coronary artery disease
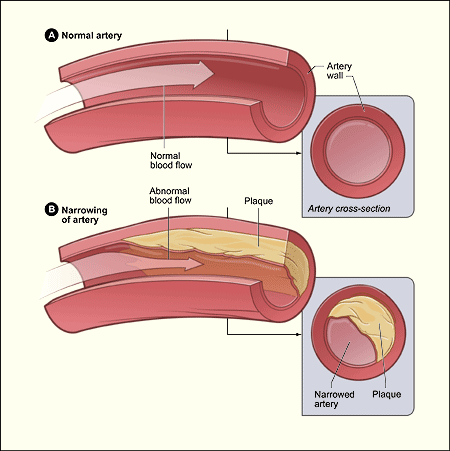
An artery with normal blood flow (figure A) and an artery containing plaque buildup (figure B). Credit: National Institutes of Health.
Coronary artery disease (CAD), also called coronary heart disease, occurs when the arteries that supply blood to the heart muscle (the coronary arteries) become hardened and narrowed. The arteries harden and narrow due to buildup of a material called plaque on their inner walls. The buildup of plaque is known as atherosclerosis. As the plaque increases in size, the insides of the coronary arteries get narrower and less blood can flow through them. Eventually, blood flow to the heart muscle is reduced, and, because blood carries much-needed oxygen, the heart muscle is not able to receive the amount of oxygen it needs. Reduced or cutoff blood flow and oxygen supply to the heart muscle can result in:
Over time, CAD can weaken the heart muscle and contribute to:
CAD is the most common type of heart disease. It is the leading cause of death in the United States in both men and women.
Causes
Coronary artery disease (CAD) is caused by atherosclerosis (the thickening and hardening of the inside walls of arteries). Some hardening of the arteries occurs normally as a person grows older.
In atherosclerosis, plaque deposits build up in the arteries. Plaque is made up of fat, cholesterol, calcium, and other substances from the blood. Plaque buildup in the arteries often begins in childhood. Over time, plaque buildup in the coronary arteries can:
Plaque in the arteries can be:
Who is at risk for?
About 13 million people in the United States have coronary artery disease (CAD). It is the leading cause of death in both men and women. Each year, more than half a million Americans die from CAD. Several factors increase the risk of developing CAD. The more risk factors you have, the greater chance you have of developing CAD. Some CAD risk factors, such as age, can't be modified, but others can.
Risk factors that cannot be modified
- In men, risk increases after age 45.
- In women, risk increases after age 55.
- Heart disease diagnosed before age 55 in father or brother.
- Heart disease diagnosed before age 65 in mother or sister.
Risk factors that can be modified
Other potential risk factors
Scientists continue to study other potential risk factors for developing CAD.
According to some research studies, high blood levels of a substance called C-reactive protein (CRP) may be associated with an increased risk of developing CAD and having a heart attack. CRP is a protein in the blood that shows the presence of inflammation. Inflammation is the body's response to injury or infection. CRP levels rise when there is inflammation. The inflammation process appears to contribute to the growth of plaque in arteries.
Research is underway to find out if reducing inflammation and lowering CRP levels can also reduce the risk of developing CAD and having a heart attack.
Signs and symptoms
The most common symptoms of coronary artery disease (CAD) are:
The severity of symptoms varies widely. Symptoms may become more severe as coronary arteries become narrower due to the buildup of plaque (atherosclerosis).
In some people, the first sign of CAD is a heart attack. A heart attack happens when plaque in a coronary artery breaks apart, causing a blood clot to form and block the artery.
Diagnosis
There is no single test to diagnose coronary artery disease (CAD). Your doctor will ask about your medical history and your family's medical history, assess your risk factors, and do a physical exam and several tests. These procedures are used to:
- Decide if you have CAD
- Determine the extent and severity of the disease
- Rule out other possible causes of your symptoms
There are several different types of echocardiograms, including a stress echocardiogram. During this test, an echocardiogram is done both before and after your heart is stressed either by having you exercise or by injecting a medicine into your bloodstream that makes your heart beat faster and work harder. A stress echocardiogram is usually done to find out if you have decreased blood flow to your heart (coronary artery disease).
During exercise stress testing, your blood pressure and EKG readings are monitored while you walk or run on a treadmill or pedal a bicycle. Other heart tests, such as nuclear heart scanning or echocardiography, also can be done at the same time. These would be ordered if your doctor needs more information than the exercise stress test can provide about how well your heart is working.
If you are unable to exercise, a medicine can be injected through an intravenous line (IV) into your bloodstream to make your heart work harder and beat faster, as if you are exercising on a treadmill or bicycle. Nuclear heart scanning or echocardiography is then usually done.
During nuclear heart scanning, radioactive tracer is injected into your bloodstream, and a special camera shows the flow of blood through your heart and arteries. Echocardiography uses sound waves to show blood flow through the chambers and valves of your heart and to show the strength of your heart muscle.
Your doctor also may order two newer tests along with stress testing if more information is needed about how well your heart works. These new tests are magnetic resonance imaging (MRI) and positron emission tomography (PET) scanning of the heart. MRI shows detailed images of the structures and beating of your heart, which may help your doctor better assess if parts of your heart are weak or damaged. PET scanning shows the level of chemical activity in different areas of your heart. This can help your doctor determine if enough blood is flowing to the areas of your heart. A PET scan can show decreased blood flow caused by disease or damaged muscles that may not be detected by other scanning methods.
There are different types of nuclear heart scans. Most scans have two phases – taking pictures of the heart at rest and while it is beating faster (called a stress test), although sometimes only a rest scan is done. Many heart problems show up more clearly when your heart is stressed than when it is at rest. By comparing the nuclear heart scan of your heart at rest to your heart at "stress," your doctor can determine if your heart is functioning normally or not.
Your doctor may also order the following blood tests:
Prevention or delay
Preventing or delaying coronary artery disease (CAD) begins with knowing which risk factors you have and taking action. Remember, your chances of developing CAD increase with the number of risk factors you have.
Know your family history of health problems related to CAD. If you or someone in your family has CAD, be sure to tell your doctor. Make sure everyone in your family gets enough exercise and maintains a healthy body weight.
By controlling your risk factors with lifestyle changes and medicines, you may prevent or delay the development of CAD.
CAD can cause serious complications, but by following your doctor's advice and changing your habits, you can prevent or reduce the chance of:
If you have any other health conditions, it is important that you follow your doctor's directions to treat those conditions. By staying as healthy as possible, you can lower your risk of developing CAD and its complications.
Treatment
Treatment for coronary artery disease (CAD) may include lifestyle changes, medicines, and special procedures. The goals of treatment are to:
Lifestyle changes
Making lifestyle changes can help treat CAD. For some people, these changes may be the only treatment needed:
Medicines
In addition to making lifestyle changes, medicines may be needed to treat CAD. Some medicines decrease the workload on the heart and relieve symptoms of CAD. Others decrease the chance of having a heart attack or dying suddenly and prevent or delay the need for a special procedure (for example, angioplasty or bypass surgery).
Several types of medicine are commonly used to treat CAD.
Special procedures
Angioplasty or bypass surgery may be used to treat CAD if:
Some people may need to have angioplasty or bypass surgery on an emergency basis during a heart attack to limit damage to the heart.
Cardiac rehabilitation
Your doctor may prescribe cardiac rehabilitation (rehab) for angina or after bypass surgery, angioplasty, or a heart attack. Cardiac rehab, when combined with medicine and surgical treatments, can help you recover faster, feel better, and develop a healthier lifestyle.
Almost everyone with CAD can benefit from cardiac rehab.
Cardiac rehab often begins in the hospital after a heart attack, heart surgery, or other heart treatment. Rehab continues in an outpatient setting after you leave the hospital.
The cardiac rehab team may include:
Rehab has two parts:


