coronary artery bypass grafting
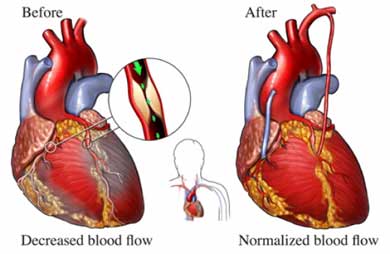
Coronary artery bypass graft. © 2005 Nucleus Communications.
Coronary artery bypass grafting (CABG) is a type of surgery called revascularization, used to improve blood flow to the heart in people with severe coronary artery disease (CAD). It is also called heart bypass surgery.
CAD occurs when the arteries that supply blood to the heart muscle (the coronary arteries) become blocked due to the buildup of a material called plaque (plak) on the inside of the blood vessels. If the blockage is severe, chest pain (also called angina), shortness of breath, and, in some cases, heart attack can occur.
CABG is one treatment for CAD. During CABG, a healthy artery or vein from another part of the body is connected, or grafted, to the blocked coronary artery. The grafted artery or vein bypasses (that is, it goes around) the blocked portion of the coronary artery. This new passage routes oxygen-rich blood around the blockage to the heart muscle. As many as four major blocked coronary arteries can be bypassed during one surgery.
Overview
CABG is the most common type of open-heart surgery in the United States, with more than 500,000 surgeries performed each year. Doctors called cardiothoracic surgeons perform this surgery.
CABG isn't used for everyone with CAD. Many people with CAD can be treated by other means, such as lifestyle changes, medicines, and another revascularization procedure called angioplasty.
CABG may be an option if you have severe blockages in the large coronary arteries that supply a major part of the heart muscle with blood – especially if the heart's pumping action has already been weakened.
CABG may also be an option if you have blockages in the heart that can't be treated with angioplasty. In these situations, CABG is considered more effective than other types of treatment.
If you're a candidate for CABG, the goals of having the surgery are to:
Repeat surgery may be needed if grafted arteries or veins become blocked, or if new blockages develop in arteries that weren't blocked before. Taking medicines as prescribed and making lifestyle changes that your doctor recommends can lower the chance of a graft becoming blocked.
In people who are candidates for the surgery, the results are usually excellent, with 85 percent of people having significantly reduced symptoms, less risk for future heart attacks, and a decreased chance of dying within 10 years following the surgery.
Who needs coronary artery bypass grafting?
Coronary artery bypass grafting (CABG) is only used to treat people who have severe coronary artery disease (CAD) that could lead to a heart attack.
Your doctor may recommend CABG if other treatments, such as lifestyle changes or medicines, haven't worked. He or she also may recommend CABG if you have severe blockages in the large coronary arteries that supply a major part of the heart muscle with blood – especially if your heart's pumping action has already been weakened.
CABG also may be a treatment option if you have blockages in the heart that can't be treated with angioplasty.
Your doctor will determine if you're a candidate for CABG based on a number of factors. These include the presence and severity of CAD symptoms, the severity and location of blockages in your coronary arteries, your response to other treatments, your quality of life, and any other medical problems you may have.
In some cases, CABG may be performed on an emergency basis, such as pending or during a heart attack.
Physical exam and diagnostic tests
To determine if you're a candidate for CABG, your doctor will do a physical exam that involves checking your cardiovascular system, focusing on heart, lungs, and pulse. Your doctor also will ask you about any symptoms you have, such as chest pain or shortness of breath, and how long, how often, and how severe they are.
Medical tests will be done to find out which arteries are clogged, how much they're clogged, and whether there's any heart damage. Tests may include:
During exercise stress testing, your blood pressure and EKG readings are monitored while you walk or run on a treadmill or pedal a bicycle. Other heart tests, such as nuclear heart scanning or echocardiography, also can be done at the same time. These would be ordered if your doctor needs more detailed information on blood flow and the heart's pumping action than the exercise stress test can provide.
If you are unable to exercise, a medicine can be injected through an intravenous line (IV) into your bloodstream to make your heart work harder and beat faster, as if you are exercising on a treadmill or bicycle. Nuclear heart scanning or echocardiography is then usually done. During nuclear heart scanning, radioactive tracer is injected into your bloodstream, and a special camera shows the flow of blood through your heart and arteries. Echocardiography uses sound waves to show blood flow through the chambers and valves of your heart and to show how well your heart pumps.
Your doctor also may order two newer tests along with stress testing if more information is needed about how well your heart works. These new tests are magnetic resonance imaging (MRI) and positron emission tomography (PET) scanning of the heart. MRI shows detailed images of the structures and beating of your heart, which may help your doctor better assess if parts of your heart are weak or damaged. PET scanning shows the level of metabolic activity in different areas of your heart. This can help your doctor determine if enough blood is flowing to the areas of your heart. A PET scan can show decreased blood flow caused by disease or damaged muscles that may not be detected by other scanning methods.
There are several different types of echocardiograms, including a stress echocardiogram. During this test, an echocardiogram is done both before and after your heart is stressed either by having you exercise or by injecting a medicine into your bloodstream that makes your heart beat faster and work harder. A stress echocardiogram is usually done to find out if you have decreased pumping action of your heart (CAD).
Other considerations
When deciding if you're a candidate for CABG, you doctor will also consider your:
Medicines and other medical procedures may be tried before CABG. Medicines that lower cholesterol levels and blood pressure and improve blood flow through the coronary arteries are often tried.
A procedure called coronary angioplasty (also called balloon angioplasty) may be tried. During this procedure, a thin tube with a balloon or other device on the end is threaded through a blood vessel in your groin (upper thigh) or arm up to the narrowed or blocked coronary artery. Once in place, the balloon is inflated to push the plaque against the wall of the artery, widening the artery and restoring the flow of blood through it. In many cases, after the initial balloon angioplasty, a tiny mesh tube called a stent is inserted permanently in the area to keep the artery open.
Before coronary artery bypass grafting
Tests may be done to prepare you for coronary artery bypass grafting, including blood tests, EKG, echocardiogram, chest X-ray, cardiac catheterization, and angiography.
Your doctor will give you specific instructions about how to prepare for surgery. There will be instructions about what to eat or drink, what medicines to take, and what activities to stop (such as smoking). You will likely be admitted to the hospital on the same day as the surgery.
During coronary artery bypass grafting
Coronary artery bypass grafting (CABG) requires a team of experts. A cardiothoracic surgeon performs the surgery with support from an anesthesiologist, perfusionist (heart-lung machine specialist), other surgeons, and nurses.
There are several different types of CABG. They range from traditional surgery in which the chest is opened to reach the heart, to a nontraditional surgery in which small incisions are made to bypass the narrowed artery.
Traditional coronary artery bypass grafting
This type of surgery usually lasts 3 to 5 hours, depending on the number of arteries being bypassed. Numerous steps take place during traditional CABG.
Anesthesia is given to put you to sleep. During the surgery, the anesthesiologist monitors your heartbeat, blood pressure, oxygen levels, and breathing. A breathing tube is placed in your lungs through your throat, and connected to a ventilator (breathing machine).
An incision is made down the center of your chest. The chest bone is then cut and your rib cage is opened so that the surgeon can get to your heart.
Medicines are used to stop your heart, which allows the surgeon to operate on it while it's not beating. A heart-lung machine keeps oxygen-rich blood moving throughout your body. An artery or vein is taken from a different part of your body, such as your chest or leg, and prepared to be used as a graft for the bypass. In surgery with several bypasses, a combination of both artery and vein grafts is commonly used.
The surgeon uses wires that stay in your body permanently to close your chest bone and stitches or staples to close the skin incision. The breathing tube is removed when you're able to breathe without it.
Nontraditional coronary artery bypass grafting
Nontraditional CABG includes off-pump CABG and minimally invasive CABG.
Off-pump coronary artery bypass grafting
This type of surgery can be used to bypass any of the coronary arteries. Off-pump CABG also is called beating heart bypass grafting because the heart isn't stopped and a heart-lung machine isn't used. Instead, the part of the heart where grafting is being done is steadied with a mechanical device.
Off-pump CABG may reduce complications that can occur when a heart-lung machine is used, especially in people who have had a stroke or "mini-strokes" in the past, who are over age 70, and who have diabetes, lung disease, or kidney disease.
Other advantages of this type of bypass surgery include:
Minimally invasive direct coronary artery bypass grafting
There are several types of minimally invasive direct coronary artery bypass (MIDCAB) grafting. These types of surgery differ from traditional bypass surgery because they only require small incisions rather than opening the chest bone to get to the heart. These procedures sometimes use a heart-lung machine.
MIDCAB procedure. This procedure is used when only one or two coronary arteries need to be bypassed. A series of small incisions is made between your ribs on the left side of your chest, directly over the artery to be bypassed. The incisions are usually about 3 inches long. (The incisions made in traditional CABG are at least 6 to 8 inches long.) The left internal mammary artery is most often used for the graft. A heart-lung machine isn't used during this procedure.
Port-access coronary artery bypass procedure. This procedure is performed through small incisions (ports) made in your chest. Artery or vein grafts are used. The heart-lung machine is used during this procedure.
Robot-assisted technique. This type of procedure allows for even smaller, keyhole-sized incisions. A small video camera is inserted in one incision to show the heart, while the surgeon uses remotely controlled surgical instruments to perform the surgery. The heart-lung machine is sometimes used during this procedure.
Advantages of minimally invasive CABG include smaller incisions, smaller scars, shorter recovery and hospital stay, less bleeding, less chance for infection, and less pain.
After coronary artery bypass grafting
Recovery in the hospital
After surgery, you will typically spend 1 or 2 days in an intensive care unit. Your heart rate and blood pressure will be continuously monitored during this time. Intravenous medicines (medicines injected through a vein) are often given to regulate blood circulation and blood pressure. You will then be moved to a less intensive care area of the hospital for 3 to 5 days before going home.
Recovery at home
Your doctor will give you specific instructions for recovering at home, especially concerning:
You may also receive instructions on how to deal with common after-effects from surgery. After-effects often go away within 4 to 6 weeks after surgery, but may include:
Full recovery from traditional CABG may take 6 to 12 weeks or more. Less recovery time is needed for nontraditional CABG.
Your doctor will provide instructions on resuming physical activity. This varies from person to person, but there are some typical timeframes. Most people can resume sexual activity within about 4 weeks and driving after 3 to 8 weeks.
Returning to work after 6 weeks is common unless the job involves specific and demanding physical activity. Some people may need to find less physically demanding types of work or work a reduced schedule at first.
Ongoing care
Care after surgery may include periodic checkups with doctors. During these visits, tests may be done to see how the heart is working. Tests may include EKG, stress testing, and echocardiogram.
CABG is not a cure for coronary artery disease (CAD). You and your doctor may develop a management plan that includes lifestyle changes to help you stay healthy and reduce the chances of CAD getting worse. Lifestyle changes may include quitting smoking, making changes in your diet, getting regular exercise, and lowering and managing stress.
In some cases, your doctor may refer you to a cardiac rehabilitation (rehab) program. These programs can help you recover through supervised physical activity and education on how to make choices that reduce your risk for future heart problems and help you get back to your regular lifestyle after surgery.
Doctors supervise these programs, which include counseling about lifestyle changes as well as exercise training to build strength and energy. Cardiac rehab programs may be offered in hospitals and other community facilities. Ask your doctor whether you're a candidate for cardiac rehab.
Taking medicines as prescribed also is an important part of care after surgery. Medicines may be prescribed to manage pain during recovery; lower cholesterol, blood pressure, and the chance of developing blood clots; manage diabetes; or treat depression.
Risks
Although complications from coronary artery bypass grafting (CABG) are uncommon, the risks include:
Some patients can develop a fever associated with chest pain, irritability, and decreased appetite. This is due to inflammation involving the lung and heart sac, and is sometimes seen 1 to 6 weeks after surgeries that involve cutting through the pericardium (the outer covering of the heart). This reaction is usually a mild, self-limited illness, but some patients may develop fluid buildup around the heart that requires treatment.
Use of the heart-lung machine also can cause complications. Memory loss and other changes, such as difficulty concentrating or thinking clearly, may occur in some people. These changes are more likely to occur in people who are older, who have high blood pressure or lung disease, or who drink excessive amounts of alcohol. These side effects often improve several months after surgery.
The heart-lung machine also increases the risk of blood clots forming in your blood vessels. Clots can travel to the brain or other parts of the body and block the flow of blood, which can cause stroke or other problems. Recent technical improvements in heart-lung machines are helping to reduce the risk of blood clots forming.
In general, the chances of developing complications are higher when CABG is done in an emergency situation (for example, if performed during a heart attack), if you're over age 70, or if you have a history of smoking. Your risks also are higher if you have other diseases or conditions such as diabetes, kidney disease, lung disease, or peripheral vascular disease.


