vasculitis
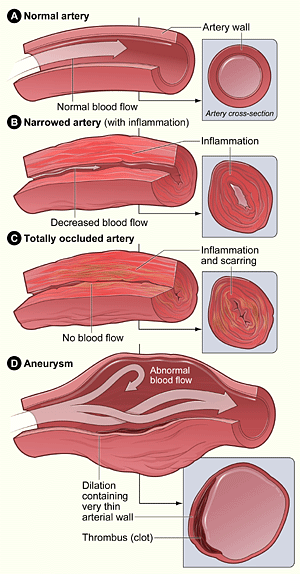
Fig A shows a normal artery with normal blood flow (the inset image shows a cross-section of the normal artery). Fig B shows an artery narrowed due to inflammation in the arterial wall, causing decreased blood flow (the inset image shows a cross-section of the inflamed artery). Fig C shows a totally occluded (blocked) artery due to inflammation and scarring in the arterial wall (the inset image shows a cross-section of the block artery). Fig D shows an artery containing an aneurysm.
Vasculitis is an inflammation of the blood vessels in the body. In vasculitis, the body's immune system mistakenly attacks the body's own blood vessels, causing them to become inflamed. Inflammation can damage the blood vessels and lead to a number of serious complications.
Vasculitis can affect any of the body's blood vessels. These include arteries, veins, and capillaries. Arteries are vessels that carry blood from the heart to the body's organs, veins are the vessels that carry blood back to the heart, and capillaries are the tiny blood vessels that connect the small arteries and veins.
When a blood vessel becomes inflamed, it can:
The disruption in blood flow from inflammation can damage the body's organs. Specific signs and symptoms depend on which organ has been damaged and the extent of the damage. Typical signs and symptoms of inflammation (fever, swelling, and a general sense of feeling ill) are common among people with vasculitis.
Outlook
The outlook for people who have vasculitis varies depending on both the type and severity of the vasculitis. The course of a case of vasculitis can be hard to predict. Treatment is often very effective if vasculitis is diagnosed and treated early. Vasculitis may disappear or go into a period of remission. In some cases, it may be a chronic problem, requiring ongoing treatment, or it may come back ("flare") after a period of remission. In more severe cases, treatment may not help, and vasculitis can lead to disability or even death.
Much is still unknown about vasculitis. There are many different types of vasculitis, but overall it is a fairly rare condition in the general population. Additional research is needed to learn more about the various types of vasculitis and their causes, treatments, and remission patterns.
Types of vasculitis
There are many different disorders that are classified as types of vasculitis. Although all of these disorders include inflammation of the blood vessels, most differ from each other in terms of what populations of people and which organs they affect.
Behcet's disease
Behcet's disease can affect any part of the body because it can occur in vessels of any size or type. Commonly affected organs include the eyes, the mouth, and the genitals. Patients with this type of vasculitis are often younger than those with other types, many times in their twenties and thirties. The HLA-B51 gene allele is often associated with Behcet's disease, but not everyone with the gene will develop the disease. Behcet's is more common in individuals of Mediterranean, Middle Eastern, or Far Eastern descent, but is usually not found in Blacks.
Buerger's disease
Buerger's disease typically affects blood flow to the hands and feet. Buerger's disease is also known as thromboangiitis obliterans and is more likely to occur in smokers than nonsmokers.
Central nervous system vasculitis
Central nervous system vasculitis affects the brain and sometimes the spinal cord.
Churg-Strauss syndrome
Churg-Strauss syndrome can affect many different organs, but it most commonly affects the lungs, skin, kidneys, and heart. Many people who are diagnosed with Churg-Strauss syndrome also have asthma. They may have had preexisting, newly diagnosed, or recently worsened asthma when diagnosed with Churg-Strauss syndrome.
Cryoglobulinemia
Common signs and symptoms of cryoglobulinemia are a rash on the lower limbs, arthritis, and nerve damage. Type 1 cryoglobulinemia is often associated with lymphoma, while Type 2 cryoglobulinemia is often associated with hepatitis C infection.
Giant cell arteritis
Common symptoms of giant cell arteritis include headache, fever, blurred vision, and pain in the jaw, shoulders, or hips. It is the most common form of vasculitis that occurs in adults older than 50 years. It is more likely to occur in people of Scandinavian origin, but can occur in people of any race.
Henoch-Schonlein purpura
Henoch-Schonlein purpura most commonly affects the skin, kidneys, joints, and stomach. It is the most common form of vasculitis found in children, but can occur at any age. When seen in children, it often follows an upper respiratory infection. It is not usually a chronic disease, and full recovery is common.
Microscopic polyangiitis
Microscopic polyangiitis most commonly affects the kidneys, skin, and nerves, but it can affect any organ in the body.
Polyarteritis nodosa
Polyarteritis nodosa most commonly affects the kidneys, skin, and nerves, but it can affect any organ in the body. It is most common in people in their thirties and forties. Men are twice as likely as women to get polyarteritis nodosa. In some cases, it is associated with chronic hepatitis B infection or a very specific type of leukemia known as hairy cell leukemia.
Polymyalgia rheumatica
Polymyalgia rheumatica most commonly affects the large joints in the body, such as the shoulders and hips. It often occurs along with giant cell arteritis.
Rheumatoid vasculitis
Rheumatoid vasculitis can affect many different organs, including the eyes, skin, hands, and feet. It commonly occurs in patients who have severe rheumatoid arthritis.
Takayasu's arteritis
Takayasu arteritis affects the aorta (the largest blood vessel in the body) and its branches, which carry blood away from the heart. It typically occurs in Asian women younger than 40.
Wegener's granulomatosis
Wegener's granulomatosis can occur anywhere in the body. It most commonly affects the upper respiratory tract (nose, sinuses, and throat), lungs, and kidneys. It is most common in people who are middle-aged and older.
Causes
Vasculitis is an inflammation of the blood vessels, but what causes the inflammation is often unknown. It is sometimes a side effect of the body's immune system response to a recent or chronic infection. It also can be a side effect of the body's response to a medicine. The body sometimes recognizes a medicine as a foreign substance, and may develop an "allergic reaction" to try to get rid of it.
Vasculitis is sometimes linked to other diseases, such as:
Who is at risk?
Vasculitis can affect anyone, including men, women, and people of all ages. Some types of vasculitis are more likely to affect certain populations than others. Examples of populations that might be more affected by certain types of vasculitis include smokers, children, young women, middle-aged adults, and people with chronic hepatitis B and/or C infections.
Signs and symptoms
Vasculitis can have many different signs and symptoms depending on the type of vasculitis and which organs are involved as well as how severely they are affected. With vasculitis, any number of organs may be involved, so a patient can experience very few signs and symptoms or may be very sick.
There are two types of signs and symptoms that are common among people with vasculitis: those that affect the body in a general way (systemic) and those that affect specific organs or body systems.
Systemic
Systemic signs and symptoms are not specific to a particular part of the body, but affect a person overall, causing general aches, pains, and sickness. Common systemic symptoms include:
Organ- or body system-specific
These signs and symptoms are specific to a particular organ or body system. The organs and body systems that can be affected include:
Diagnosis
The diagnosis of vasculitis is based on a person's medical history, physical exam, signs and symptoms, and laboratory tests.
Specialists involved
A person with vasculitis may be referred to various specialists, including:
Diagnostic tests and procedures
A variety of tests are used to diagnose vasculitis. The type of test chosen will depend on the signs and symptoms a person has. Some of the tests used in the diagnosis of vasculitis include:
Treatment
Most cases of vasculitis are treated with prescription medicines.
Goals of treatment
The main goal of treatment is to stop the inflammation in the affected blood vessels. Most treatments do this by stopping the immune or inflammatory response that caused the vasculitis to occur.
Specific types of treatment
There are two types of prescription medicines that are typically used to treat vasculitis: corticosteroid medicines and cytotoxic medicines.
Corticosteroid medicines
Corticosteroid medicines are often called steroids, though these are not the same kind of steroids that athletes have been reported to use. These medicines are used to reduce the inflammation in the blood vessels. Examples of corticosteroids that the doctor might prescribe include prednisone, prednisolone, and methylprednisolone.
Cytotoxic medicines
Cytotoxic medicines are typically used to treat cancer, but certain drugs also can be used to treat vasculitis. They may be prescribed in severe cases or in cases in which the patient did not respond to corticosteroids. Sometimes, they are prescribed along with corticosteroids. Cytotoxic medicines work by killing the cells that have caused the inflammation. Examples of these medicines include azathioprine and cyclophosphamide. Doses used for vasculitis are usually lower than those used to treat cancer.
Prevention
There is currently no known way to prevent vasculitis, but with treatment, the complications of vasculitis can be prevented or delayed.
Llving with vasculitis
General information about outcomes
The course of vasculitis is unpredictable and depends on the type and severity of the disease. Vasculitis may:
Ongoing health care needs
The medicines used to treat vasculitis can have significant side effects. Your doctor may adjust the type or dose of medicine you take to lessen the side effects.
In cases in which remission occurs, the doctor may carefully withdraw medicines but still require careful monitoring of flares. Patients who continue taking medicines should stay under the careful watch of their doctor to monitor and control side effects. Patients also should always monitor their health, side effects, and symptoms and discuss any changes with their doctor.


