liver cancer
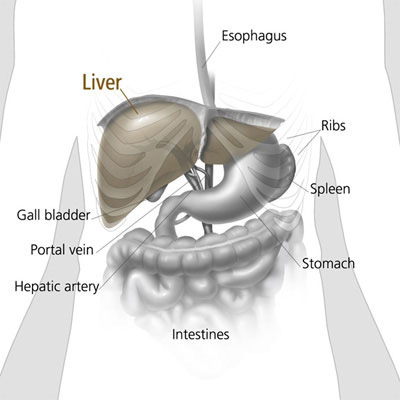
The liver and nearby organs.
Cancer that begins in the liver is called primary liver cancer and is not common in the West. However, it is common for cancer to spread to the liver from the colon, lungs, breasts, or other parts of the body. When this happens, the disease is not liver cancer. The cancer in the liver is a secondary cancer. It is named for the organ or the tissue in which it began.
Most primary liver cancers begin in hepatocytes (liver cells). This type of cancer is called hepatocellular carcinoma or malignant hepatoma.
Children may develop childhood hepatocellular carcinoma or hepatoblastoma. This article does not deal with childhood liver cancer.
When liver cancer spreads (metastasizes) outside the liver, the cancer cells tend to spread to nearby lymph nodes and to the bones and lungs. When this happens, the new tumor has the same kind of abnormal cells as the primary tumor in the liver. For example, if liver cancer spreads to the bones, the cancer cells in the bones are actually liver cancer cells. The disease is metastatic liver cancer, not bone cancer. It is treated as liver cancer, not bone cancer.
Similarly, cancer that spreads to the liver from another part of the body is different from primary liver cancer. The cancer cells in the liver are like the cells in the original tumor. When cancer cells spread to the liver from another organ (such as the colon, lung, or breast), doctors may call the tumor in the liver a secondary tumor. In the United States, secondary tumors in the liver are far more common than primary tumors.
The liver
The liver is the largest organ in the body. It is found behind the rib-cage on the right side of the abdomen. The liver has two parts, a right lobe and a smaller left lobe.
The liver has many important functions that keep a person healthy. It removes harmful material from the blood. It makes enzymes and bile that help digest food. It also converts food into substances needed for life and growth.
The liver gets its supply of blood from two vessels. Most of its blood comes from the hepatic portal vein. The rest comes from the hepatic artery.
Who is at risk?
Researchers in hospitals and medical centers around the world are working to learn more about what causes liver cancer. At this time, no one knows its exact causes. However, scientists have found that people with certain risk factors are more likely than others to develop liver cancer. A risk factor is anything that increases a person's chance of developing a disease.
Studies have shown the following risk factors:
These infections may not cause symptoms, but blood tests can show whether either virus is present. If so, the doctor may suggest treatment. Also, the doctor may discuss ways of avoiding infecting other people.
In people who are not already infected with hepatitis B virus, hepatitis B vaccine can prevent chronic hepatitis B infection and can protect against liver cancer. Researchers are now working to develop a vaccine to prevent hepatitis C infection.
The more risk factors a person has, the greater the chance that liver cancer will develop. However, many people with known risk factors for liver cancer do not develop the disease. People who think they may be at risk for liver cancer should discuss this concern with their doctor. The doctor may plan a schedule for checkups.
Signs and symptoms
Liver cancer is sometimes called a silent disease because in an early stage it often does not cause symptoms. But, as the cancer grows, symptoms may include:
These symptoms are not sure signs of liver cancer. Other liver diseases and other health problems can also cause these symptoms. Anyone with these symptoms should see a doctor as soon as possible. Only a doctor can diagnose and treat the problem.
Diagnosis
If a patient has symptoms that suggest liver cancer, the doctor performs one or more of the following procedures:
Staging
If liver cancer is diagnosed, the doctor needs to know the stage, or extent, of the disease to plan the best treatment. Staging is an attempt to find out the size of the tumor, whether the disease has spread, and if so, to what parts of the body. Careful staging shows whether the tumor can be removed with surgery. This is very important because most liver cancers cannot be removed with surgery.
The doctor may determine the stage of liver cancer at the time of diagnosis, or the patient may need more tests. These tests may include imaging tests, such as a CT scan, MRI, angiogram, or ultrasound. Imaging tests can help the doctor find out whether the liver cancer has spread. The doctor also may use a laparoscope to look directly at the liver and nearby organs.


