varicose veins
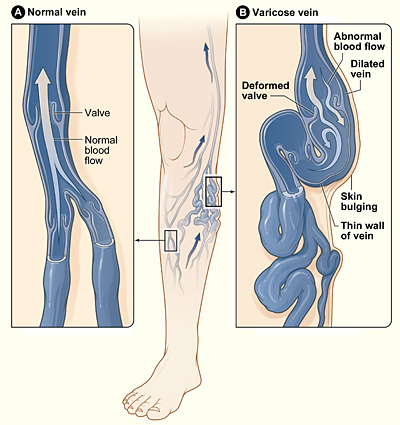
The illustration shows the location of leg veins, which can become varicose veins. Figure A shows a normal vein with working valves and normal blood flow. Figure B shows a varicose vein with deformed valves, abnormal blood flow, and thin, dilated (stretched) walls.
Varicose veins are swollen and twisted veins that are visible just under the surface of the skin. They appear most commonly in the legs, but also can develop in other parts of the body.
Veins are blood vessels that carry blood from the tissues of the body to the heart. In the heart, blood is pumped to the lungs to pick up oxygen. The oxygen-rich blood is then pumped out to the body through the arteries. From the arteries, blood flows through tiny blood vessels called capillaries, where it gives up its oxygen to the body's tissues. The blood then returns back to the heart through the veins to pick up more oxygen.
Veins have one-way valves that help to keep the blood flowing toward the heart. When the valves don't work well, blood backs up and pools in the veins. This causes them to swell and become varicose veins.
Varicose veins usually don't cause medical problems. On occasion, they require treatment for pain, skin problems, blood clots, or other complications. People may choose to have cosmetic treatment to improve the appearance of varicose veins.
Related vein problems
A number of other types of vein problems are related to varicose veins.
Spider veins
Spider veins are a smaller version of varicose veins. They occur in the capillaries, which are the smallest blood vessels in the body. Spider veins are commonly found on the legs and face, and they usually resemble a spider web or tree branch in shape. They can be red or blue. Spider veins are usually not a medical concern.
Telangiectasias
Telangiectasias are small clusters of blood vessels that look similar to spider veins. They are red in color and are commonly found on the upper body, including the face. They can develop during pregnancy and in people who have certain genetic disorders, viral infections, and other medical conditions (such as liver disease). Newly developed telangiectasias are often a reason to see a doctor.
Venous lakes
Venous lakes are another type of varicose veins in which blood collects in the veins of the face and neck.
Reticular veins
Reticular veins are flat blue veins commonly seen behind the knees.
Hemorrhoids
Hemorrhoids are varicose veins in blood vessels in and around the anus.
Varicoceles
Varicoceles are varicose veins in the scrotum (the skin over the testicles). Varicoceles may be linked to male infertility and should be checked by a doctor.
Outlook
People with varicose veins often require only simple self-care measures, such as performing certain leg exercises, wearing compression stockings, and avoiding long periods of sitting or standing. For those who are concerned about the appearance of varicose veins, several cosmetic treatments are available. Although uncommon, in some cases, complications such as pain, skin ulcers, and blood clots can develop. A variety of medical and surgical procedures are used to treat varicose veins in these more complicated cases.
Causes
Veins, especially those in the legs, have to pump the blood "up hill" to the heart, against gravity. Inside the veins are one-way valves that help with pumping action and prevent blood from flowing backward. These valves allow blood to flow in only one direction, toward the heart. Varicose veins develop when the valves become weakened, damaged, or don't work well.
Weakness in the valves may be due to weakness in the walls of the veins. This weakness tends to be associated with certain factors, including increasing age, a family history of varicose veins, or high pressure inside veins due to overweight or pregnancy.
When the walls of the veins are weak, they lose their normal elasticity, like an overstretched rubber band. This makes them longer and wider and causes the flaps of the valves to separate. Blood is then able to flow backward through the valves, filling the vein and stretching it even more. The vein becomes enlarged, swollen, and often twisted trying to squeeze into its normal space.
Who is at risk?
Populations affected
About 25 million Americans are affected by varicose veins. They are most common in people aged 30 to 70.
Risk factors
Risk factors for developing varicose veins include:
Signs and symptoms
Common signs and symptoms of varicose veins include:
Complications
Only a small percentage of people have complications from varicose veins. Complications may include dermatitis and thrombophlebitis.
Dermatitis
Dermatitis is an itchy rash that can occur on the lower leg or ankle of a person with varicose veins in the legs. It can sometimes cause bleeding or a skin ulcer to develop if scratched or irritated.
Thrombophlebitis
This is a blood clot (thrombus) that occurs in a vein. There are two types of thrombophlebitis:
Diagnosis
Varicose veins are often diagnosed based simply on the appearance of the veins. For varicose veins in the legs, your doctor will examine your legs while you are standing or seated with your legs dangling. Your doctor may also ask you to describe pain or any other symptoms. Some diagnostic tests may be done to rule out other disorders or conditions.
Specialists involved
The following specialists may be involved in your medical care if you have varicose veins:
Diagnostic tests and procedures
Your doctor may order a Doppler ultrasound to evaluate the flow of blood in your veins and to look for blood clots. During a Doppler ultrasound, a handheld device is placed on your body and passed back and forth over the affected area. A computer converts sound waves into a picture of the blood flow in the arteries and veins.
Rarely, your doctor may order an angiogram to look at blood flow through your blood vessels. The procedure involves injecting a dye into your veins that can be seen using X-ray. An angiogram can help to rule out other diagnoses besides varicose veins.
Treatment
Goals of treatment
The goals of treating varicose veins may include easing symptoms, avoiding complications, and improving cosmetic appearance. Although treatment can target existing varicose veins, it can't keep new varicose veins from forming.
Who needs treatment
Varicose veins that cause few signs and symptoms usually don't need to be treated. Instead, your doctor may recommend simple self-care measures. Varicose veins causing more severe signs and symptoms may need medical or surgical treatment. Treatment may be recommended when the varicose veins are causing skin ulcers, serious skin conditions, blood clots, significant pain, or disruption of daily life activities. Some people with varicose veins may choose to have medical or surgical treatments to improve the cosmetic appearance of varicose veins.
Types of treatment
Self-care measures
Self-care measures are a common option for treating varicose veins. If self-care measures are called for, your doctor may ask you to:
Medical and surgical treatments
Medical and surgical treatments are used to either remove varicose veins or close them. Removing or closing varicose veins usually doesn't create circulation problems because the blood reroutes itself through other veins. These therapies range from approaches that don't involve incisions or injections to those that are surgical procedures. It may be necessary to combine therapies, depending on your condition and lifestyle.
Sclerotherapy. This procedure uses a liquid chemical to close off the vein. The solution is injected into the vein to cause irritation and scarring inside the vein, which causes the vein to close off and fade away. It's usually used to treat smaller varicose veins and spider veins. Sclerotherapy is usually done in the doctor's office, while you stand. You may need several sclerotherapy treatments to close off a vein completely. In this case, treatments are typically given every 4 to 6 weeks. Following treatments, your legs are wrapped in elastic bandaging to help healing and decrease swelling.
Microsclerotherapy. This procedure is used to treat spider veins and other very small varicose veins. It involves injection of small amounts of a liquid chemical using a very fine needle. The chemical causes scarring in the inner lining of the veins, causing them to close off.
Laser surgery. This procedure uses no incisions or injections. Light energy from a laser is used to make the vein fade away. Laser surgery is typically used to treat smaller varicose veins. With new technology, lasers are more effective than they used to be.
Endovenous ablation therapy. This procedure uses an energy source (either laser or radiowave) to create heat to close off the vein. A tiny incision is made in the skin, and a small catheter (tube) is inserted into the vein. A device at the tip of the catheter heats up the inside of the vein, which causes it to close off. You're awake during the procedure, but your doctor numbs the area of the vein. You can usually go home on the same day. You may experience less pain and recover more quickly with this procedure than with some of the others.
Endoscopic vein surgery.
This procedure uses a tiny camera at the end of a thin tube (an endoscope) to move through the varicose veins. A surgical instrument at the end of the camera is used to close the veins. Endoscopic vein surgery is currently only used in severe cases in which there are skin ulcers due to the varicose veins. Only small incisions are required for this procedure.
Ambulatory phlebectomy. In this procedure, small varicose veins are removed through small incisions in your skin. Ambulatory phlebectomy is typically used to treat varicose veins close to the surface of the skin. You're awake during the procedure, but your doctor numbs the area of the vein. You can usually go home the same day.
Vein stripping and ligation. In this procedure, veins are tied shut (ligation) and removed (stripping) through small incisions. The procedure is typically used in severe cases, in which the varicose veins cause pain or skin ulcers. You're given medicine to sleep so that you don't feel any pain during the procedure.
After treatment
Recovery times vary based on the specific procedure that's performed. Vein stripping and ligation requires more recovery than most other procedures. Activity is not significantly limited following most other procedures. In fact, walking is often recommended during recovery. Some treatments may require that you wear compression stockings or bandages for a period ranging from a couple days to a few weeks following the procedure.
Common side effects immediately following a procedure may include bruising, swelling, skin discoloration, cramping, and itching. Swelling and skin discoloration may last for several months. Less common side effects include blood clots or nerve damage. An uncommon side effect of sclerotherapy is liquid chemical leaking out of the vein, which could cause tissue damage or ulcers.
Prevention
Varicose veins can't be prevented from forming, but there are ways to reduce the severity of existing varicose veins and the risk of getting new varicose veins. To decrease the risk for and severity of varicose veins, you can:
Living with varicose veins
Varicose veins can typically be treated with self-care. If medical procedures are necessary, they are generally very effective, and treated veins eventually fade or disappear. But the treatments don't prevent new varicose veins or other vein problems. It's possible for the same varicose veins to reappear after treatment, but this is uncommon.
Ongoing health care needs
Although it's not possible to completely prevent new varicose veins from forming, following the steps in the "How Can Varicose Veins Be Prevented?" section can help keep developing or worsening varicose veins under control. Watch for skin ulcers or other complications that may develop, and consult a doctor if this happens.


