the mitral valve flaps and for backflow (regurgitation) of blood through the leaky valve.
There are several different types of echocardiograms, including a stress echocardiogram. During this test, an echocardiogram is done both before and after your heart is stressed either by having you exercise or by injecting a medicine into your bloodstream that makes your heart beat faster and work harder. A stress echocardiogram is usually done to find out if you have decreased blood flow to your heart (see coronary artery disease).
Echocardiography also can be performed through your esophagus (the tube leading from your mouth to your stomach) to get a closer look at the mitral valve. A tiny probe in your esophagus takes sound wave pictures of your heart. This form of echocardiogram is called a transesophageal echocardiogram, or TEE.
Doppler ultrasound
A Doppler ultrasound is part of the echocardiogram test. The Doppler ultrasound is used to show the speed and direction of blood flow through the mitral valve.
Other tests
Other tests that can help diagnose MVP are:
Treatment
Goals of treatment
The goals of treating mitral valve prolapse (MVP) are to:
Who needs treatment?
Most people with MVP don't need treatment because they don't have significant regurgitation of blood through the valve, and they have few or no symptoms. Even people who do have symptoms may not require treatment. The presence of symptoms doesn't necessarily mean that there is significant regurgitation through the valve. People with MVP and troublesome mitral valve regurgitation usually need treatment.
Specific types of treatment
MVP can be treated with medicine, surgery, or both.
Medicine
For people with MVP who have little or no regurgitation, medicines called beta blockers have been used to treat symptoms such as palpitations (strong or rapid heartbeats) and chest discomfort.
For people with MVP who have significant regurgitation and symptoms, the following medicines may be used to prevent complications:
Surgery
Surgery on the mitral valve is done only when the valve is very abnormal and blood is regurgitating into the atrium. The main goal of surgery is to improve symptoms and reduce the risk for heart failure.
The timing of the surgery is very important. If it's done too early and your leaking valve is working fairly well, you may be put at needless risk from surgery. If it's done too late, irreversible heart damage may have already occurred.
Surgical approaches. The traditional surgical approach for mitral valve repair and replacement is through an incision in the breastbone to expose the heart. A small but growing number of heart surgeons are using another approach that uses one or more smaller incisions through the side of the chest wall. This approach can result in less cutting, reduced blood loss, and a shorter hospital stay, but it isn't available yet in all hospitals.
Valve repair versus valve replacement. In mitral valve surgery, the valve may either be repaired or replaced completely. Valve repair is preferred when possible. It's less likely to weaken the heart, lowers the risk of infection, and decreases the need for lifelong use of blood-thinning medicines. If repair isn't an option, then the valve can be replaced. Two types of substitute valves are available: a mechanical valve or a biological valve. Mechanical valves are made of man-made materials and can last a lifetime. Patients with mechanical valves must take blood-thinning medicines for life. Biological valves are valves taken from cows or pigs or made from human tissue. Many patients with biological valves don't need to take blood-thinning medicines for life. The major drawback of biological valves is that they weaken and often only last about 10 years.
After surgery, a patient usually stays in the intensive care unit in the hospital for 2 to 3 days. Most people spend about 1 to 2 weeks in the hospital. Complete recovery takes a few weeks to several months, depending on the person's health before surgery.
Experimental approaches. Some researchers are testing the repair of leaky valves using a catheter inserted through a large blood vessel. While this approach is less invasive and can save the patient from having open heart surgery, it's only being done in a few medical centers. In addition, because it's a new procedure, it hasn't yet been shown in large studies to be better than traditional approaches.
Prevention
Mitral valve prolapse (MVP) can't be prevented, but some of its complications can.
People with mitral valve regurgitation and/or thickened valve flaps are at increased risk for infective endocarditis, an infection of the surface of the mitral valve flaps. To prevent infective endocarditis, antibiotics are given before dental and medical procedures that can let bacteria into the bloodstream. Antibiotics are usually given 1 hour before a procedure, and a second dose may be given later. Antibiotics are usually given for the following types of procedures:
Antibiotics may be given at childbirth as well, although MVP by itself has no effect on pregnancy.
You doctor will prescribe antibiotics that are appropriate for the type of procedure you're having. Therefore, taking only those antibiotics prescribed, and exactly as prescribed, is important. Not taking antibiotics as prescribed can increase the risk of resistant bacteria causing a valve infection in the future. This type of infection is difficult to treat.
Living with mitral valve prolapse
Most people with mitral valve prolapse (MVP) have no symptoms or problems, need no treatment, and are able to lead normal, active lives. Symptoms and complications, when present, most often can be controlled with medicines. Some people may need heart valve surgery to relieve their symptoms and prevent complications. In a few cases, complications of MVP can result in heart failure, arrhythmias, or stroke.
Ongoing health care needs
If you have MVP, you should:
- Tell your doctors and dentists that you have MVP. Take good care of your teeth and gums. See your dentist for regular visits.
- Call your doctor if you have any signs of infection, such as sore throat, general body aches, and fever.
- Take antibiotics specifically as prescribed before dental work and certain types of surgery.
- Avoid smoking and taking birth control pills, which increase the risk for blood clots.
- Talk with your health care provider about how much and what kind of exercise is right for you.
- Ask about any changes you need to make to your diet.


