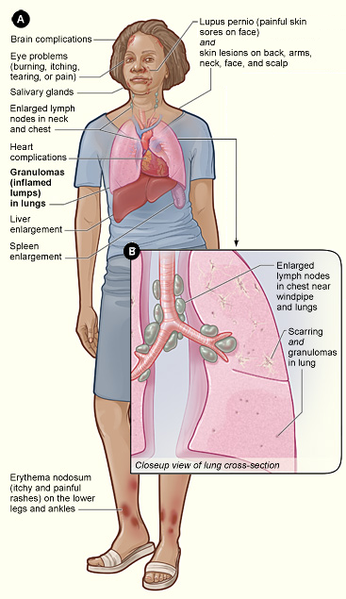
Sarcoidosis involves inflammation that produces tiny lumps of cells in various organs in the body. The lumps are called granulomas
because they look like grains of sugar or sand. They are very small and
can be seen only with a microscope.
These tiny granulomas can grow and clump together, making many large and
small groups of lumps. If many granulomas form in an organ, they can affect
how the organ works. This can cause symptoms of sarcoidosis.
Sarcoidosis can occur in almost any part of the body, although it usually
affects some organs more than others. It usually starts in one of two places:
Lungs
Lymph nodes, especially the lymph
nodes in the chest cavity.
Sarcoidosis also often affects the:
Skin
Eyes
Liver.
Less often, sarcoidosis affects the:
Spleen
Brain
Nerves
Heart
Lacrimal glands
Salivary glands
Bones and joints.
Rarely, sarcoidosis affects other organs, including the:
Thyroid gland
Breasts
Kidneys
Reproductive organs.
Sarcoidosis almost always occurs in more than one organ at a time.
Sarcoidosis has an active and a nonactive phase:
In the active phase, the granulomas form and grow. In this phase,
symptoms can develop, and scar tissue can form in the organs where the
granulomas occur.
In the nonactive phase, the inflammation goes down, and the granulomas
stay the same size or shrink. But the scars may remain and cause symptoms.
The course of the disease varies greatly among people.
In many people, sarcoidosis is mild. The inflammation that causes
the granulomas may get better on its own. The granulomas may stop growing
or shrink. Symptoms may go away within a few years.
In some people, the inflammation remains but doesn't get worse. You
may also have symptoms or flare-ups and need treatment every now and
then.
In other people, sarcoidosis slowly gets worse over the years and
can cause permanent organ damage. Although treatment can help, sarcoidosis
may leave scar tissue in the lungs, skin, eyes, or other organs. The
scar tissue can affect how the organs work. Treatment usually does not
affect scar tissue.
Changes in sarcoidosis usually occur slowly (e.g., over months). Sarcoidosis
does not usually cause sudden illness. However, some symptoms may occur
suddenly. They include:
Disturbed heart rhythms
Arthritis in the ankles
Eye symptoms.
In some serious cases in which vital organs are affected, sarcoidosis can
result in death.
Sarcoidosis is not a form of cancer.
There is no known way to prevent sarcoidosis.
Sarcoidosis was once thought to be an uncommon condition. It's now known
to affect tens of thousands of people throughout the United States alone.
Because many people who have sarcoidosis have no symptoms, it's hard to
know how many people have the condition.
Sarcoidosis was identified in the late 1860s. Since then, scientists have
developed better tests to diagnose it and made advances in treating it.
Causes
The cause of sarcoidosis is not known. And, there may be more than one thing
that causes it.
Scientists think that sarcoidosis develops when the immune
system responds to something in the environment (e.g., bacteria, viruses,
dust, chemicals) or perhaps to the body's own tissues (autoimmunity).
Normally, the immune system defends the body against things that it sees
as foreign and harmful. It does this by sending special cells to the organs
that are being affected by these things. These cells release chemicals that
produce inflammation around the foreign substance or substances to isolate
and destroy them.
In sarcoidosis, this inflammation remains and leads to the development of
granulomas or lumps.
Scientists have not yet identified the specific substance or substances
that trigger the immune system response in the first place. They also think
that sarcoidosis develops only if a person has inherited a certain combination
of genes.
A person cannot catch sarcoidosis from someone who has it.
More research is needed to discover what causes sarcoidosis.
Who is at risk?
Sarcoidosis affects people of all ages and races worldwide.
It occurs mostly in:
Adults between the ages of 20 and 40
African Americans (especially women)
People of Asian, German, Irish, Puerto Rican, and Scandinavian origin.
In the United States, sarcoidosis affects African Americans somewhat more
often and more severely than Caucasians.
Studies have shown that sarcoidosis is more likely to affect certain organs
in certain populations. For example,
Sarcoidosis of the heart and eye appears to be more common in Japan.
Painful skin lumps on the legs occur more often in people from Northern
Europe.
People who are more likely to get sarcoidosis include:
Health care workers
Nonsmokers
Elementary and secondary school teachers
People exposed to agricultural dust, insecticides, pesticides, or
mold
Firefighters.
Brothers and sisters, parents, and children of people who have sarcoidosis
are more likely than others to have sarcoidosis.
Signs and symptoms
Many people who have sarcoidosis have no symptoms. Often, the condition
is discovered by accident only because a person has a chest
X-ray for another reason, such as a pre-employment X-ray.
Some people have very few symptoms, but others have many.
Symptoms usually depend on which organs the disease affects.
Lung symptoms
Shortness of breath
A dry cough that doesn't bring up phlegm, or mucus
Wheezing
Pain in the middle of your chest that gets worse when you breathe
deeply or cough (rare).
Lymph node symptoms
Enlarged and sometimes tender lymph nodes – most often those
in the neck and chest but sometimes those under the chin, in the arm
pits, or in the groin.
Skin symptoms
Various types of bumps, ulcers, or, rarely, flat areas of discolored
skin, that appear mostly near the nose, eyes, back, arms, legs, and
scalp. They usually itch but aren't painful. They usually last a long
time.
Painful bumps that usually appear on the ankles and shins and can
be warm, tender, red or purple-to-red in color, and slightly raised.
This is called erythema nodosum. A person may have fever and swollen ankles and joint pain along with the bumps. The bumps often
are an early sign of sarcoidosis, but they occur in other diseases too.
The bumps usually go away in weeks to months, even without treatment.
Disfiguring skin sores that may affect your nose, nasal passages,
cheeks, ears, eyelids, and fingers. This is called lupus pernio. The
sores tend to be ongoing and can return after treatment is over.
Eye symptoms
Burning, itching, tearing, pain
Red eye
Sensitivity to light
Dryness
Floaters (i.e., seeing black spots)
Blurred vision
Reduced color vision
Reduced visual clearness
Blindness (in rare cases).
Heart symptoms
Shortness of breath
Swelling in the legs
Wheezing
Coughing
Irregular heartbeat, including palpitations (a fluttering feeling
of rapid heartbeats) and skipped beats
Sudden loss of consciousness
Sudden death.
Joint and muscle symptoms
Joint stiffness or swelling – usually in the ankles, feet, and
hands.
Joint pain.
Muscle aches (myalgias).
Muscle pain, a mass in a muscle, or muscle weakness.
Painful arthritis in the ankles that results from erythema nodosum.
It may need treatment but usually clears up in several weeks.
Painless arthritis that can last for months or even years. It should
be treated.
Bone symptoms
Painless holes in the bones.
Painless swelling, most often in the fingers.
Anemia that results from granulomas
affecting the bone marrow. This
usually should be treated.
Liver symptoms
Fever
Fatigue
Itching
Pain in the upper right part of the abdomen,
under the right ribs
Enlarged liver.
Parotid and other salivary gland symptoms
Swelling, which makes the cheeks look puffy
Excessive dryness in the mouth and throat.
Blood, urinary tract, and kidney symptoms
Increased calcium in the blood or urine,
which can lead to painful kidney stones
Confusion
Increased urination.
Nervous system symptoms
Headaches.
Vision problems.
Weakness or numbness of an arm or leg.
Coma (rare).
Drooping of one side of the face that results from sarcoidosis affecting
a facial nerve. This can be confused
with Bell's palsy, a disorder that
may be caused by a virus.
Paralysis of your arms or legs that results from sarcoidosis affecting
the spinal cord.
Weakness, pain, or a "stinging needles" sensation in areas where many
nerves are affected by sarcoidosis.
Pituitary gland symptoms (rare)
Headaches
Vision problems
Weakness or numbness of an arm or leg
Coma (rare).
Other symptoms
Nasal obstruction or frequent bouts of sinusitis.
Enlarged spleen, which leads to a decrease in platelets in the blood
and pain in the upper left abdomen. Platelets are needed to help the
blood clot.
Sarcoidosis may also cause more general symptoms, including:
Uneasiness, feeling sick (malaise), an overall feeling of ill health
Tiredness, fatigue, weakness
Loss of appetite or weight
Fever
Night sweats
Sleep problems
These general symptoms are often caused by other conditions. If a person
has these general symptoms but doesn't have symptoms from affected organs,
he or she probably does not have sarcoidosis.
Diagnosis
Sarcoidosis is diagnosed by taking a detailed medical history and conducting
a physical exam and several diagnostic tests. The purpose is to:
Identify the presence of granulomas in any of the organs.
Rule out other causes of the symptoms.
Determine the amount of damage to any of the affected organs.
Determine whether a person needs treatment.
Medical history
A doctor will ask for a detailed medical history. He or she will want to
know about any family history of sarcoidosis and what jobs a person has
had that may have increased their chances of getting sarcoidosis.
The doctor may also ask whether a person has ever been exposed to inhaled beryllium metal, which is used in aircraft
and weapons manufacture, or organic dust from birds or hay. These things
can produce granulomas in the lungs that look like the granulomas that are
caused by sarcoidosis but are actually signs of other conditions.
Physical exam
A doctor will look for symptoms of sarcoidosis, such as red bumps on the
skin; swollen lymph nodes; an enlarged liver, spleen, or salivary gland(s);
or redness in the eyes. He or she will also listen for abnormal lung sounds
or heart rhythm, and will check for other likely causes of the symptoms.
Diagnostic tests
There is no one specific test for diagnosing sarcoidosis. It is harder to
diagnose sarcoidosis in some organs (e.g., heart, nervous system) than in
others. A doctor will probably conduct a variety of tests and procedures
to help in the diagnosis.
These include:
chest X-ray. A chest X-ray
takes a picture of the heart and lungs. It may show granulomas or enlarged
lymph nodes in the chest. About 95 out of every 100 people who have
sarcoidosis have an abnormal chest X-ray.
Doctors usually use a staging system for chest X-rays taken to detect
sarcoidosis:
Stage 0: Normal chest X-ray
Stage 1: Chest X-ray showing enlarged lymph nodes but otherwise
clear lungs
Stage 2: Chest X-ray showing enlarged lymph nodes and shadows
in the lungs
Stage 3: Chest X-ray showing shadows in the lungs, but the lymph
nodes are not enlarged
Stage 4: Chest X-ray showing scars in the lung tissue.
In general, the higher the stage of the X-ray, the worse the symptoms
and lung function are. But there are a lot of differences among people.
If the X-ray results show Stages 0, 1, 2, or 3, the patient may not
have symptoms or need treatment, and may get better and have normal
chest X-rays again over time.
blood tests. These tests
can show the number and type of cells in the blood. They also will show
whether there are increases in the calcium levels or changes in the
liver, kidney, and bone marrow that can occur with sarcoidosis.
lung function tests.
One test uses a spirometer, a device that measures how much and how
fast a person can blow air out of their lungs after taking a deep breath.
If there is a lot of inflammation and/or scarring in the lungs, a person
will not be able to move normal amounts of air in and out.
Another test measures how much air the lungs can hold. Sarcoidosis can
cause the lungs to shrink, and they will not be able to hold as much
air as healthy lungs.
electrocardiogram (EKG).
This test will help show if the heart is affected by sarcoidosis.
pulse oximetry. A small
clip attached to the finger tip can show how well the heart and lungs
are moving oxygen into the blood.
Arterial blood
gas test. This test is more accurate than pulse oximetry for
checking the level of oxygen in the bloodstream. Blood is taken from
an artery (usually in the wrist). It
is then analyzed for its oxygen and carbon dioxide levels.
fiberoptic bronchoscopy.
In this procedure, a doctor inserts a long, narrow, flexible tube with
a light on the end through the nose or mouth into the lungs to look
at your airways. This tube is called a bronchoscope. A person most likely
would have this procedure as an outpatient in a hospital under local anesthesia.
Bronchoalveolar lavage (BAL). During bronchoscopy, a doctor
may inject a small amount of salt water (saline) through the bronchoscope
into the lungs. This fluid washes the lungs and helps bring up cells
and other material from the air sacs deep in the lungs where the inflammation
usually starts to develop. The cells and fluid are then examined for
signs of inflammation.
biopsy. A doctor may take a
small sample of tissue from one of the affected organs. For example,
when breathing tests or chest X-rays show signs of sarcoidosis in the
lungs, a doctor may do a fiberoptic bronchoscopy biopsy. This will help
confirm the diagnosis. Tiny forceps as inserted through the bronchoscope
to collect tissue that will be examined. Because the granulomas may
be spread out in the lungs, the bronchoscope may miss some of them.
Biopsies of the skin and liver are sometimes done to detect granulomas
in these organs.
A person may have sarcoidosis in other organs as well and multiple biopsies
may be necessary. However, every organ involved does not need to be
biopsied for a diagnosis to be made.
computed tomography
(CT) scan. This test provides a computer-generated image of
the organs that has more detail than a regular chest X-ray. It can provide
more information about how sarcoidosis has affected an organ.
A doctor may do a CT scan to:
Obtain more information about how much of the lung is affected
by sarcoidosis.
Detect sarcoidosis in the liver. A CT scan of the abdomen will
show if the liver is enlarged and if there is a pattern suggesting
granulomas.
magnetic resonance
(MR) scan. This test is also called nuclear magnetic resonance
(NMR) scanning or magnetic resonance imaging (MRI). This scan uses powerful
magnets and radio waves to make images of some of the organs that a
doctor doesn't want to risk doing a biopsy on. For example, an MR scan
can be used to diagnose sarcoidosis in the brain, spinal cord, nerves,
or heart.
thallium and gallium scans. These scans are often done to see if sarcoidosis is affecting
the heart. Thallium and gallium are radioactive elements. A doctor injects
a small amount of one of them into the patient's vein in the arm. The
elements collect at places in the body where there is inflammation.
After a while, the body is scanned for radioactivity. Increased radioactivity
at any place may be a sign of inflammation.
This test gives information on the tissue in the body that has been
affected by sarcoidosis and the amount of damage to it. But since this
test shows all inflammation in the body, even inflammation caused by
conditions other than sarcoidosis, it does not give a definite diagnosis
of sarcoidosis.
positron emission
tomography (PET) scan. This test also uses radioactive injections.
It may be more sensitive than gallium in detecting areas of inflammation.
Some doctors are using it instead of gallium scans.
Your doctor may not need to find every one of the organs affected by
sarcoidosis, only those that cause symptoms. Often the organs affected
by the condition continue to function well and don't need to be treated.
Treatment
The goals of treatment are to:
Improve how the organs affected by sarcoidosis work
Relieve symptoms
Shrink the granulomas.
Treatment may shrink the granulomas and even cause them to disappear, but
this may take many months. If scars have formed, treatment may not help,
and a person may have ongoing symptoms.
A person's treatment depends on:
What symptoms he or she has
How severe the symptoms are
Whether any of the vital organs (e.g., the lungs, eyes, heart, or
brain) are affected
How the organ is affected.
Some organs must be treated, regardless of the symptoms. Others may not
need to be treated. Usually, if a person doesn't have symptoms, he or she
doesn't need treatment, and they probably will recover in time.
Drugs
The main treatment for sarcoidosis is prednisone.
Prednisone is a corticosteroid, or
anti-inflammatory drug. Sometimes it is used with other drugs. Sometimes
other corticosteroids are used.
Prednisone almost always relieves symptoms of inflammation. If a symptom
doesn't improve with prednisone treatment within a couple of months, consult
your physician.
Prednisone is usually given for many months, sometimes for a year or more.
Low doses of prednisone can often relieve symptoms without causing major
side effects.
When used at high doses, prednisone can cause serious side effects.
Side effects can include:
Weight gain.
Diabetes.
High blood pressure.
Mood swings (depression).
Difficulty sleeping at night.
Heartburn.
Acne.
Thinning of the skin and bones (called osteoporosis).
Cataracts.
Glaucoma.
Adrenal gland insufficiency, which occurs when the adrenal
glands don't make enough of certain hormones. This requires treatment
by an endocrinologist, a doctor who specializes in the diagnosis and
treatment of the endocrine glands. The endocrine glands include the
adrenal and pituitary glands.
Aseptic or avascular necrosis of the hip, the development of cysts
and hardened and dead tissue in the hip. A doctor can usually help a
person manage these side effects.
When it is time to stop taking prednisone, a person should cut back slowly,
with a doctor's help. This will help prevent flare-ups of sarcoidosis and
allow the body to adjust to life without the drug.
A person may also want to see an endocrinologist to make sure that the endocrine
glands are making enough hormones. The endocrinologist may prescribe certain
hormones for the patient to take until their endocrine glands are working
well again.
Other drugs used to treat sarcoidosis
Other drugs are sometimes used to treat sarcoidosis. A doctor may prescribe
one of them if:
A person's condition gets worse while they are taking prednisone
A person can't stand the side effects of prednisone.
Most of these other drugs are immune system suppressants. This means that
they prevent the immune system from fighting things like bacteria and viruses.
As a result, a person may have a greater chance of getting infections.
Most of these drugs also can cause serious side effects. Some also could
increase the chances of getting cancer, especially if they are taken at
high doses.
A person and his or her doctor must weigh living with the symptoms of sarcoidosis
against the side effects of the drugs.
Some drugs work better than others for different people.
A person may be given more than one drug.
Some drugs used to treat sarcoidosis are taken by mouth. Others are applied
locally to an affected area.
Local therapy is the safest way to treat sarcoidosis. The drug is applied
directly to the affected area. As a result, only small amounts of the drug
reach other parts of the body.
Drugs used for local therapy include:
Eye drops
Inhaled drugs for the lungs
Skin creams.
Drugs can be used locally only if the affected area is easily reached. For
instance, inhaled steroids can ease coughing and wheezing in the upper airways,
but they don't seem to relieve these symptoms when the affected lung tissue
is deep within the chest.
A person should talk with their doctor about these treatments and the side
effects that may occur.
The other drugs used to treat sarcoidosis include:
hydroxychloroquine (Plaquenil). This drug can usually help
people who have sarcoidosis in the skin or a high level of calcium in
their blood. This drug can irritate the stomach. It also can cause eye
problems. Before starting on this drug, a person should see an ophthalmologist,
or eye doctor, for some baseline tests. Once a person starts taking
it, they should have their eyes examined every 6 months.
methotrexate. This drug is taken once a week by mouth or injection
and usually takes up to 6 months to relieve symptoms. This drug may
cause side effects, especially if taken in high doses. These include:
Nausea.
Mouth sores.
A decrease in infection-fighting white blood cells. A person then
has a greater chance of getting an infection. If this drug is taken,
a person should have regular blood tests to check the levels of
their white blood cells.
An allergic reaction in the lungs that goes away when the person
stops taking the drug. This is extremely rare.
Liver damage. This is the most serious side effect. If methotrexate
is taken, a person should be monitored regularly by a physician.
If a person is pregnant, they should not take this drug. Taking folic
acid can help reduce the chances of having bad side effects from
methotrexate.
azathioprine (Imuran). This drug may work in about half of
the people who have sarcoidosis. It is usually taken for at least 6
months. Side effects include:
Nausea
Reduced white blood cell levels, which increases a person's chances
of getting an infection.
This drug has caused cancer in some people, especially when they have
taken it at high doses. It should not be taken by patients who are pregnant.
cyclophosphamide (Cytoxan). This is a very toxic drug. It
is rarely used to treat sarcoidosis. It is given only to people who
have serious forms of sarcoidosis, such as sarcoidosis in their central
nervous system (neurosarcoidosis). This drug is more likely to cause
nausea and reduce the white blood cell levels than either methotrexate
or azathioprine. A doctor should check the white blood cell levels often
while a person is taking this drug to make sure they have a high enough
level to fight infection. Cyclophosphamide can also irritate the bladder.
Some people who have taken it for more than 2 years have developed bladder
cancer. It should not be taken during pregnancy. Cyclophosphamide can
be given intravenously (through one of the veins), which lessens some
of its side effects, but this doesn't reduce the risk of cancer.
Treatments for specific types of sarcoidosis
eyes. Sarcoidosis in the eyes almost always responds well
to treatment. Often, the only treatment needed is eye drops containing
corticosteroids. A person should have yearly eye exams, even if they
think their eyes are doing well.
spleen. Sarcoidosis can cause the spleen to enlarge. This
can lead to a decrease in the red or white blood cells or platelets
and increase the chances of infection and blood
clotting disorders. Treatment is usually given to increase the number
of blood cells and ease pain. In rare cases, the spleen may need to
be removed.
liver. Sarcoidosis rarely causes permanent liver damage. As
a result, the liver usually isn't treated unless it's causing major
symptoms (e.g., fever). Drug treatment can usually reduce granulomas
in the liver. Liver transplantation has been successful in those rare
cases in which the condition has become worse. Follow-up care includes
regular blood tests to find out how well your liver is working. A person
should check with their doctor to find out how often they need these
tests.
nervous system. Sarcoidosis in the nervous system (neurosarcoidosis)
usually needs treatment. Nerve tissue heals slowly, so treatment often
takes a long time. A person may need to take several drugs at high doses.
erythema nodosum. These painful bumps on the shins often go
away in weeks to months without treatment. A doctor probably will not
give medication unless a person is very uncomfortable. Aspirin or ibuprofen, an anti-inflammatory
drug that can be bought without a prescription, will usually help.
heart. Sarcoidosis in the heart is usually treated with steroids.
Heart drugs may also be given to improve the heart's pumping ability
or to correct a disturbed heart rhythm. If a person has a severe heart
rhythm disturbance, their doctor may prescribe one of these devices:
A cardiac pacemaker, a small
battery-operated device, often put under the skin, that regulates
the heartbeat
A defibrillator, an implanted device that shocks the heart into
a normal heartbeat or, if it has stopped, into beating.
If the heart is severely affected and doesn't respond to treatment,
a transplant may be done. But this is rarely needed.
lupus Pernio. This rash on the face, especially the cheeks
and nose, can be distressing because it's in a very visible area. It
often occurs with loss of the sense of smell,
nasal stuffiness, and sinus infections. Options for treatment include:
Local treatment with skin creams
Oral drugs (plaquenil or prednisone, for example)
Local injections of steroid preparations.
Lupus pernio is often treated by dermatologists, doctors who specialize
in skin diseases, working with a sarcoidosis specialist. Because sarcoidosis
varies so much among different people, a doctor may find it hard to
tell whether the treatment is helping.
Other drugs being studied for use in treating sarcoidosis
Scientists also are studying drugs that are used for other conditions to
see if they can help people who have sarcoidosis. These drugs include:
Etanercept (Enbrel). This drug is an immune system suppressant.
It's injected under the skin to reduce symptoms of rheumatoid arthritis.
It may also be used to treat psoriasis or ankylosing spondylitis, a
type of arthritis that affects the joints in the spine. Early studies
suggest that it will not be useful in treating sarcoidosis, but research
is ongoing.
Infliximab (Remicaide). This drug is an immune system suppressant.
It's injected into a vein in the arm. It's used to treat Crohn's Disease,
rheumatoid arthritis, and ankylosing spondylitis. Some studies have
shown it to help sarcoidosis patients who also have lupus pernio, eye
disease, or neurosarcoidosis. This drug has serious side effects but
may improve lung function in some people who aren't helped by corticosteroids.
More research is needed.
Pentoxifylline. This drug is an immune system suppressant.
Stomach and gastrointestinal side effects are common. Early studies
show that it has helped some people who have sarcoidosis in their lungs
reduce their doses of prednisone while taking it. More research is needed.
Tetracycline. Tetracycline antibiotics are used to treat Lyme
Disease, some types of pneumonia,
and acne. A few small studies suggest that they may help in treating
sarcoidosis in the skin. Research is ongoing.
Thalidomide. This immune system suppressant can cause bad
side effects. It is effective against other conditions that involve
granulomas of the skin (e.g., leprosy, tuberculosis).
Scientists are studying this drug to see if it can be used to treat
sarcoidosis in the skin.
The future
Scientists worldwide are trying to learn more about sarcoidosis and how
to improve its diagnosis and treatment. Some recent studies have led to
possible new treatments, which, in turn, are being studied. Current research
includes studies of:
The agent or agents that cause sarcoidosis
Why sarcoidosis seems to act differently in people of different races
Why sarcoidosis appears in some families
How genes, passed from one generation to another, may make some people
more likely than others to develop sarcoidosis
How cells act and communicate with each other to cause sarcoidosis
symptoms.
Living with sarcoidosis
A person should take steps to stay healthy. This includes:
Not smoking.
Avoiding substances like dusts and chemicals that can harm the lungs.
Trying to follow a healthy eating plan.
Being as active as possible without straining.
Joining a patient support group may help adjust to living with sarcoidosis.
Talking to others who have the same symptoms can help a person see how they
have coped with them.
A patient's regular doctor may be able to diagnose and treat the sarcoidosis,
but diagnosis and treatment by a doctor who specializes in sarcoidosis is
recommended. If a person prefers to use their regular doctor, they should
see a doctor who specializes in the organs that are affected by their sarcoidosis
at least once. For example, an ophthalmologist should be seen if the eyes
are affected or a pulmonologist if the sarcoidosis is in the lungs. These
specialists are often found at major medical centers. They will work with
a person's regular doctor to help make a diagnosis, develop a treatment
plan, and schedule periodic exams and lab tests.
Pregnancy
Many women give birth to healthy babies while being treated for sarcoidosis.
Pregnancy usually doesn't affect the course of sarcoidosis, and person can
continue corticosteroid treatment through their pregnancy. None of the other
drugs are recommended for use during pregnancy.
Sometimes sarcoidosis may get worse after the baby is delivered.
Women with severe sarcoidosis, especially if they are older, may have trouble
becoming pregnant.
It's important for a person to discuss this issue with their doctor. A patient
who becomes pregnant should be sure to get both good prenatal care and regular
sarcoidosis checkups during and after pregnancy.
Follow-up care
Regular follow-up care is important, even if a person isn't taking medication
for their sarcoidosis. New symptoms can occur at any time, and the condition
can get worse slowly, without the person noticing.
Follow-up exams usually include:
A review of the symptoms
A physical exam
A chest X-ray and CT scan
Breathing tests
An eye exam
Blood tests
An electrocardiogram (EKG).
The frequency of examinations and tests depends on:
How severe the symptoms are
Which organs were affected at diagnosis
What treatment is being used
Any complications that may develop during treatment.
A person will probably need routine followup care for several years. Whether
they see their regular doctor or a sarcoidosis specialist for this depends
on the symptoms during the first year of follow-up.
Here are some examples of how follow-up care can be managed. They are based
on either the person's condition at the time of diagnosis with sarcoidosis
or the treatment used.
Follow-up after initial diagnosis
If at diagnosis, there are no symptoms, a normal breathing test, and
an abnormal chest X-ray:
A person should plan on having a follow-up exam every 6 to 12 months
until their condition is stable or improving.
A breathing test may need to be repeated. The need to repeat it
depends on the symptoms and ability to be active.
If at the first follow-up visit, there are no new symptoms and the
chest X-ray is normal, a person can go to their regular doctor for future
follow-up care.
If at diagnosis, there are some symptoms, an abnormal chest X-ray,
but a person doesn't need treatment:
They should plan on having a follow-up exam in 3 to 6 months.
If at the follow-up exam, a person's condition has become worse (i.e.,
there are now more symptoms, an abnormal X-ray, or abnormal lab tests)
they may need treatment.
If treatment is started, follow-up tests may be needed more often.
Follow-up based on the drug treatment
If treatment is begun with prednisone:
Checks should be carried out for the side effects of high blood
pressure, too much weight gain, diabetes, loss of calcium from the
bones, and pain in one or both hips.
If treatment is begun with hydroxychloroquine:
An eye exam should be performed every 6 months while taking this
drug.
If treatment is begun with methotrexate:
Blood tests should be done every month or every other month to
see if there is anemia, low white blood cell or platelet levels,
or liver inflammation.
Other follow-up tests
Depending on how serious the condition is and what organs are affected,
certain tests may need to be done regularly.
Eye tests
Everyone who is diagnosed with sarcoidosis, even if they don't have eye
symptoms, should see an ophthalmologist (eye doctor) for eye tests. This
is important because there may be eye damage even if there are no symptoms.
These tests may include:
A slit lamp examination. An instrument with a high-intensity light
source is used to look at the front of the eyes.
A visual fields examination. The patient will be asked to look at
a light through an instrument.
Inspection of the retina and optic nerve.
If eye symptoms develop, a doctor will have you repeat the tests.
A person should also have regular eye exams if they are being treated with:
Chloroquine or hydroxycholoroquine (Plaquenil)
Corticosteroids.
Breathing tests
These tests are used to check the course of sarcoidosis in the lungs. The
results are compared over time.
Blood tests
A blood test for calcium should be done. If the calcium level is high, treatment
is probably needed. A person also should not take vitamin and mineral supplements
containing calcium or vitamin D, and should
avoid too much exposure to the sun.
Electrocardiogram
This test is needed to make sure that the heart is still not affected by
sarcoidosis. The heart can be affected at any time if the sarcoidosis is
active.